Squamous Cell Skin Carcinoma Symptoms
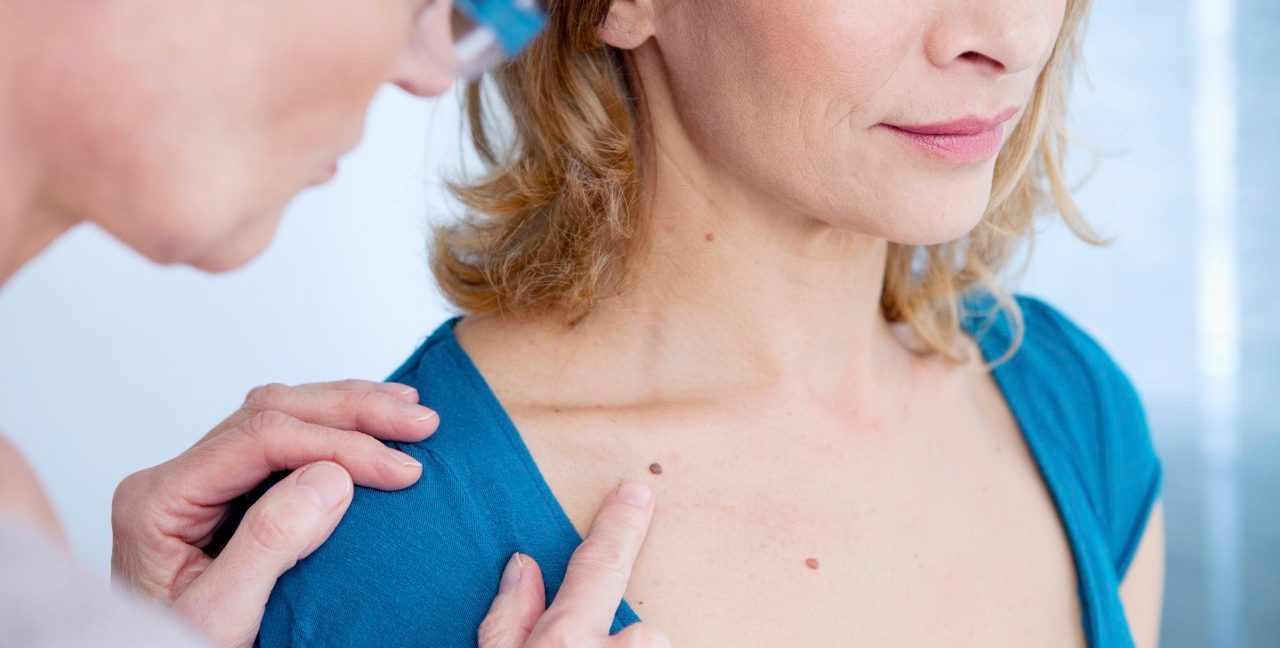
See your doctor if you have any squamous cell skin carcinoma symptoms. While this skin cancer doesn’t often spread, it can — so don’t ignore symptoms.
Squamous cell skin carcinoma is a common form of skin cancer. It develops when abnormal cells grow out of control in your skin’s middle and outer layers. Unlike potentially deadly melanoma skin cancer, squamous cell skin cancer is typically not life-threatening.
That doesn’t mean it’s safe to ignore squamous cell skin carcinoma symptoms.
Without treatment, this form of skin cancer can grow deeper and wider. In some cases, it can be aggressive, spreading to other parts of your body, causing potentially serious complications.
YOU MIGHT ALSO LIKE: Our Skin Cancer section
Squamous cell skin carcinoma symptoms
Prolonged exposure to ultraviolet radiation causes most squamous cell carcinomas of the skin, either from direct sunshine or from tanning beds or lamps. Squamous cell skin cancers usually occur on areas of your body often exposed to the sun, especially your face, lips, ears, neck, and back of your hands.
This skin cancer may also develop in scars or skin sores on other parts of your body. Infrequently, squamous cell skin cancer forms in the genital area, too, the American Cancer Society points out.
Common squamous cell skin carcinoma symptoms include:
- Thick red patches, often with a raised border, that feel rough and scaly and may crust over or bleed
- Wart-like growths
- Raised growths, sometimes with a lower area in the center of the lump
- Open sores that don’t heal, or that heal for a while and then return. The sores may ooze and have crusted areas, too.
Squamous cell skin cancer can also simply appear as a flat area only slightly different from your normal skin, according to the American Cancer Society (ACS).
Skin self-exam for squamous cell skin carcinoma
Knowing your own skin is the best way to protect yourself from skin cancer. You can spot skin cancers in early stages, when they are most easily treated.
A self-exam can also reveal changes indicating pre-cancerous growths called actinic keratoses which increase the risk of developing squamous cell carcinomas. The rough and scaly growths are slightly raised, can be brown or red in color, and are found on the most sun-exposed areas of your body. The risk for actinic keratoses increases with age.
Although the growths are benign, removing them can often prevent squamous cell skin carcinomas in the future. Fourty to 60 percent of squamous cell carcinomas begin as untreated actinic keratoses, according to the Skin Cancer Foundation.
It’s a good idea to check your skin once a month in a room with a full-length mirror and good lighting. Use a hand-held mirror to examine parts of your body that are difficult to see (like the back of your thighs), and don’t forget to examine your nails, back, ears, the palms of your hands, and the soles of your feet. Ask a friend or family member to help you look for any skin changes on your scalp and back.
If you note changes in your skin, such as growths or color changes in moles and any new blemishes, freckles, or unexplained rough patches, talk to your doctor.
Checking out squamous cell skin carcinoma symptoms
Your doctor or dermatologist will use a variety of techniques to investigate changes in your skin. A special magnifying lens and light can sometimes reveal the change in your skin is benign.
If a suspicious area needs to be examined for cancer, the doctor will remove a small area for a biopsy, using a local anesthetic. The ACS explains that when a biopsy removes the entire skin growth — and the growth turns out to be a squamous cell carcinoma — the biopsy alone is often enough to cure the cancer without further treatment.
YOU MIGHT ALSO LIKE: How Is Nonmelanoma Skin Cancer Treated?
Updated:
May 26, 2023
Reviewed By:
Janet O’Dell, RN