Breast Cancer Diagnosis
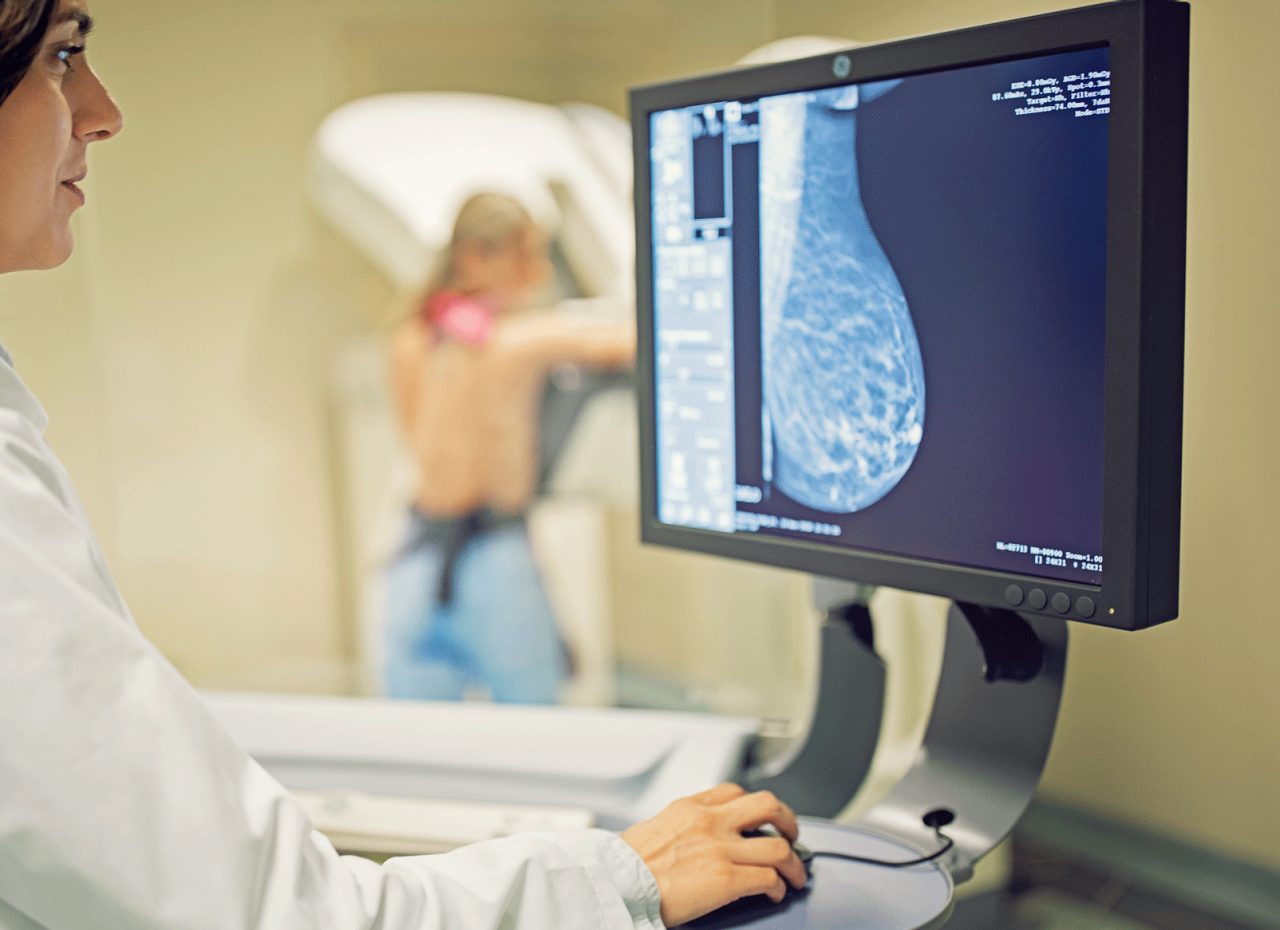
Finding breast cancer involves more than a mammogram. Other tests provide important information, but a biopsy is needed to confirm a breast cancer diagnosis.
If you’re a woman who’s found a lump in her breast while bathing or performing a self-exam — or if a doctor has called about a screening mammogram that’s spotted something irregular — it’s hard not to assume you have breast cancer.
A breast cancer diagnosis, however, involves far more testing than a manual exam or an initial mammogram.
Not only are additional tests needed to confirm or rule out a breast malignancy, but they provide your doctor with information about the stage of the disease and what treatment is best.
YOU MIGHT ALSO LIKE: Why You Should Get Your Annual Mammogram
The first steps in a breast cancer diagnosis
A new lump or mass in your breast is the most common symptom of a breast malignancy, according to the American Cancer Society. While a hard, painless lump with irregular edges is more likely to be cancer than soft and round masses, there’s no way to make a breast cancer diagnosis based on what a mass feels like alone. If you or your doctor find you have a breast irregularity, however, it can be the first step toward appropriate testing for a possible breast cancer diagnosis.
Of course, breast cancer may produce no symptoms in the earliest stage of the disease; that’s why regular breast cancer screening is important. A screening mammogram takes x-ray pictures of each breast from different angles to search for any signs of breast cancer in women who don’t have known breast symptoms.
If the mammogram reveals an area has changed from a prior mammogram or shows an abnormal area, such as masses or calcifications, it doesn’t diagnose breast cancer. It does, however, indicate more imaging is needed.
Making a definitive breast cancer diagnosis
After suspicious areas are found in your breast, your doctor will order other tests or refer you to a breast cancer specialist. This does not mean you definitely have cancer, the Centers for Disease Control and Prevention points out.
Before you can receive a diagnosis, you’ll likely get a diagnostic mammogram. Although it’s done much like a screening mammogram, it takes more x-ray pictures of various angles, paying extra attention to any section of the breast that has raised concern. You may have other imaging tests — an ultrasound or a magnetic resonance imagining (MRI) —to take pictures of the inside of your breast.
If your doctor believes you likely have a malignancy, a breast biopsy is next, the only way to make a definitive breast cancer diagnosis. Cells or small pieces of tissue are removed from the area of the breast where a malignancy is suspected, which a pathologist examines under a microscope to check for signs of cancer, the National Cancer Institute (NCI) explains.
There are different kinds of breast biopsies, some involving incisions and other a fine, hollow needle. For most areas in your breast, the less invasive needle biopsy is appropriate.
If breast cancer is confirmed, you may need a biopsy of one or more lymph nodes — either at the same time as the breast biopsy of the breast tumor, or when a breast tumor is surgically removed — to see if the cancer has spread.
After your diagnosis, your oncologist will conduct additional tests to see what treatment is best for your cancer, based on whether your malignancy:
- Is at a very early stage
- Has spread to lymph glands and possibly beyond
- Is hormone dependent (indicating hormone blocking therapy may be an appropriate therapy)
Updated:
May 03, 2023
Reviewed By:
Janet O’Dell, RN