More Americans Will Take Drugs by Injection or Infusion
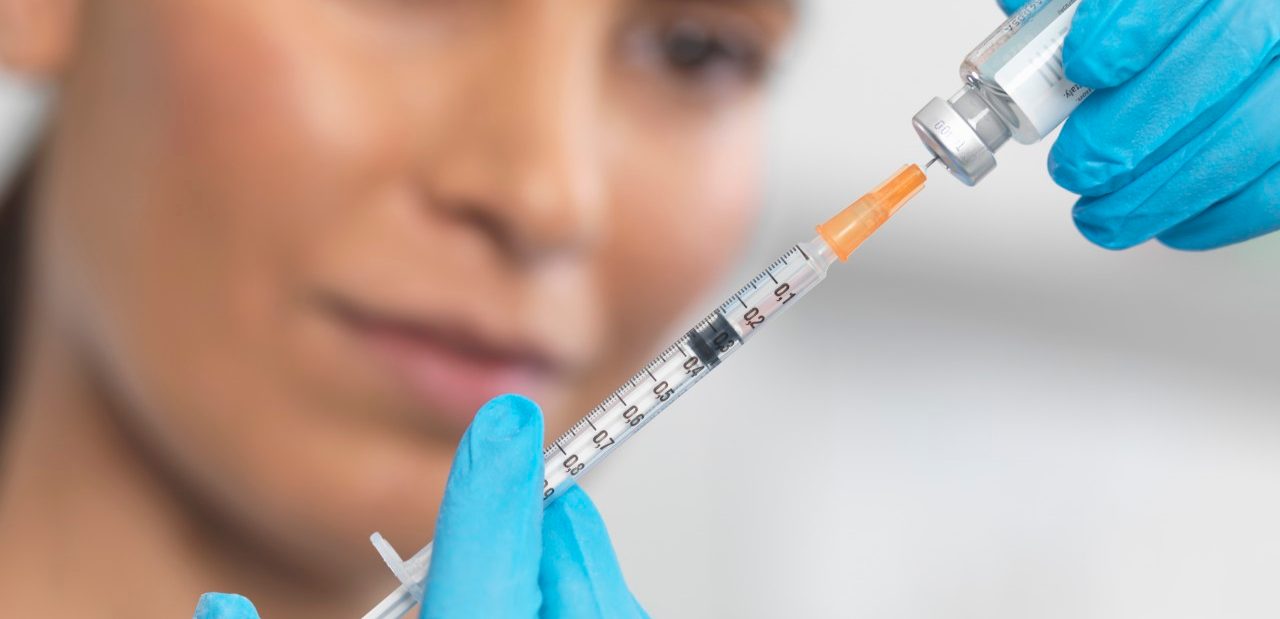
As we age, we’re more likely to develop chronic conditions. And the pricey category of “specialty medications” is growing fast to treat them. Learn more.
After a week of swollen, stiff hands, one morning you wake up from a dream about a great aunt. You recall trying hard not to stare at her gnarly hands. As a child, you didn’t even ask — you knew she was a witch.
When you hear your diagnosis, rheumatoid arthritis, you’ll also hear that treatment is much more successful than in your aunt’s day. The autoimmune illness, which destroys your joints, affects more than a million Americans.
In the 1990s, about one in five people newly diagnosed with rheumatoid arthritis ended up retiring within two years. Now, a new class of drugs called biologics can keep your fingers from gnarling up. The copays are substantial, and you’ll need infusions by IV. But patients seize the chance to keep their hands useful.
YOU MIGHT ALSO LIKE: Drug Interactions with Alcohol
About 4 million Americans turn 65 each year, and they can expect to survive another two decades. As we age, we’re more likely to develop chronic, often painful, diseases like rheumatoid arthritis and cancer.
The drug industry has responded with a flood of products that tend to require injections or infusions by IV. The U.S. Food and Drug Administration (FDA) approve several “specialty medications” each year, accounting for about half of all new approvals. Remicade, Enbrel, and Humira, the top sellers, treat rheumatoid arthritis and other autoimmune diseases like psoriasis.
Specialty medications can be life-savers — and a huge burden. You might have to endure two-hour sessions hooked up to an IV, or weekly injections. If you travel, you might need to carry your medication in a cooler.
But the biggest burden is financial. More than half a million Americans incur yearly medication costs of more than $50,000, facing co-pays of up to 33 percent, though, on newer drugs, manufacturers may provide assistance.
More Americans will be facing those choices as they age, as specialty medications arrive for increasingly common conditions like heart disease and obesity. About a third of American adults have high cholesterol.
In 2015, the first injectable drug to lower cholesterol, alirocumab (Praulent), won FDA approval to treat people with a history of heart disease or stroke or an inherited kind of high cholesterol. The injection is intended to boost the effectiveness of statins for people whose cholesterol levels don’t fall enough with the statin alone. It’s common for drugs to first win approval for a relatively small group, and then win approval for ever-bigger populations.
About two thirds of Americans are overweight or obese. Several diabetes drugs have become available for weight problems..
Clinics are offering infusions by IV with ketamine, prescribed off-label for suicidal thinking. Suicide is the ninth leading cause of death in the United States for people between the ages of 10 and 64.
So far, about half of the current spending on specialty medications goes to inflammatory illnesses (like rheumatoid arthritis and psoriasis), multiple sclerosis, and cancer. The other half goes to treatments for hepatitis C, HIV, growth deficiency in children, cystic fibrosis, pulmonary hypertension, and sleep disorders.
In the debate over who will pay for pricy medications, remember that no one would go to all this trouble if the drug didn’t meet a significant need. HIV drugs extend the life expectancy of someone with an HIV infection. And drugs for rheumatoid arthritis are allowing people to drive and use keyboards. How much is that worth?
YOU MIGHT ALSO LIKE: FDA-Approved Drugs May Not Be as Safe as You Think
Updated:
June 22, 2023
Reviewed By:
Janet O’Dell, RN