What Is a Widowmaker Heart Attack?
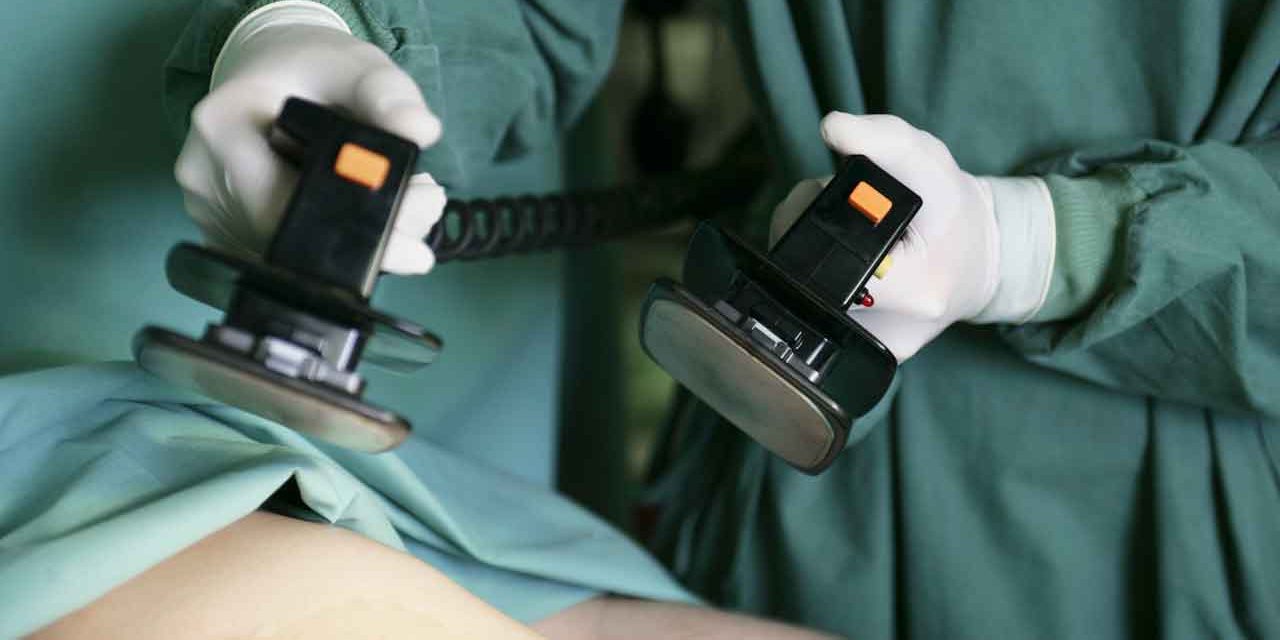
Don’t let the name confuse you: Both men and women can get a “widowmaker heart attack,” which is often a 100 percent blockage in the most important artery to the heart.
Don’t rush to conclusions if you hear the term “widowmaker heart attack.”
“People often refer to heart attacks as widow makers inaccurately, which generates a great deal of anxiety,” explains Mustafa Ahmed, MD, an interventional cardiologist in Birmingham, Ala.
Even if your loved one actually has had this kind of heart attack, it doesn’t have to be fatal immediately or indicate a likelihood of another fatal attack.
YOU MIGHT ALSO LIKE: What Causes a Heart Attack?
Heart attacks occur when plaque forms inside an artery, or when a blood clot dislodges from elsewhere in your body, and blocks the flow of blood. When a patient enters the emergency room with heart attack symptoms, the team promptly performs an electrocardiogram (EKG) or heart tracing to detect which artery is blocked and how badly.
The worst situation: a significant blockage, sometimes 100 percent, in the left coronary artery to the heart, which supplies oxygenated blood. If you make it to the hospital, you will most likely immediately undergo open heart surgery.
The more common threat described as a widowmaker heart attack actually occurs further on in the left anterior descending (LAD) artery. The left main artery brings oxygenated blood to the LAD and also the circumflex artery. The LAD runs down the front of your heart and supplies the front and main wall. If it is either completely or significantly blocked near the beginning, the front of the heart loses its blood supply. But you’re in better shape than you would be with a main artery blockage, because the left side still has a second source of blood, the circumflex artery.
The truth is that both men and women can get a widowmaker, and it isn’t always fatal. You’ll need a procedure to open up the blood flow in the LAD and compensate for any scarring. The chances of death go down dramatically if the artery is opened in less than an hour.
The signs of this kind of heart attack are usually classic: chest pain and trouble breathing. The celebrity trainer Bob Harper, who appears on “The Biggest Loser” TV show, has described his heart attack as a widowmaker. He dropped to his knees after his usual workout, unable to breathe. Harper was lucky — his coach found doctors who gave him CPR and a jolt from a defibrillator, which restores the heart’s rhythm, and he got to the hospital quickly.
A LAD blockage can be treated with a stent. To open up a blockage, your team inserts a catheter with a balloon at the tip, moves it to the point of the blockage, and inflates the balloon. This procedure, a balloon angioplasty, pushes back the plaque. The balloon comes out again. In about a third of balloon angioplasty patients, the artery will close up again within months. For a longer-lasting solution, your team is likely to put in a stent, a wire-mesh tube. This time, a collapsed stent straddles the balloon, which again is inserted at the end of a catheter and inflated at the key spot. The stent expands, and locks in place. Some stents disappear on their own over time.
Stents may be coated with drugs that help keep the artery from closing up again. Those drugs may be making stents in the LAD more successful, according to a study of more than 8,700 stent patients. Researchers compared patients with a stent in the LAD to those who had a stent outside it. Four years after the procedure, 5.8 percent of both groups had died, with no difference between the two. A second heart attack in that period was slightly more likely in the LAD group, but 94 percent of those patients did not have one.
Updated:
March 03, 2020
Reviewed By:
Christopher Nystuen, MD, MBA