Tracheoscopy with Bronchoscopy
Tracheoscopy with Bronchoscopy
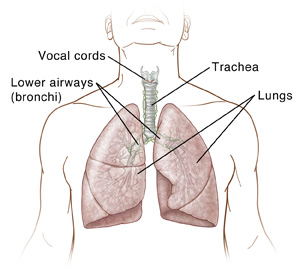
Tracheoscopy with bronchoscopy is a procedure that lets your provider look inside your windpipe (trachea) and down into your lower airways. To do this, a thin, flexible tube (endoscope) is used. It has a tiny camera and light at the end.
Getting ready for your procedure
Follow any instructions from your healthcare provider. Tell your provider about any medicines you are taking. You may need to stop taking all or some of these before the procedure. This includes:
All prescription medicines
Any blood-thinning medicines (anticoagulants)
Over-the-counter medicines such as aspirin or ibuprofen
Street drugs
Herbs, vitamins, and other supplements
Also tell your provider if you smoke or drink alcohol.
During your procedure
The procedure can take up to 45 minutes. You will go home the same day. Before the procedure starts, your throat will be numbed. You may also be given medicine to help you relax. During the procedure:
You may sit upright in a chair that supports your head or lay down on a cushioned table.
The endoscope is gently put into your nose and moved down into your throat, between your vocal cords. It may then be moved into your lower airways. You will need to breathe through your mouth while the endoscope is in place.
The endoscope sends pictures from inside your trachea and lower airways to a video screen. Your provider uses the images to move the scope and look for problems.
If needed, the endoscope can be used to take a small tissue sample (biopsy) from inside your trachea or airways. This sample is sent to a lab for testing.
When the test is done, the endoscope is removed.
After your procedure
Have an adult family member or friend drive you home. Take it easy for the rest of the day. Due to the numbing medicine, swallowing may be hard at first. This may last a few hours. Don’t eat or drink until swallowing returns to normal. Follow any instructions you have been given, such as:
If you smoke, stop for at least 24 hours after the procedure. Smoking will make your throat irritation worse and slow your recovery.
If a biopsy was taken, try not to cough or clear your throat. This will help prevent bleeding. But, it's OK to cough if you need to.
Once you are able to swallow normally, drink plenty of water.
Use throat lozenges as prescribed by your provider.
When to call your healthcare provider
If you are having trouble breathing, call 911 or your local emergency number right away. Don't wait to see if it will get better on its own. This can be a life-threatening emergency.
Call your provider if you have any of the following problems:
Trouble swallowing that doesn’t improve
Fever of 100.4°F (38°C) or higher, or as directed by your healthcare provider
Hoarseness that is not improving
Severe nausea or vomiting
Bloody cough or vomit (you may cough up small amounts of blood, especially if a biopsy was taken)
Follow-up
Within a week or so, your provider will likely see you for a follow-up visit. During this visit, your provider will discuss the results of your procedure and biopsy. You can also discuss any treatments that might be needed.
Risks and possible complications
All procedures have some risk. Possible risks of this procedure include:
Bleeding
Infection
Swollen throat
Breathing problems
Vomiting
Food or fluids going into your airways (aspiration)
Vocal cord paralysis. This is rare.
Updated:
October 13, 2017
Sources:
Tracheal infections associated with tracheostomy tubes and endotracheal intubation in children. UpToDate, Verma, Sunii P., MD. Transnasal Tracheoscopy. The Laryngoscope. 2012; 122 (6): 1326-1330.
Reviewed By:
Blavias, Allen, J., DO,Brown, Kim, APRN