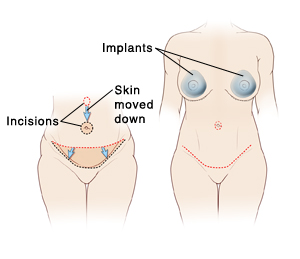
Tummy Tuck with Breast Implants
Tummy Tuck with Breast Implants
Abdominoplasty (“tummy tuck”) and breast augmentation (implants) are two cosmetic surgeries that may be done together. Having a tummy tuck can remove excess fat and skin from your belly. It can also tighten weaknesses in the abdominal wall by repositioning the affected muscles. Breast augmentation is surgery to place breast implants, which makes the breasts larger. This sheet explains how the two procedures are done.
Different kinds of implants
Breast implants are made of a silicone shell. The shell may be filled with saline (saltwater) or silicone (gel). Different implant sizes, shapes, and textures are available, as well as different thicknesses of silicone. There are benefits and drawbacks to each type of implant. You and your doctor will discuss which type is best for you.
Preparing for surgery
Meet with your surgeon before the day of surgery to ask questions about the doctor's experience with breast augmentation, your specific surgery, and the results you can expect. The Food and Drug Administration (FDA) provides a list of questions that may help you with this conversation. Ask your doctor what makes you a good candidate for breast implants, and what your options are for size, shape, and surface texture. Your doctor will also review the risks and benefits of the surgery. Ask for before and after pictures of other patients so you can understand whether your expectations are realistic.
During this meeting, ask the doctor for a copy of the patient labeling for the breast implant that will be used. As a patient, it is your right to have this information and the doctor will expect to provide it. Talk with your doctor about the risk of breast implant associated anaplastic large cell lymphoma (BIA-ALCL), a rare type of non-Hodgkin's lymphoma that can develop after breast implants. While the exact number of cases is not known, the most current data suggest that BIA-ALCL is seen more often after breast implants with textured surfaces rather than those with smooth surfaces.
Read and understand the informed consent form. Ask any questions before you sign it.
Prepare for the surgery as you have been told. In addition:
Tell your doctor if you think you could be pregnant.
Some surgeons ask that you have a mammogram or breast X-rays before the surgery. This helps show any breast abnormality and gives the doctor a preoperative image of your breast tissue.
Tell your doctor about all medicines you take. This includes herbs and other supplements. It also includes any blood thinners, such as warfarin or daily aspirin. You may need to stop taking some or all of them before surgery.
Don't eat or drink during the 8 hours before your surgery, or as directed by your surgeon. This includes coffee, water, gum, and mints. (If you have been instructed to take medications, take them with a small sip of water.)
The day of surgery
The surgery takes about 4 to 6 hours. You will stay overnight for 1 or more nights.
Before the surgery begins:
An IV line is put into a vein in your arm or hand. This line delivers fluids and medicines.
To keep you pain free during surgery, you’re given general anesthesia. This medicine puts you into a state like deep sleep through the surgery. A tube may be inserted into your throat to help you breathe.
For breast implants:
The incision for the implant is made. You and your doctor will have discussed the placement of the incision before surgery. It may be under the breast. It may be under or within the areola (dark skin around the nipple). Or it may be under the arm.
The doctor forms a “pocket” to hold the implant. This may be above or below the chest muscle. Then the implant is inserted through the incision and into the pocket. If the implant needs to be filled with saline, it is done at this time. It is then positioned.
If both breasts are receiving implants, the procedure is repeated on the other breast.
A small tube (drain) may be placed in each incision. This drains excess fluid as the wound heals.
Incisions are closed with sutures (stitches), surgical glue, or both.
For the tummy tuck:
An incision is made in the belly from hipbone to hipbone. This is often along the lower part of the belly just above the pubic hairline. You and your doctor will choose the exact incision site prior to surgery. An incision is also made around the bellybutton.
The skin and fat beneath are lifted to expose the abdominal wall beneath. The abdominal wall includes fascia (fibrous tissue) and muscles.
If needed, the belly muscles are pulled together to tighten the abdominal wall. Stitches (sutures) are used down the middle of the belly, to hold the muscles in their new position.
After the abdominal wall is tightened, the skin and fat are pulled back down. Excess fat and skin are then removed from the belly.
Once the skin and fat are pulled down, the bellybutton may be covered up. In such cases, an incision is made so the bellybutton can be seen. The skin is then sewn into place around the bellybutton.
Small tubes (drains) may be placed near the incisions. These drain fluid that may build up as the wound heals.
Incisions are closed with sutures, surgical glue, or both.
After the surgery
You will be taken to a room to wake up from the anesthesia. You may feel sleepy and nauseated. If a breathing tube was used, your throat may be sore at first. You will be given medicine to control pain. If you need to stay overnight, you will be taken to a hospital room. Once you are ready to go home, you will be released to an adult family member or friend.
Recovering at home
Once home, follow any instructions you are given. Your doctor will tell you when you can return to your normal routine. During your recovery:
Take any prescribed medicines exactly as directed.
Wear the special bra or Ace bandage you were given before discharge as directed by your doctor.
Walk slightly bent at the waist, if suggested by your doctor. This helps protect the abdominal wall as it heals.
Care for your incisions and the dressing (bandage) over them as instructed by your doctor.
Don’t shower for 72 hours after surgery, or as instructed by your doctor. Don't swim, take a bath, use a hot tub, or do other activities that cause the incisions to be covered with water until your doctor says it’s OK.
When you shower, gently wash your incision sites. Then pat the incisions dry. Don’t apply lotions, oils, or creams to the incisions until after they are fully healed.
Don’t raise your arms above breast level for 10 days. And don’t lift, push, or pull anything heavier than 10 pounds for at least 14 days.
Avoid strenuous activity and exercise as directed. Talk to your doctor about light exercise, such as walking, that you can do to maintain your weight until you’re fully healed.
Don’t drive until you are no longer taking prescription pain medicine and your doctor says it’s OK. When riding in a car, carefully position the seatbelt so that it doesn’t compress your breasts.
Be aware that breast swelling may last for 3 to 5 weeks. If advised by your doctor, use a cold pack wrapped in a thin towel to relieve discomfort and control swelling. It’s important not to leave the cold pack on for too long, or your skin could be damaged. Put the pack over your bandages for no more than 20 minutes at a time. Then, leave it off for at least 20 minutes. Repeat this as often as needed during waking hours until swelling starts to improve. Don’t fall asleep with the cold pack on. If you’re not sure how to safely use the cold pack, ask your doctor.
When to call your healthcare provider
Call your healthcare provider if you have any of the following:
Extreme chest pain or trouble breathing (call 911)
A fever of 100.4°F (38°C) or higher, or as directed by your healthcare provider
Bleeding or drainage through the Ace bandage, compression garment, or special bra
Symptoms of infection at an incision site such as increased redness or swelling, warmth, worsening pain, or foul-smelling drainage
Pain that is not relieved by medicine
A lot more soreness, swelling, or bruising on one breast than the other
Breast that is very warm to the touch
Nothing comes out of your drains for more than 6 hours
Pain, swelling, redness, or warmth in your leg, calf, or thigh
Follow-up
You will have follow-up visits so your doctor can see how well you’re healing. If needed, stitches or drains will be removed at one of these visits. Let you doctor know if you have any questions or concerns during your recovery. To maintain the results of your tummy tuck, take steps to avoid gaining weight. Also, call your doctor if you notice any changes in your breasts. This may include injury to the breast or dimpling of the skin of your breast or nipple. If the implants leak or break, they will need to be removed or replaced.
Risks and complications
Risks and possible complications include:
Bleeding or infection
Blood clots
Capsular contracture (scar tissue squeezing the implant)
Excessive scarring on the breast or abdomen
Changes in breast or nipple sensation (short-term or permanent)
Breasts that are not the same shape or size
Persistent pain
Skin color changes
Damage to nerves, muscles, or the lungs
Death of fat cells deep in the skin (fat necrosis)
Rupture or leakage of an implant
Not being happy with cosmetic results
Risks of anesthesia
Updated:
December 02, 2017
Sources:
Breast reconstruction: Preoperative assessment, Up To Date, Breast reconstruction: Prosthetic devices, Up To Date
Reviewed By:
Fraser, Marianne, MSN, RN,Lickstein, David, MD