People Can Spread Zika Virus in Many Ways
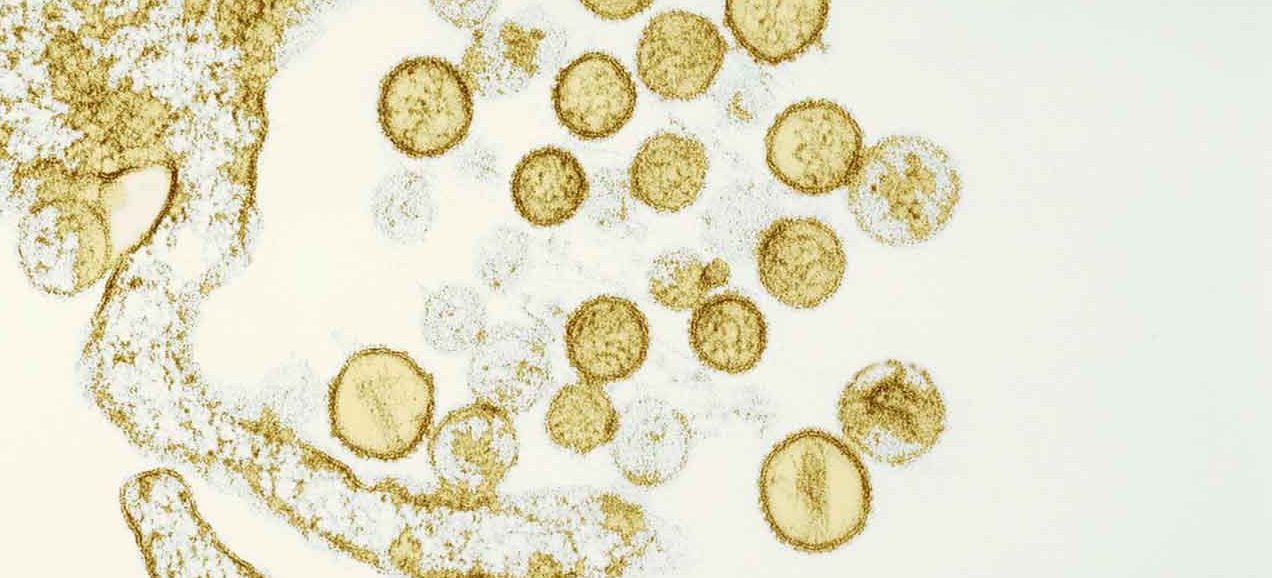
Not only mosquitoes carry Zika – research shows humans can cause transmission, too.
When news of the Zika epidemic first broke, advice about preventing the infection centered around one important strategy: Avoid mosquitoes. After all, Zika is a mosquito-borne virus so finding ways to prevent being bitten by mosquitoes makes sense.
But as cases of the disease increase and continue to spread from South America northward into U.S. territories and states, researchers are learning it’s not just bites from Zika-carrying mosquitoes that result in the infection. Human-to-human Zika virus transmission is now known to be a reality.
YOU MIGHT ALSO LIKE: Your Guide to Zika Virus and Other Mosquito-Borne Illnesses
In fact, while it’s true the virus is still spread primarily by mosquitoes, humans may play a significant role in whether Zika spreads rapidly around the country. Local outbreaks could be sparked by thousands of people who contracted Zika in areas where the virus is active and then returned from a trip or moved to the U.S., most with no idea they are infected, according to Anne Schuchat, MD, the principal deputy director at the Centers for Disease Control and Prevention (CDC).
At a recent panel discussion at the Woodrow Wilson International Center for Scholars, Schuchat, along with National Institute of Allergy and Infectious Diseases Director Anthony Fauci, MD, and other health experts, noted that about 80 percent of people with Zika don’t have symptoms (like rash, joint pain, and conjunctivitis) and are unaware they have the virus. However, if infected persons are simply bitten by mosquitoes, which is not unlikely in the summer months in many areas of the country, the insects then carry the disease and can infect other people. The panel called for anyone returning from areas where Zika virus has been reported to protect themselves from mosquito bites for three weeks to prevent passing Zika to mosquitoes and triggering outbreaks.
Researchers have found that the virus can live in blood for at least several weeks so blood transfusions may be another way human-to-human Zika infection can occur. To reduce this risk of contracting the virus, the Red Cross now asks potential blood donors to delay their blood donation for four weeks if there’s a possibility they’ve been exposed to the virus. Risks include having been in an area with local Zika infections within the past four weeks, being diagnosed with Zika or having two or more symptoms of the virus within two weeks of leaving an area with local transmission, and sexual contact within the past four weeks with a man who has Zika or could have been exposed to the disease.
With tests for Zika virus becoming more available, it might seem reasonable for anyone who could have been exposed to the virus to find out for sure if they are infected. Unfortunately, the CDC has determined the tests can be confusing to interpret – and miss Zika infections. Specifically, a Zika test with the complicated-sounding name “positive real-time reverse transcription-polymerase chain reaction” does confirm Zika virus infection if results are positive; but a negative test result doesn’t mean you aren’t infected.
There are additional tests for Zika antibodies that can help diagnose infection with the virus. But, it turns out, those tests have problems with accuracy, too.
"Zika virus antibody test results can be difficult to interpret because of cross-reactivity with other flaviviruses, which can preclude identification of the specific infecting virus, especially when the person previously was infected with or vaccinated against a related flavivirus,” the latest CDC report explained.
How Zika is passed to babies – before and (possibly) after birth
Doctors in Brazil first noticed a potential link between Zika and the heartbreaking birth defect known as microcephaly (characterized by a smaller than normal head and brain and serious neurological problems). That association, now confirmed by researchers, indicated a pregnant woman with Zika could spread the infection to her unborn child. The CDC and other health agencies warn women who are pregnant or could become pregnant to not only avoid mosquitoes but to also practice abstinence or safer sex with condom use in case a partner is or might be infected with Zika and could potentially pass on the virus.
How a woman infected with Zika can transmit the virus to her unborn baby has puzzled researchers. Other viruses that are related to Zika (flaviviruses), including dengue, West Nile, and yellow fever, are rarely passed from mother to fetus. Most likely, this is because the placenta (the organ that develops in the uterus during pregnancy and provides oxygen and nutrients to the growing baby) separates the circulatory systems of the pregnant mother and the developing baby. So something must be different about the Zika virus that enables it to slip past the protection of the placenta.
Research from Emory University School of Medicine scientists suggests Zika can wreak havoc on a fetal brain because, in a sense, the virus hijacks immune cells in the placenta. It infects and reproduces in these cells without harming them. Then the virus moves on to infect and damage brain cells in a developing fetus.
“Zika may be unique in its ability to infect placental cells and cross the placental barrier, in comparison with other flaviviruses,” said Mehul Suthar, PhD, assistant professor of pediatrics at Emory who headed the study.
YOU MIGHT ALSO LIKE: What Pregnant Women Should Know about the Zika Virus
But not every pregnant woman infected with Zika delivers a child with microcephaly so other factors, still not understood, likely play a role in whether the virus is passed on from mother to unborn baby.
“Host genetics and non-viral factors, including nutrition and microbiota, as well as timing may be influencing infectivity,” Suthar explained. “A better understanding of these factors could allow the design of preventive measures, and eventually antiviral therapies."
If a woman who’s infected with Zika gives birth to a healthy baby – and many do – does that mean the child has escaped health problems from the virus? The bottom line is, researchers simply don’t know yet. Zika is found in urine, blood, and saliva, and some scientists suggest the virus could possibly be transmitted from mother to newborn during birth or with close contact afterwards between baby and mom.
Zika virus has also been found in breastmilk. However, the World Health Organization (WHO) and the CDC still recommend that women with Zika nurse their babies. Based on the evidence so far, WHO says the benefits of breastfeeding for babies and mothers outweigh any potential risk of Zika virus transmission through breast milk.
However, that’s not the final word on the matter. Global health experts from Cornell University are heading an international team of researchers studying the likelihood and potential seriousness of transmitting the Zika virus through breastfeeding. WHO will use the research team’s findings to update guidelines for feeding infants during a Zika outbreak.
In the meanwhile, scientists at the Pasteur Institute who are studying Zika are calling for caution when it comes to mothers with Zika infection or symptoms of the virus nursing their babies. Transmission of other viruses related to Zika are likely transmitted via breastfeeding, and the Pasteur scientists have recently found high viral loads of Zika in breastmilk.
What is known – and not known yet – about sexual transmission of Zika
In recent months, scientists have confirmed Zika is a sexually transmitted disease. And it’s now known the Zika virus can be spread by heterosexual and gay both vaginal and anal sex.
Even if pregnancy is not a possibility for you, it’s still important to take steps to avoid infection if your partner may have Zika. Although most cases of the virus involve fairly mild symptoms, there’s mounting evidence that the infection can lead to more severe health woes in some people. For example, Zika is associated with cases of Guillain-Barre syndrome, which causes neurological problems and can, rarely, paralyze and even be fatal. The virus also has also been linked to MS-type symptoms in several patients.
Based on current knowledge of Zika, abstaining from sex or practicing safer sex with condoms now makes sense for most everyone who is sexually active, especially if you are in an area where the virus has been reported or if your partner has recently visited a place where there is a Zika outbreak.
A man infected with Zika can potentially pass the virus to a partner before symptoms start, while he has symptoms, and even after his symptoms have gone away. For now, testing blood or urine to see if a man is likely to pass the Zika virus on through sex isn’t recommended — a man could test negative and still have the Zika virus in his semen, according to the CDC.
What’s more, researchers don’t know how long the virus stays in semen but it may survive for months, meaning that sexual transmission could be possible long after any Zika infection symptoms have cleared.
There’s now evidence that not only men infected with Zika can pass on the infection to female or male sex partners via vaginal or anal intercourse, but infected women can pass on the virus to their partners, too. In fact, the updated CDC Zika prevention guidelines warn that any sexual activity — including vaginal, anal and oral sex, and the sharing of sex toys — may transmit the virus.
Warnings for healthcare workers
The CDC and the Occupational Safety and Health Administration have issued new guidance and information for protecting people employed in the healthcare field or who work in medical laboratories from possibly contracting Zika while on the job.
Accidental sticks with needles contaminated with Zika can cause infections and should be reported. A University of Pittsburgh researcher who had no other risk factors for the virus recently developed symptoms of Zika eight days after a needle stick. She is complying with a request from the Allegheny County Health Department to wear long sleeves and pants and is wearing insect repellent for several weeks to avoid being bitten by a mosquito that could then spread the disease and cause an outbreak in her area.
Standard infection control precautions are recommended — including wearing gowns, masks, gloves, and eye protection — during the delivery of babies and for any procedures and tests that could result in exposure to body fluids (including blood, saliva, breastmilk, and amniotic fluid).
Washing hands with soap and water or using alcohol-based hand rubs containing at least 60 percent alcohol before and after any contact with a patient, whether or not Zika infection is suspected, is also important. Laboratories must make sure their facilities and practices meet the appropriate Biosafety Level for handling and working with Zika virus, too.
Bottom line
For now, the best way to protect yourself — and others — is to avoid mosquitoes and practice safer sex. And, if there’s any chance at all you could have Zika, no matter how healthy you feel, remember to do everything you can to avoid potentially spreading the virus to others.
YOU MIGHT ALSO LIKE: Does Zika Virus Make a Trip to the Summer Olympics Dangerous?
Updated:
March 31, 2020
Reviewed By:
Christopher Nystuen, MD, MBA