What Is Radiation Therapy?
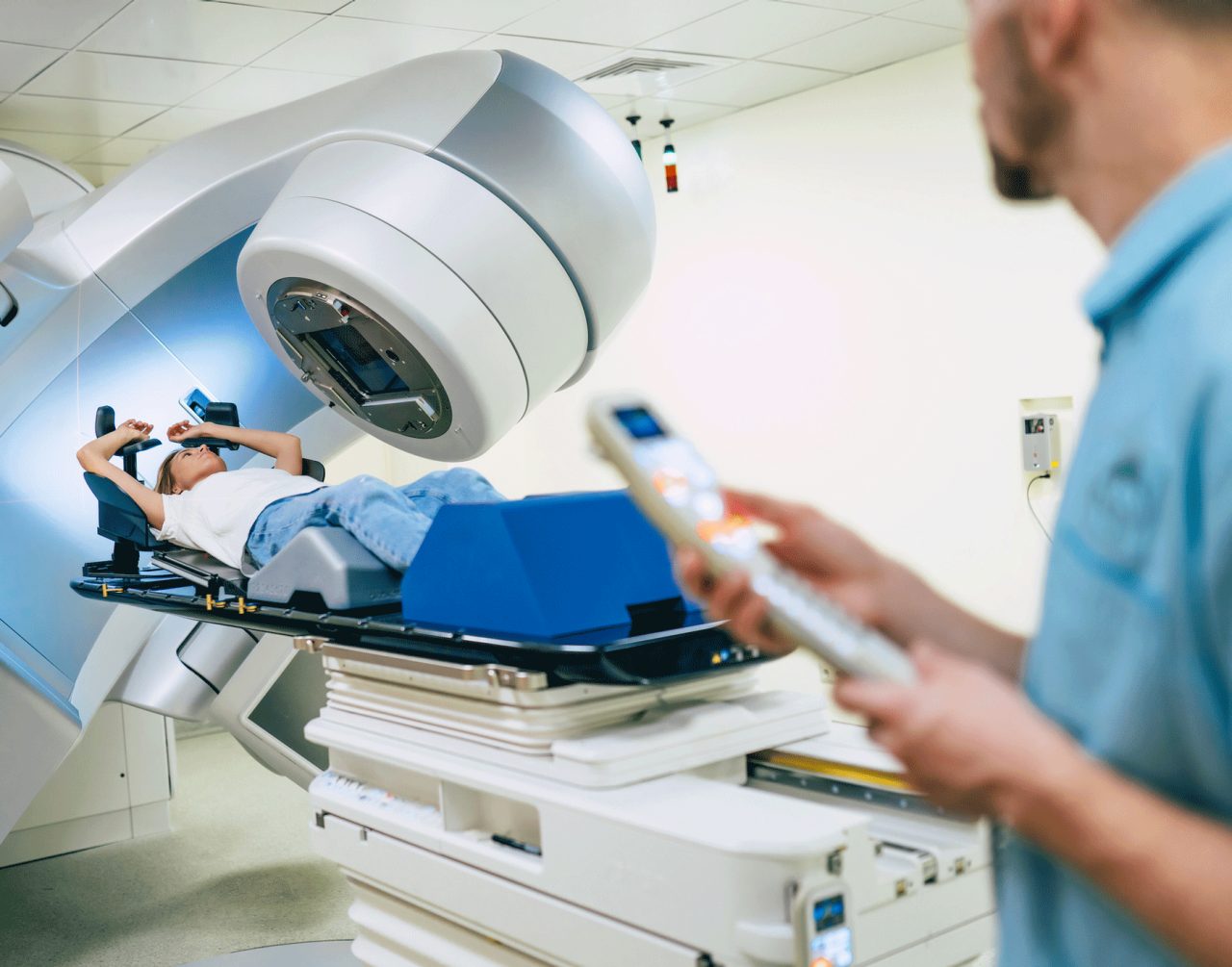
To kill cancer cells, your doctors may recommend exposing them to radiation therapy, usually via x-rays. These intense beams of energy damage their DNA.
What is radiation therapy?
More than half of all cancer patients receive radiation therapy, which can treat almost any kind of cancer. It is sometimes the only treatment a patient needs. Beams of intense energy, most often x-rays, damage the genetic material in cancer cells, interfering with the signals that allow them to grow and divide.
The energy most often comes from a machine outside your body, aimed at a precise point, but it is sometimes placed inside, close to the cancer, or delivered in a liquid.
The radiation beams may sometimes kill neighboring healthy cells. Often, however, noncancerous cells can recover from any damage.
Some people are able to work full-time during radiation therapy, some not at all.
YOU MIGHT ALSO LIKE: Can Cancer Be Tracked and Treated in Real Time?
When is radiation therapy used?
Cancer patients may receive radiation therapy more than once. It can be helpful before surgery, to shrink a malignant tumor. This is called neoadjuvant therapy. With intraoperative radiation, you can receive the beams close to the tumor without affecting the skin.
Radiation can be helpful after surgery if any cancer cells remain. This is called adjuvant therapy. You might also receive chemotherapy.
In addition, radiation can help calm symptoms in advanced cases and make patients more comfortable.
What are the risks of radiation therapy?
Ask your doctor about the risks of your radiation therapy, including possible side effects. Although the side effects of radiation can be miserable, they usually don’t last after the treatment ends. Some side effects can appear later.
It’s common to lose hair at the treatment site, sometimes permanently. You might also be very tired. Other side effects vary depending on the location of your cancer. If your chest receives radiation, you may develop a cough and shortness of breath. If your pelvis receives radiation, you might develop an irritated bladder, diarrhea, or sexual problems.
What will I experience during radiation therapy?
With external beam radiation, you’ll most likely receive 10-to-30-minute treatments five days a week. Short breaks allow healthy cells to repair any damage. The process can take several weeks altogether.
To make sure the energy beams land on the correct spot, you will get a kind of practice run, a simulation in which you’ll be positioned on a table with cushions and restraints. You’ll have to stay still, so it’s important to be comfortable. You will also have a computerized tomography (or CT) scan to pinpoint the treatment target. Your team calculates a dose and focus to protect healthy tissue and kill the cancer cells.
During a treatment session, you'll lie down in the position planned beforehand. Next, a buzzing linear accelerator machine rotates around your body, delivering the rays from different angles. It isn’t likely to be painful, and you’ll be able to gesture or speak to a radiation team.
Follow-up scans provide information on how the therapy affected your cancer.
With internal radiation, the source of the beams is a solid or liquid placed inside the body. In brachytherapy (brak-e-THER-uh-pee), seeds, ribbons, or capsules that contain a radiation source are placed in or near the tumor and will give off radiation for some time. This is most likely in cases of cancers of the head and neck, breast, cervix, prostate, and eye.
Systemic therapy uses a liquid that travels in the blood to reach cancer cells in many parts of the body. The patient might receive the liquid through their mouth, an IV line in a vein, or through an injection.
Radiopharmaceuticals, a type of medication, can treat pain from cancer that has spread to the bone.
Radioactive iodine treats some kinds of thyroid cancer.
How does radiation therapy work?
The beams of energy destroy the DNA in cancer cells. This process can take some time. Eventually, cells with damaged DNA stop dividing or die.
It may take weeks or months to see a difference, as cancer cells slowly die.
Updated:
September 08, 2022
Reviewed By:
Janet O’Dell, RN