What Is Psoriasis?
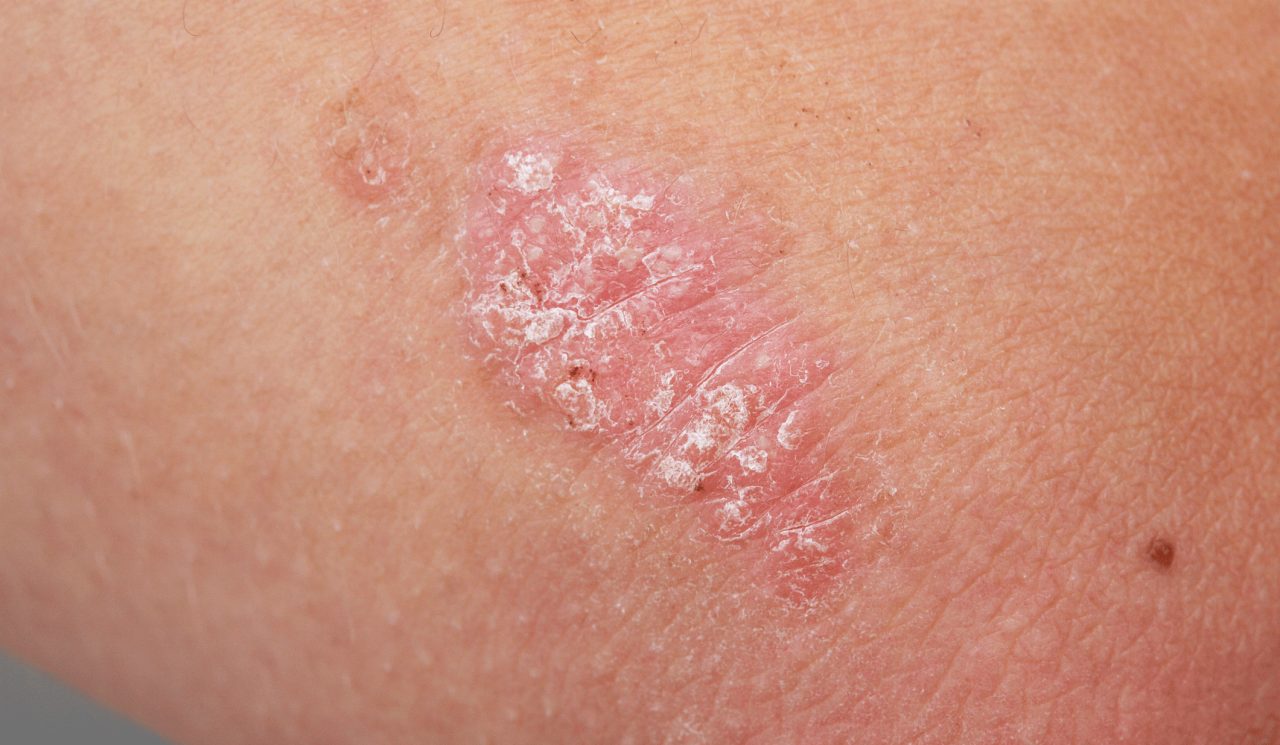
Talk to your doctor if you see white scales on your skin, often on your elbows or knees. The scales can mean you have psoriasis.
What is psoriasis?
The most common kind is plaque psoriasis. Your skin cells accumulate up to 10 times faster than normal because of an error in your immune system.
Psoriasis affects up to 11 percent of caucasians. On this kind of skin, you’ll notice raised, red patches covered with dead skin cells that look like silver or white scales.
Less often, it affects people with darker skin. The areas may look purple or gray or be thicker than surrounding skin. Sometimes the patches crack and bleed.
Although psoriasis can appear anywhere on your skin, it’s most likely on your scalp, knees, elbows, and torso. You’ll usually see it on both sides of your body. It tends to flare up for a few weeks or months, then subside for a while.
YOU MIGHT ALSO LIKE: Treating Psoriasis May Help You Avoid Dementia
Other types of psoriasis
In nail psoriasis, your nails become discolored and pitted and may crumble off.
About a third of all people with psoriasis also develop psoriatic arthritis, when your joints become stiff and swell, often in the morning.
Guttate psoriasis primarily affects young adults and children, typically after a case of strep throat. The lesions are small, shaped like drops.
Inverse psoriasis may affect the skin folds of your groin, buttocks, and breasts, often after fungal infections.
There are two other rare forms called pustular psoriasis (causing pus filled welts) and erythrodermic psoriasis (marked by a red painful peeling rash).
See photos showing the differences here.
What causes psoriasis?
A genetic vulnerability combined with a trigger in your life sets off inflammation when your immune system incorrectly acts as if you are in danger, even though you are not.
Possible triggers include chronic infections, drinking too much alcohol, low humidity, medications (beta-blockers and lithium), smoking, obesity, and stress.
People with psoriasis are more likely to have high cholesterol, high blood pressure, type 2 diabetes, or heart disease. Psoriasis may increase your risk for heart attack or stroke, even in mild cases. People with the skin condition are also more likely to be anxious or depressed.
How do you treat plaque psoriasis?
Doctors advise starting with the mildest treatment, depending on your type of psoriasis and how much of your body it covers.
The most frequently prescribed medications are corticosteroids, available as ointments, creams, lotions, gels, foams, sprays, and shampoos. You might apply the medicine once a day during flares and on alternate days or weekends only when you don’t have symptoms.
Corticosteroids, however, can stop working over time. If that happens, you can try vitamin D, which slows the growth of skin cells, or retinoids, calcineurin inhibitors, salicylic acid, or coal tar (for your scalp).
You can use light therapy alone or with other medications. You’ll need repeat treatments, but you might be able to do them at home. You might even rely on sunlight, on a schedule, avoiding the peak hours of 10 a.m. to 2 p.m.
In a treatment known as PUVA, you take a light-sensitizing drug called psoralem before exposure to UVA light. But there are both short-term and long-term side effects.
Oral drugs can suppress your immune system.
Losing weight and exercise can help as well.
If no treatment helps and your case is moderate to severe, you might try medications called biologics (made from genetically engineered living cells). They require an IV infusion or injection, although you can sometimes do the injection at home.
Biologics include:
- Secukinumab (Cosentyx)
- Adalimumab (Humira)
- Etanercept (Enbrel)
- Infliximab (Remicade)
- Ustekinumab (Stelara)
- Ixekizumab (Taltz)
- Tildrakizumab (Ilumya)
- Apremilast (Otezla)
These drugs are expensive, and insurance doesn't always cover the cost. They may also have side effects.
A newer drug, bimekizumab, made the condition go away completely for 67 percent of patients after 48 weeks of treatment, compared with 46 percent of patients receiving secukinumab.
Other drugs biologics block the pro-inflammatory biochemical, IL-17A, the most potent form of interleukin-17, which helps your immune system fight inflammation. Bimekizumab blocks that chemical plus IL-17F, a similar chemical that is more abundant in your body.
In another clinical trial, after 16 weeks, 86 percent of patients on bimekizumab had a 90 percent reduction in their psoriasis, compared to 47 percent of those taking adalimumab. Bimekizumab also treats psoriatic arthritis.
The downside: In the 48-week study, nearly 20 percent of the volunteers got thrush, a yeast infection in the mouth, which was treated with a common anti-fungal drug. The volunteers also experienced diarrhea. More seriously, it’s possible that, like other drugs that block interleukin-17, it may increase the risk of other infections and cancer.
Updated:
July 12, 2023
Reviewed By:
Janet O’Dell, RN