The Heartbreak and Joy of Premature Babies
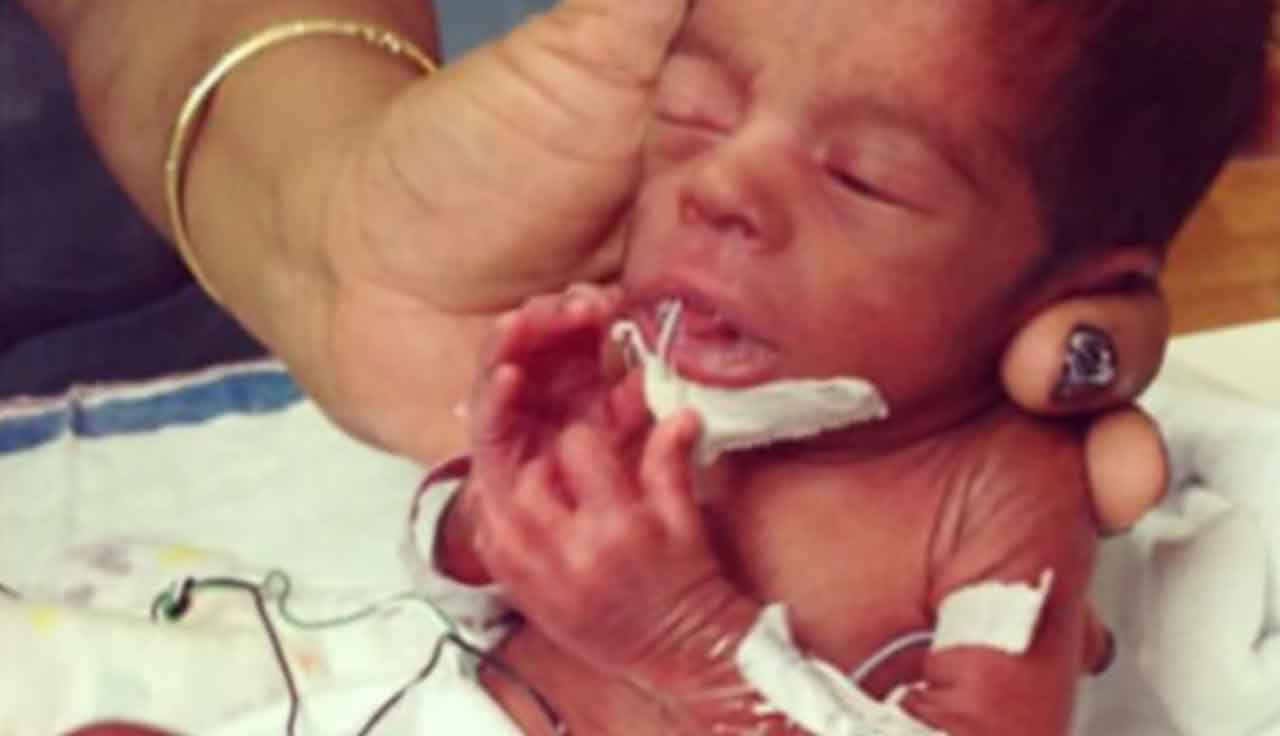
Jaelynn Brown in the NICU. PHOTO COURTESTY JO-VANNE BASKERVILLE BROWN.
One in 10 U.S. infants is born preterm, often facing serious and sometimes fatal health problems. Here are two stories of premature babies who are thriving.
When a woman learns she is pregnant, she anticipates her baby coming along in nine months. Most every mom-to-be assumes her infant will be born healthy around her due date.
Most of the time, that’s what happens. But some babies are born premature.
YOU MIGHT ALSO LIKE: When Your Baby Is in Neonatal Intensive Care
Premature babies, born before 37 weeks of pregnancy, are not a rarity in the U.S. About one in every 10 American infants is born prematurely, according to the Centers for Disease Control and Prevention. Those babies are not simply tinier than normal. They are often born with immediate health problems, including breathing difficulties, bleeding in the brain, jaundice, and anemia. They may also face an increased risk of problems with vision and developmental and long-term neurological disabilities.
Preterm birth is the greatest cause of infant mortality, especially for babies born very early, before 32 weeks. Worldwide, 15 million babies are born too soon each year, and nearly one million of those infants die as a result of their early births, according to the World Health Organization.
The number of premature births in the U.S. has decreased slightly, although they did increase from 2015 through 2021 after falling in the early 2010s.
Statistics and medical facts are important. But there’s another element to premature birth — the individual family’s struggles, worries, heartbreak, and, often, joy watching their preemie survive and even thrive.
We asked two moms of preemies who commented on our Facebook page to tell their stories of going through it all and, thankfully, emerging with tales of hope for other families who may have a preemie in the neonatal intensive care unit (NICU).
Jaelynn’s story
First-time mom Jo-Vanne Baskerville-Brown didn’t have a problem-free pregnancy. She was diagnosed with fibroids (abnormal benign growths in her uterus) and high blood pressure. Then, when she was 30 weeks pregnant, she began bleeding.
An emergency trip to the hospital confirmed Jo-Vanne was in premature labor and her unborn baby was in trouble. A C-section delivered her baby girl, Jaelynn. Weighing 2 lbs. 5 oz., the tiny preemie had jaundice and bleeding in her brain. Unable to feed, she received nutrients through an intravenous line.
Jo-Vanne and her husband, Da Juan Brown, were heartsick with worry. “I wanted to put myself in her tiny place and I just felt horrible as a mother,” Jo-Vanne says. “As a parent you want to protect your child and take away all of the pain, and to know that I couldn’t do that was the worst feeling in the world.”
The stress took a physical toll on the new mom. Her blood pressure spiked dangerously high, and she was unable to see her baby for two days after giving birth.
A friend sent Jo-Vanne messages of support, and the family turned to prayer for comfort. Doctors and nurses at Jacobi Hospital, located in the Bronx, N.Y, offered encouragement, answered questions, and helped Jo-Vanne and her husband realize there was hope for their preemie. Slowly, their baby’s condition improved.
In all, Jaelynn was in the NICU for seven weeks and two days. Her mom visited every day for about 12 hours, going home at midnight or later. “I never wanted to leave, but I had to get sleep and energize my body in order to be any good for her,” Jo-Vanne says. “I also had to pump milk so that I could bring it to the hospital.”
Today, Jaelynn is two and a half years old. Her progress has been remarkable. Her parents report their toddler walks, runs, jumps, plays with her toys, knows her colors, can say the entire alphabet, and often speaks in sentences — including telling her mom to “Please get me some juice!” She’s also learned some Spanish.
Jaelynn experiences residual breathing problems during winter due to her premature birth. “She uses a nebulizer machine and an inhaler — but we only need them when the weather is extremely cold,” her mom explains.
Jo-Vanne urges parents of premature babies to participate in any early intervention programs their doctors recommend. “They are so beneficial for children born too early. Jaelynn was given physical therapy, and the result has been amazing,” she says. “I feel as though my purpose in life now is to advocate for all women that birth children too early.”
To that end, Jo-Vanne and her family have supported the March of Dimes since 2013, participating in fundraising efforts. “Our team name is ‘A Walk for Princess Jaelynn,’” she says. “My husband and I can’t wait to see how Jaelynn continues to grow and develop. I want her to know that no matter what she experiences in life, mommy and daddy will always be here for her.”

A thriving Jaelynn Brown. PHOTO COURTESTY JO-VANNE BASKERVILLE BROWN.
Judah’s story
Jamie Reid and her husband, Richard, of Cullman, Ala., already had a large family when their youngest, Judah, was born. Their other children — Devon, Kai, Cade, Ace, and Layne — had normal births. But Judah came too early.
Born at 34 weeks and weighing 5 lbs. and 3 oz., the little preemie soon developed breathing problems. His doctor at St. Vincent Hospital in Birmingham placed the tiny baby on a CPAP (continuous positive airway pressure) machine to help.
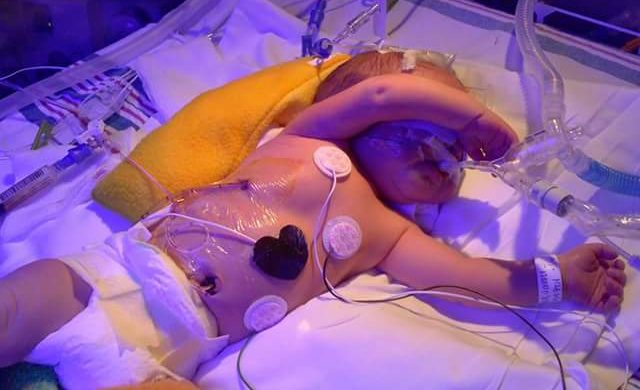
Judah Reid in the NICU. PHOTO COURTESY JAMIE REID.
By the next morning, Judah had developed a pneumothorax, the medical term for a collapsed lung, and was connected to a ventilator with a tube in his tiny chest.
“I was devastated,” Jamie recalls. “I could barely stand to look at him with all those tubes and wires. We were not allowed to hold him or touch him. His vitals went crazy with any kind of stimulus.”
In many premature infants, lungs are not fully developed and lack a slippery substance called surfactant that helps lungs fill with air and keeps the air sacs from deflating. Judah’s doctor used a surfactant derived from cows’ lungs in hopes of spurring Judah's lungs to work properly.
“I had never heard of that, but the doctor said they would try it up to four times, and if it worked, Judah would have a good chance at survival,” Jamie says.
“Up until that point, I had never considered the fact that my baby might not make it. I completely lost it. Luckily my husband was my rock at that moment. I cried and screamed, and then went numb. Those were the hardest days of my life. It was definitely an emotional roller coaster.”
On the fourth and last day of cow surfactant, the treatment finally succeeded.
“Judah's lungs started working on their own! The air around his lungs dissipated,” his mom explains. “At that point, they started removing some of the wires. The chest tube was removed first, then the PICC line (a type of catheter) in his head, then the feeding tube and, on day nine, they removed the ventilator.”
“I finally got to hold my precious baby boy! He recovered quickly and we took him home when he was 13 days old.”

Judah Reid with his mom. PHOTO COURTESY JAMIE REID.
Today, Judah is a healthy, happy, 20-month-old toddler. “He walks, talks, and chases after his five big brothers. He is an absolute joy to us,” Jamie says.
“My advice to parents with babies in the NICU is to trust the doctors and nurses and take care of yourself. Do what you can for your baby. The only thing I could do for Judah was pump breast milk, which they gave him in his feeding tube. It made me feel like I was helping him, at least a little,” she adds. “Just breathe, and take it day by day, minute by minute if you have to. Be strong for your baby."
Updated:
November 22, 2023
Reviewed By:
Janet O’Dell, RN