Know Early Melanoma Symptoms
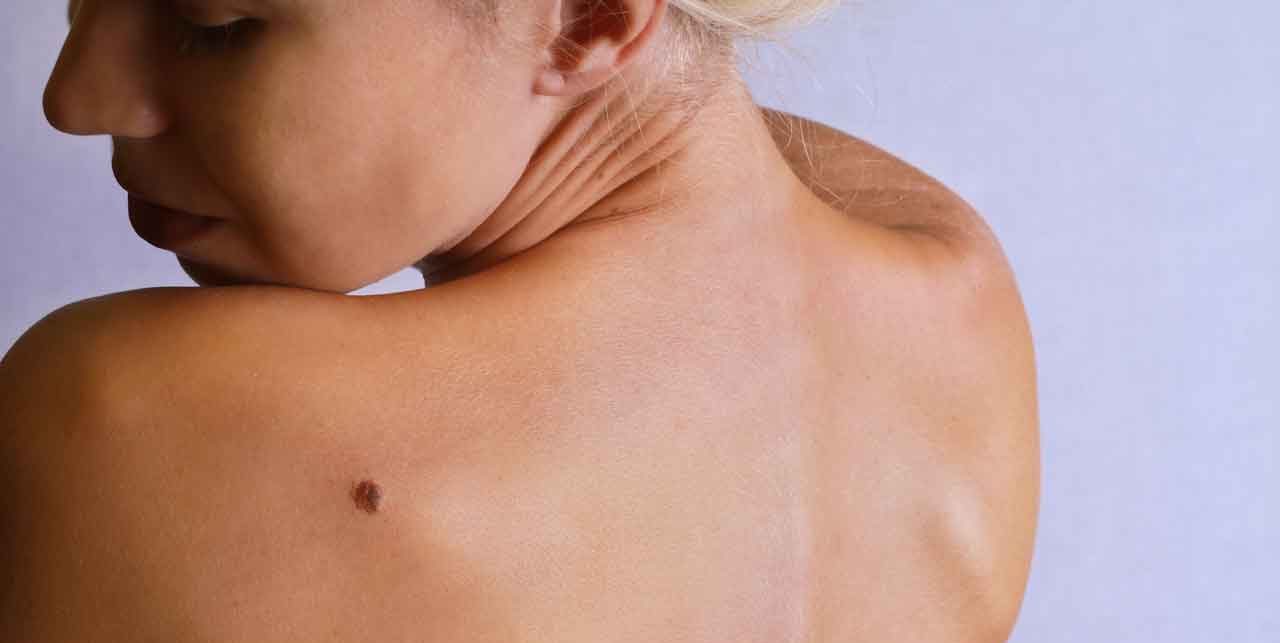
If you know early melanoma symptoms and get treatment, you can save your life — but be aware that treatment delays of only weeks can be fatal.
Melanoma is the most serious form of skin cancer because it can spread to other parts of your body, including your brain. Although melanoma accounts for only about one percent of skin cancers, it causes almost all the deaths from skin cancer. In all, about 87,000 people in the U.S. are diagnosed with melanomas annually. Almost 10,000 of them will die, according to the American Cancer Society.
YOU MIGHT ALSO LIKE: Our Skin Cancer section
While early detection and treatment are the best strategies for all cancers, researchers from the Cleveland Clinic have found spotting and treating melanomas as quickly as possible can make a huge difference in the outcome of melanoma — especially when the disease is caught in stage 1. In fact, even treatment delays of a few weeks to months after diagnosis can have a negative impact on whether a person with melanoma is likely to survive long-term.
The impact of early treatment for melanoma
For their study, published in the Journal of the American Academy of Dermatology, researchers from Cleveland Clinic’s Dermatology and Plastic Surgery Institute analyzed information from the National Cancer Database compiled on 153,218 adult patients who were diagnosed with stage I, II, or III melanoma. The results showed that no matter what the stage of their malignancy, patients with melanoma who waited longer than 90 days for surgery had a lower chance of surviving.
But for those with stage I of the disease, when melanoma is just starting to invade deeper layers of skin, the advantages of early detection and treatment were especially dramatic.
Compared to people who were treated within a month of being diagnosed, melanoma patients with stage I disease were:
- 5 percent more likely to die when treated between 30 and 59 days
- 16 percent more likely to die when treated between 60 and 89 days
- Almost 30 percent more likely to die if treatment was delayed between 91 and 120 days
- Over 40 percent more likely to die if they weren’t treated until after 120 days
"The ideal timing for melanoma treatment, predominantly surgery, had yet to be determined — until now," said researcher Brian Gastman, MD, director of melanoma surgery at Cleveland Clinic.
"Patients and referring physicians are not only concerned with how a melanoma is removed, but also when it's removed. We saw significantly worse prognoses and outcomes for those surgically treated after 30 days of stage I melanoma diagnosis," Gastman explained. “Knowing for certain that a more expedient time to surgery to remove an early melanoma improves the chances of survival is a game-changer in treating this life-threatening skin cancer."
What is melanoma?
Melanocytes are skin cells that produce the brown pigment melanin that gives skin a brown color naturally or from tanning. When your skin is exposed to the sun, melanocytes make more melanin, darkening your skin. This protects the deeper layers of your skin from some of the harmful effects of the sun.
Melanoma is cancer that originates in melanocytes. Most melanoma tumors are black or brown, but some melanomas don’t produce melanin and are tan, pink, or even white.
Melanomas appear anywhere on skin but are more likely to develop on the chest and back in men and on the legs in women. The neck and face are other common areas where melanomas start, but they can also be found on:
- The palms of the hands
- Soles of the feet
- Under the nails
Although more rare than melanoma of the trunk, they can show up in the eyes mouth, genitals, and anal area, according the American Cancer Society.
How do you get melanoma?
Scientists don’t know exactly how you get melanomas, but they’ve documented gene changes inside mole cells that may trigger melanoma. Researchers have linked exposure to UV (ultraviolet) rays from sunlight and tanning beds as the major risk factor for most melanomas — probably because UV rays damage the DNA of genes controlling skin cell growth, the American Cancer Society explains.
Some gene mutations that raise the risk of melanoma are inherited and play a role in why melanomas seem to occur frequently in certain families. But about half of all melanomas have a change in a gene — the BRAF oncogene — which is not inherited. Instead, this gene mutation occurs as skin cancer develops and the altered gene spurs the growth of the melanoma.
The National Cancer Institute (NCI) lists these risk factors for melanoma:
- Having a fair complexion, especially if your skin freckles and burns easily or tans poorly
- Blue or green or other light-colored eyes
- Red or blond hair
- Being exposed to UV light from the sun, tanning booths, or sunlamps over time
- Being exposed to environmental risk factors for melanoma in your environment — including radiation, solvents, vinyl chloride, and PCBs (polychlorinated biphenyls, used widely in paints, dyes, and plastics before the chemicals were banned in l979)
- Having a history of many blistering sunburns, especially as a child or teenager
- Having several large or many small moles
- Having a family history of unusual moles (atypical nevus syndrome)
- Having a personal or family history of melanoma
- Having a weakened immune system
Early melanoma symptoms
Early melanoma symptoms are changes in the shape or size of an existing mole. The American Academy of Dermatology advises contacting your doctor if you notice any of these ABCDE melanoma symptoms:
- Asymmetry: Is one half of a mole different from the other half?
- Border: Do you have a mole with an irregular, scalloped, or poorly defined border?
- Color: Does a mole have more than one color — for example, shades of tan and brown, black, white, red, or blue?
- Diameter: Is a mole larger than the size of a pencil eraser (about 6 mm)? (Although melanomas are usually over 6 mm when diagnosed, they can be smaller.)
- Evolving: Does a mole or another spot on your skin look different from the rest? Have you noticed a mole or another spot changing size, shape, or color?
How is melanoma treated?
If a biopsy shows an abnormal mole or lesion is a melanoma, the tissue sample may also be tested for certain gene changes. Then your doctor will advise a treatment plan based on the stage and location of the cancer, as well as any other health conditions you may have that can impact how melanoma is treated.
The stages of melanoma indicate how far the cancer has spread within skin and whether it has metastasized to other parts of the body, according to the NCI.
In addition to biopsy results, determining the stage of the disease involves:
- A physical exam and blood tests
- A biopsy or other testing of sentinel lymph nodes (the first lymph node or nodes near the melanoma where cancer cells are most likely to have spread)
- Imaging tests such as CT, PET scans, and MRIs to search for any spread of the malignancy
Important factors used to stage a melanoma include:
- The thickness of the tumor
- Whether it has broken through your skin
- If it has spread to lymph glands (and whether this has caused lymph glands to be matted together)
- Signs of the tumor metastasizing to other areas of your body
Staging of melaonma occurs on a scale from 0, the earliest and easiest to treat form of the disease, to the more serious and life-threatening later stages III and IV.
At very early stage 0, melanomas are confined to the epidermis, the top layer of the skin. The cancer is typically removed with surgery along with a small amount of skin around the melanoma. If cancer cells appear at the edges of the biopsied skin, you may need more surgery to make sure all of the cancer cells have been removed.
If an early-stage melanoma is on your face and surgery can cause a disfiguring scar, a doctor may consider using radiation therapy or a topical anti-tumor medication (imiquimod) to treat the cancer. But the American Cancer Society points out that not all doctors agree with this melanoma treatment.
Stage I melanomas are found deeper in the skin than stage 0. Stage II melanomas have spread to the lower part of the inner layer of skin (dermis), but not into the tissue below or into nearby lymph nodes. Stage I and stage II melanomas are treated similarly — with wide excisions to take off the melanoma along with a margin of normal skin.
In some cases, you may receive the drug interferon after surgery. Interferon is a protein produced by normal cells to fight viral infections and disease and is used in large doses to treat melanoma as an immunotherapy.
Stage III melanoma may be any thickness and may have or lack ulceration — but the cancer has usually spread to your lymph glands. Surgical treatment for stage III melanoma usually requires a wide excision to remove the tumor, along with lymph node dissection.
Interferon treatment and radiation therapy to the areas where the lymph nodes were removed may delay the recurrence of stage III melanomas. You may receive chemotherapy to treat stage III melanoma, and it may be combined with immunotherapy.
Stage IV melanomas have a poor prognosis because the cancer has already spread to distant lymph nodes or other parts of your body. Skin tumors or enlarged lymph nodes can be removed by surgery or treated with radiation therapy.
Chemotherapy, usually with the drugs acarbazine (DTIC) and temozolomide (Temodar), may shrink metastasized melanoma cancers but, unfortunately, the malignancies usually start growing again within several months.
Lower your melanoma risks
It's important for your doctors — from family physicians and dermatologists to surgeons and oncologists — to be aware of the danger of melanoma and to provide immediate treatment when cancer is found at stage I.
What’s more, Brian Gastman and colleagues advise patients to be their own health advocates. If you spot a new, changing, or suspicious mole or area of your skin, see a dermatologist ASAP for diagnosis.
If you are diagnosed with melanoma, speak out for prompt treatment and work with your doctor to prevent any delays.
To reduce your risk of melanoma and other types of skin cancers, protect yourself from exposure to harmful ultraviolet radiation from the sun and indoor tanning beds, especially young people.
To protect your skin from the sun:
- Seek shade when you are outside
- Wearing protective clothing
- Use a broad-spectrum, water-resistant sunscreen with an SPF of 30 or higher
Updated:
March 17, 2023
Reviewed By:
Christopher Nystuen, MD, MBA