The Plight of the Rural Hospital
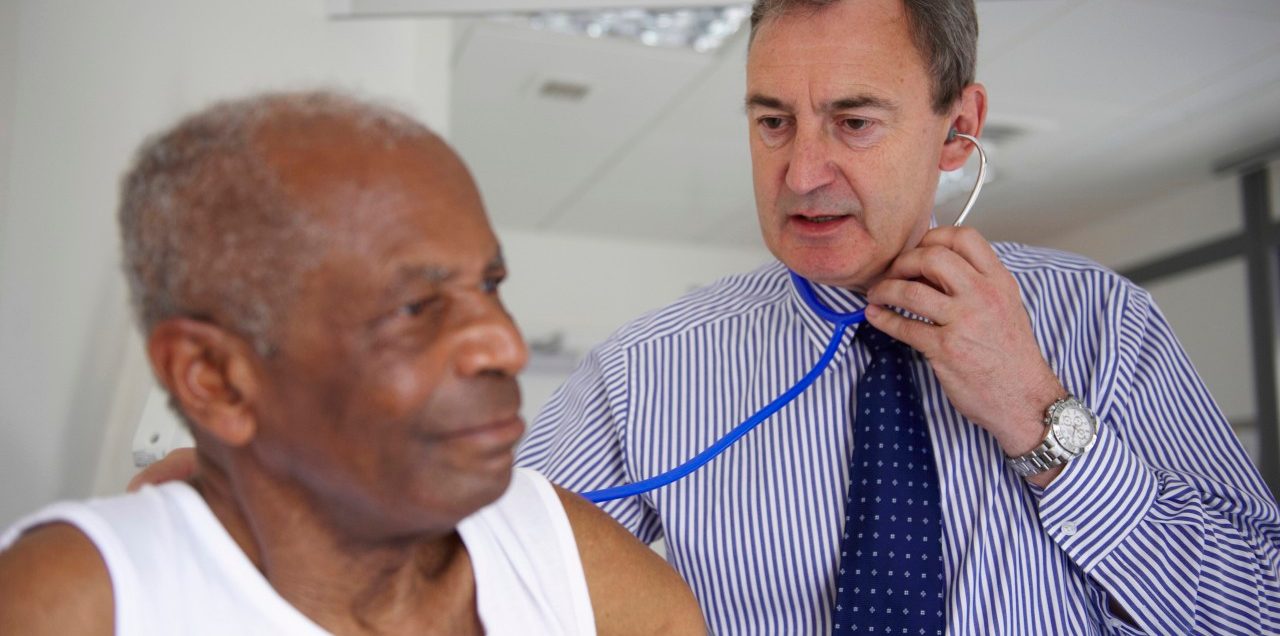
Why a wave of closures is putting rural residents’ health at risk.
On October 10, 2015, Mercy Hospital became a casualty. The century-old health facility shut down, leaving the 9,500 residents of rural Independence, Kan., without a local hospital for medical emergencies.
“It’s a sad day for our community, a sad time for our coworkers and our patients,” said hospital spokesperson, Joanne Smith. She said the hospital’s plight was the result of a “perfect storm” of causes, from a declining patient population to a lack of Medicaid expansion funding.
YOU MIGHT ALSO LIKE: A Texas Doctor’s Innovate Leadership Brings Help and Hope to Rural Residents
Mercy Hospital is just one of 76 rural U.S. hospitals that have shut their doors since 2010, according to the Sheps Center for Health Services Research at the University of North Carolina. The rate of hospital closures in small, remote communities has soared over the past six years. “About half of the closed hospitals continue to provide access to some health services as outpatient clinics or other type of facilities. The other half no longer provide health services of any kind,” said lead study author Brystana Kaufman, MSPH.
Nearly 700 rural facilities that are still operational today are at imminent risk for closure due to poor financial performance, finds a report by iVantage Health Analytics. The high rate of hospital shutdowns, and the risk of more to come have left the communities these facilities serve vulnerable.
Why rural health care is going out of business
A number of factors have been blamed for rural hospital closures, particularly a lack of Medicaid expansion and increasing regulations under the Affordable Care Act. In reality, the causes are even more diverse and complex.
To get at the root of rural hospital closures, in 2016 the Kaiser Family Foundation analyzed three facilities: Mercy Hospital in Independence, Kan., Parkway Regional Hospital in Fulton, Ky., and Marlboro Park Hospital in Bennettsville, S.C. The Foundation discovered that several factors contributed to the shutdown of these hospitals, including shrinking populations, high rates of uninsured patients, and outdated facilities and care delivery models.
In many small towns, factories have closed, taking good jobs with them. The population that’s left behind is often poor and elderly — people with big healthcare needs but little health insurance to pay for it. While some states have expanded Medicaid to cover low-income people who wouldn’t normally qualify for this program, other states — including Kansas — have not. This lack of Medicare expansion has left hospitals footing the bill for patients who can’t afford to pay.
Adding to the burden are increased regulations under the Affordable Care Act. Enhanced automation and reporting requirements, coupled with shrinking reimbursements, have been catastrophic for some smaller facilities.
Many rural hospitals already lack the funds to invest in the latest treatments and technologies, and dwindling hospital budgets restrict their access to modern healthcare even further. An inability to provide state-of-the-art care has driven both doctors and patients to larger towns with more modern facilities, cutting revenue even more.
What will happen to patients?
Every time a rural hospital closes, residents have less access to both emergency and primary care, and they must face longer travel times to get the health services they need. Needing to drive 40 minutes for healthcare can mean the difference between life and death in an emergency situation.
A 2006 report from the Sheps Center finds that when rural hospitals close, their entire communities sink even deeper into financial trouble as more jobs and tax revenues are lost. A single closed hospital reduces per capita income by more than $700, and increases unemployment in the community by 1.6 percent.
Legislation introduced in April 2016 by a bipartisan group of U.S. senators seeks to provide struggling rural hospitals with increased Medicare reimbursements to help them stay afloat (the bill has yet to go anywhere in Congress). But in order to survive, these hospitals must also evolve in ways that are feasible for them. They need to hold onto quality staff, and find a way to provide modernized care, either through increased investments or by giving patients access to telemedicine. Kaufman says, “…new models of rural healthcare may be needed to provide essential services for these communities.”
Updated:
April 06, 2020
Reviewed By:
Janet O’Dell, RN