Better Treatment for Psoriasis
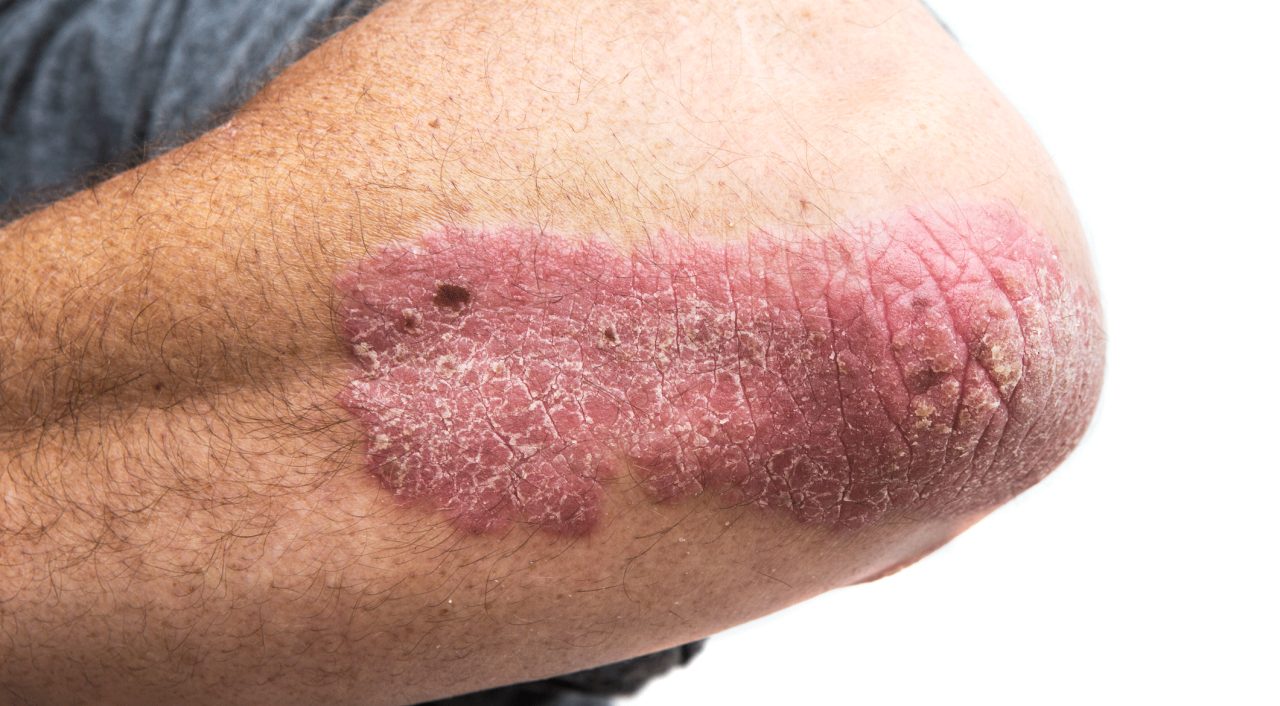
Psoriasis attacks your immune system. Medicines called biologics have radically changed treatment. How safe and effective are biologic treatments for psoriasis?
What is psoriasis?
When you have psoriasis, overactive T-cells in your blood collect in your skin, triggering skin cells to grow about 10 times faster than normal. You end up with thick red patches of itchy dry skin, often on your knees and elbows, and sometimes joint pain.
Psoriasis is one of several autoimmune illnesses in which your immune system, designed to fight dangerous foreign cells, attacks healthy tissue. It’s a common problem, affecting millions of people around the world.
Medications called biologics (lab-made versions of living cells) can calm your immune system. They have radically changed how autoimmune diseases are treated.
YOU MIGHT ALSO LIKE: The Link Between Psoriasis and Diabetes
Treatment for psoriasis
Doctors advise starting with the mildest treatment, depending on your type of psoriasis and how much of your body it covers.
The most frequently prescribed medications are corticosteroids, available as ointments, creams, lotions, gels, foams, sprays, and shampoos. You might apply the medicine once a day during flares and on alternate days or weekends only when you don’t have symptoms. Corticosteroids, however, can stop working over time.
Your case qualifies as moderate to severe if more than five to 10 percent of your skin is affected (the surface of one of your palms, including your fingers, would count as 1 percent).
Methotrexate has been the first-line treatment for moderate-to-severe psoriasis since the 1960s. But newer biologics may be both more effective and safer, according to a Harvard study that analyzed records of more than 100,000 psoriasis patients who took medication.
Methotrexate affects all of your cells, interfering with growth. Biologics are more targeted, focusing on specific immune molecules called cytokines.
The drawback of biologics is that you will need an IV infusion or, depending on the drug, you can give yourself injections. They’re relatively new, so the safety record is still growing.
And they’re expensive. If you don’t have insurance to cover the cost, biologics will cost thousands of dollars a month. You may ask the drug manufacturer for a discount, however.
Biologics may also have side effects.
Biologics include:
- Secukinumab (Cosentyx)
- Adalimumab (Humira)
- Etanercept (Enbrel)
- Infliximab (Remicade)
- Ustekinumab (Stelara)
- Ixekizumab (Taltz)
- Tildrakizumab (Ilumya)
- Apremilast (Otezla)
Treatments do not cure psoriasis but relieve symptoms. Overall, more than half of people who take biologics get a 75 percent improvement in the condition of their skin within three to four months, and even more get relief from joint pain.
A newer drug, bimekizumab, made the condition go away completely for 67 percent of patients after 48 weeks of treatment, compared with 46 percent of patients receiving secukinumab.
Other drugs biologics block the pro-inflammatory biochemical, IL-17A, the most potent form of interleukin-17, which helps your immune system fight inflammation. Bimekizumab blocks that chemical plus IL-17F, a similar chemical that is more abundant in your body.
In another clinical trial, after 16 weeks, 86 percent of patients on bimekizumab had a 90 percent reduction in their psoriasis, compared to 47 percent of those taking adalimumab. Bimekizumab also treats psoriatic arthritis.
The downside: In the 48-week study, nearly 20 percent of the volunteers got thrush, a yeast infection in the mouth, which was treated with a common anti-fungal drug. The volunteers also experienced diarrhea. More seriously, it’s possible that, like other drugs that block interleukin-17, it may increase the risk of other infections and cancer.
You can combine any of the current biologics with light therapy or a topical cream, and some can be combined with methotrexate.
Updated:
July 12, 2023
Reviewed By:
Janet O’Dell