Painkiller Overdoses Tax the Healthcare System
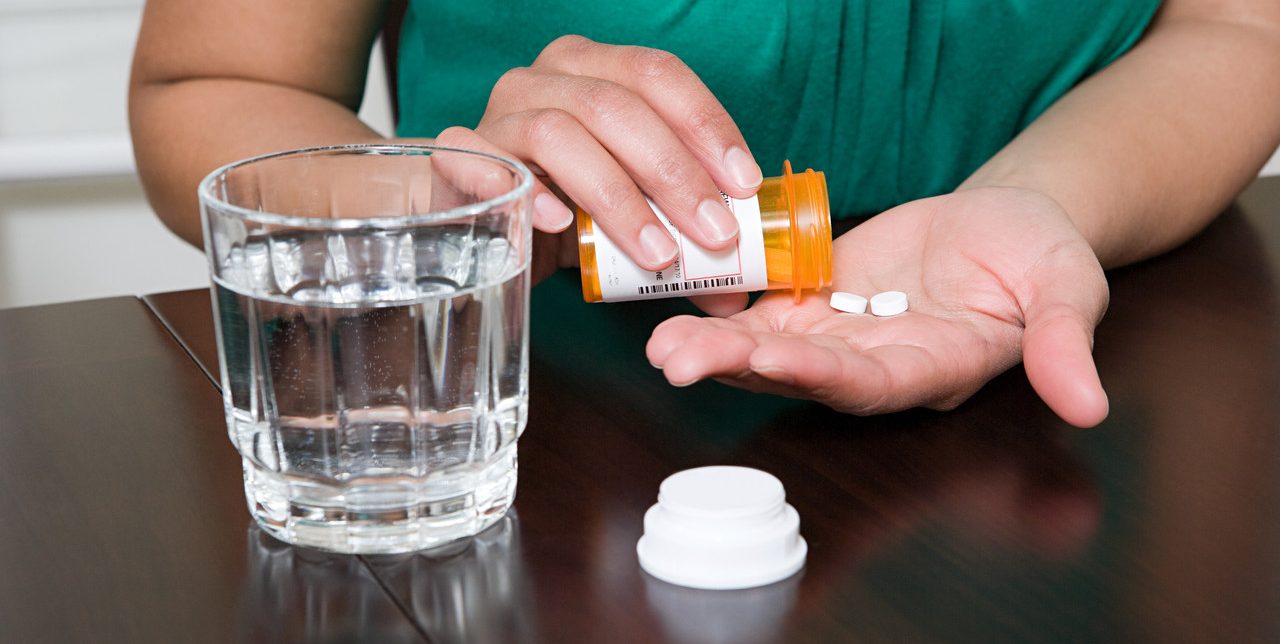
The epidemic of opioid misuse and abuse has not only resulted in personal tragedies but also taken a toll on the country’s healthcare system.
A movie star at 28, Heath Ledger appeared to have it all. He had just completed his role as the Joker in The Dark Knight, at the time the latest Batman movie, when, in February of 2008, he was found lifeless in his New York apartment. The medical examiner ruled Ledger died of "acute intoxication" from prescription drugs, including multiple narcotic painkillers known as opioids.
His death, ruled an accidental, tragic overdose, stunned the public. It seemed a senseless and preventable way to die. But in the years following Ledger’s death, opioid overdose deaths became an increasingly common occurrence.
There were more shocking headlines about other celebrities, including, Prince and Tom Petty, dying from accidental opioid overdoses. They had simply shared the all-too-common fate of thousands of other people who were dying every year from opioids.
In spring of 2022, data from the National Center for Health Statistics, of the Centers for Disease Control and Prevention (CDC), revealed about 105,732 Americans had died of drug overdoses since fall of 2021 — an unprecedented surge. And there were more opioid overdose deaths than ever. About two-thirds of those fatalities involved synthetic opioids like fentanyl, a stronger, faster-acting, and more deadly drug than natural opiates. Countless others who survived opioid overdoses ended up in emergency rooms.
Bottom line: The epidemic of opioid misuse and abuse has not only resulted in personal tragedies but also taken a toll on the country’s healthcare system.
YOU MIGHT ALSO LIKE: Killer Opioid Drugs
The opioid epidemic
Opioid overdose, which includes prescription pain medications such as hydrocodone, oxycodone (OxyContin), and the combination drug acetaminophen and hydrocodone (Vicodin), is a national epidemic, according to the CDC. In fact, it’s now the leading cause of accidental death for adults in the U.S.
In addition to the personal suffering they cause, opioid overdoses place a substantial burden on the country’s often crowded emergency departments (EDs) and hospitals, according to researchers from Stanford University, the University of Pennsylvania, Brown University, and Rush Medical College. Their analysis of data from EDs across the U.S., published in the journal JAMA Internal Medicine, found that prescription opioids were involved in almost 70 percent of ED visits for drug overdoses (over 135,971) in 2010.
The overall death rate was low, less than 2 percent, for those treated for opioid overdoses in EDs. About half of the people were so seriously ill, however, that they were admitted to hospitals. The resulting price tag for both ED and hospital care due to opioid overdoses is staggering — nearly $2.3 billion a year.
"Opioid overdose takes a significant toll on the healthcare system in the United States, both in terms of finances and resources," said Traci Green, an epidemiologist at the Department of Emergency Medicine at Rhode Island Hospital and a senior researcher on the study.
ED overdose victims often had several health conditions, including chronic respiratory diseases and mental health problems, and were taking other drugs in addition to pain relievers. Although deaths recorded for overdoses typically involved multiple opioids, tranquilizers in the benzodiazepine family (such as Xanax and Klonopin) were frequently part of the deadly mix.
“Acute benzodiazepine intoxication was recorded in 22.2 percent of all overdose patients. That shows a need for healthcare providers to exercise caution when prescribing opioids to patients in conjunction with other sedating medications," Stanford researcher Michael Yokell, who headed the study, pointed out.
Most of the time, opioid overdoses are unintentional, according to Barbara J. Turner, MD, professor of medicine at the University of Texas Health Science Center at San Antonio and director of the Center for Research to Advance Community Health. "People with chronic pain don't mean to end their lives," she said. "But they're taking a lot of drugs with substantial risks."
Turner and her colleague, Yuanyuan Liang, PhD, developed a database to analyze the healthcare and medication records of more than 200,000 HMO-enrolled patients who filled at least two prescriptions for opioid drugs to treat non-cancer pain between 2009 and 2012. Their research, published in The Journal of Pain, showed that the more potent opioid doses increased the risk of overdose, as expected — but even moderate doses of the drugs taken for more than four to six months produced almost the same risk as someone taking a high daily dose.
Another study by the duo, published in The Journal of General Internal Medicine, found a substantial overdose risk for patients with mental health disorders who were prescribed opioids along with sedatives and antidepressants — the same mixture that killed Heath Ledger.
How to address the problem
What’s the answer to the opioid overdose epidemic? According to Turner and Liang, doctors and their patients need to use common sense, non-medication approaches to alleviate chronic pain whenever possible.
(See the National Institute on Drug Abuse for more information on opioid abuse.)
The National Institutes of Health (NIH) has released a review of opioid use, published in the Annals of Internal Medicine, focusing on the drugs’ dangers and the lack of research into better and safer ways to treat chronic pain.
“The prevalence of chronic pain and the increasing use of opioids have created a ‘silent epidemic’ of distress, disability, and danger to a large percentage of Americans,” the NIH stated. “The overriding question is: Are we, as a nation, approaching management of chronic pain in the best possible manner that maximizes effectiveness and minimizes harm?”
The answer is a resounding “no,” according to the report. The NIH concluded there is insufficient evidence to determine if long-term opioid use for chronic pain is even effective — but there is plenty of evidence it can be harmful, including the thousands of annual ED visits for overdoses.
In the meantime, several U.S. companies involved in the production and distribution of prescription opioids agreed in 2022 to pay billions to settle lawsuits brought on by claims the marketing practices of the companies were complicit in the opioid epidemic. Meanwhile, some state laws now mandate how and when doctors can prescribe opioids.
Updated:
April 28, 2022
Reviewed By:
Christopher Nystuen, MD, MBA and Janet O'Dell, RN