Symptoms of Lyme Disease
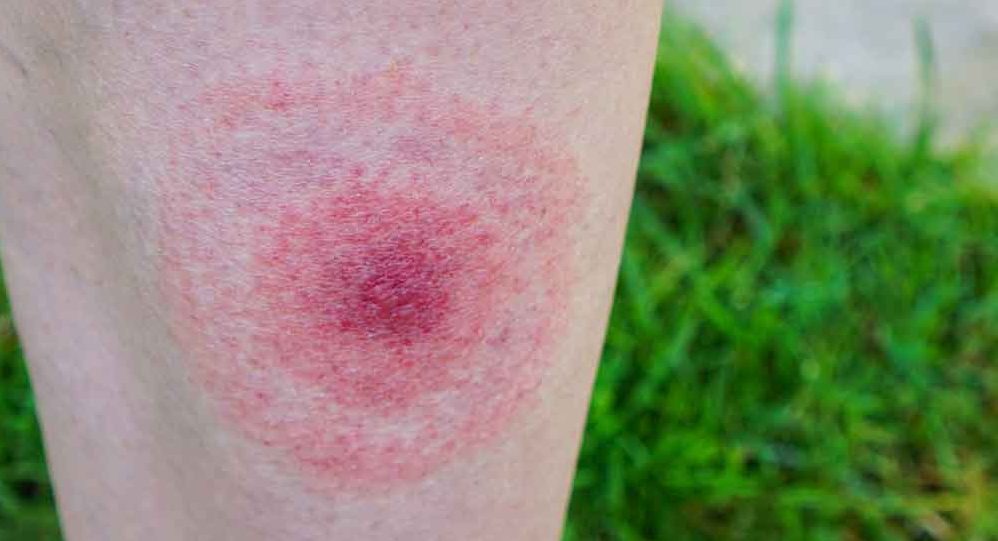
Recognize the early symptoms of Lyme disease: a red bump, an expanding rash, feeling like you have the flu, and even arthritis, heart, and neurological problems.
Speedy treatment — within days or weeks — is the best way to prevent the complications of the infectious disease Lyme disease.
How do you get Lyme disease?
The deer tick that transmits Lyme disease can be as small as a poppy seed. You may not even notice a bite. The best way to protect yourself may be to vigilantly check for the symptoms of Lyme disease.
The Centers for Disease Control and Prevention (CDC) estimates about 500,000 new cases of Lyme disease occur each year — and the danger of catching it is growing significantly.
YOU MIGHT ALSO LIKE: Prevention Guidelines for Lyme Disease
CDC charts dramatically illustrate the recent expansion of Lyme. While once confined to Connecticut and a small part of the Midwest, it’s been reported throughout the entire eastern seaboard over the past two decades. Though less commonly, it now occurs throughout the country, from California and Oregon to Florida and Texas.
Unfortunately, testing isn’t always reliable, because the Borrelia burgdorferi bacteria that causes Lyme disease takes time to work its way through your body. Even the tests doctors do have — such as ELISA or the Western blot — may return false negative or false positive results. More accurate tests are under development, as is a human vaccine.
What are the symptoms of Lyme disease?
Here are symptoms of Lyme disease to watch for.
A red bump. While it’s easy to miss a bite, some people do report finding a red bump. It may look like a spider or mosquito bite, but it may not be painful. Don’t brush it off — see a doc right away.
Diffuse, expanding rash. Within a few days, a red rash can grow around the bite. It may be warm but probably not painful. Called erythema migrans, this rash can appear in a single location, such as behind a knee, or in several locations around your body. In one study of 118 people with confirmed Lyme, half had a rash on the lower part of their body (the legs, hips, groin). A quarter reported a rash on their upper body — the armpit, shoulder, or arm.
A rash should be enough to establish an immediate diagnosis of Lyme. Not everyone will develop one, but it’s very common: The CDC estimates it occurs in 70 to 80 percent of cases. In the study, all participants had some kind of rash — for three in five, it was uniformly red throughout, while one in three had a rash that was redder in the center. Only one in 10, however, had the classic bull’s eye pattern associated with Lyme. (See pictures of common rashes here.)
Note that other tick-borne diseases, such as Rocky Mountain spotted fever or ehrlichiosis, can also cause a rash. Be sure your doc tests for the range of illnesses that ticks likely transmit.
Flu-like symptoms. Achiness, headache, and fatigue are other common symptoms of early Lyme disease, whether they accompany a rash. If you start to feel sluggish and as if you’re coming down with the flu at the height of summer, pay attention, and see your doctor quickly. Feeling hot or chilled is also common, though your body temperature may read as normal. In the above study, one in three people reported feeling feverish, yet only 6 percent in fact had a measurable fever.
Arthritis, heart, and neurological symptoms. Lyme disease often eventually moves into your joints, nervous system, and heart. Arthritis or pain in your joints could develop within months and should be checked out by a doctor. In addition, don’t dismiss emotional symptoms, such as grumpiness, irritability, or weepiness. Lyme can have serious neurological effects as well. As Lyme progresses, short-term memory loss, facial paralysis, shortness of breath, and heart palpitations can appear within days to months of infection, says the CDC.
How to protect against getting Lyme disease
Vigilance and protection are key in the battle against Lyme. If you’re in a Lyme-prone area, check yourself for ticks once or twice a day and shower at least once a day, ideally before sleep or immediately after a hike or gardening. If you’re bitten by a tick, follow the proper steps for removal. A simple tool called a Tick Key may be easier to use than tweezers (keep it on your keychain). Save the tick if you can: You or your doctor may choose to send it for testing.
YOU MIGHT ALSO LIKE: How to Protect Yourself from Tick-Borne Diseases
Updated:
March 28, 2023
Reviewed By:
Janet O’Dell, RN