Right Ventricular Assist Device Implantation
Right Ventricular Assist Device Implantation
What is right ventricular assist device (RVAD) implantation?
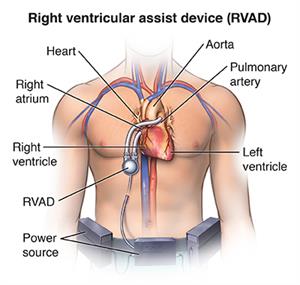
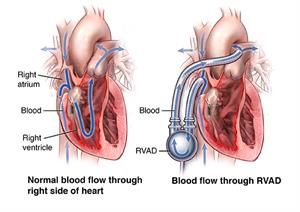
A ventricular assist device helps your heart pump blood when the pumping muscle has become weak. A right ventricular assist device (RVAD) pumps blood from your right ventricle or right atrium into your pulmonary artery and to the lungs.
Your doctor implants the pump close to your heart. The power source is located outside of your body. It is connected to the pump through a small hole in your abdomen. Both the pump and the power source of some temporary ventricular assist devices are located outside of your body. Tubes connect the pump to your heart through small holes in your abdomen.
Your surgeon implants the device during open-heart surgery. During this procedure, he or she redirects the major arteries that take blood in and out of your heart, to the pump. The pump, in turn, pushes the blood through your heart and out to the rest of your body.
Why might I need RVAD implantation?
A ventricular assist device stabilizes your heart function after injury, such as a heart attack. It's also used if you have severe heart failure that does not improve with medicines. It can also keep your heart working while you wait for a heart transplant. This may be called “bridge” therapy. For most people, an RVAD is temporary. Your surgeon usually places it after implanting a left-ventricular assist device (LVAD) or doing another type of heart surgery. Your doctor also uses an RVAD to stabilize your condition during an emergency, while your medical team evaluates your health and the best option for treatment.
What are the risks for RVAD implantation?
RVAD implantation is major surgery and requires general anesthesia (which puts you to sleep). Any general anesthesia carries the risk of heart or brain injury. Major surgery also carries the risk of blood clots forming during or after surgery. These clots can break free and travel to your lungs (pulmonary embolism) or brain (stroke).
Other risks of this surgery include:
- Infection
- Bleeding
- Device failure
- Abnormal heart rhythm
- Endocarditis (an infection of your heart tissue)
- Kidney damage
There may be other risks, depending on your specific medical condition. Be sure to discuss any concerns with your doctor before the procedure.
How do I get ready for RVAD implantation?
If you need an RVAD in an emergency, you will be unable to prepare for it. If your surgery is planned, your doctor might give you a complete evaluation, do special X-rays, blood tests, and other tests to check the health of your lungs and heart. Your doctor may also request an echocardiogram (ultrasound of the heart) and cardiac catheterization. Cardiac catheterization is used to look at circulation through the arteries in the heart muscle and to measure the amount of pressure inside the heart chambers and the lungs.
Additional preparation may include:
- Your doctor will explain the procedure to you and you can ask questions.
- You will be asked to sign a consent form that gives your permission to do the test. Read the form carefully and ask questions if something is unclear.
- You will be asked to fast for 8 hours before the procedure, generally after midnight.
- If you are pregnant or think you could be, tell your doctor.
- Tell your doctor if you are sensitive to or are allergic to any medicines, iodine, latex, tape, or anesthetic agents (local and general).
- Tell your doctor of all medicines (prescription and over-the-counter) and herbal supplements that you are taking.
- Tell your doctor if you have a history of bleeding disorders or if you are taking any anticoagulant (blood-thinning) medicines, aspirin, or other medicines that affect blood clotting. You may be told to stop some of these medicines before the procedure.
- Your doctor may do a blood test to see how long it takes your blood to clot.
- If you smoke, stop smoking as soon as possible before the procedure. This may improve your chances for a successful recovery from surgery and benefit your overall health status.
Based on your medical condition, your doctor may request other specific preparations.
What happens during RVAD implantation?
The operation may take between 4 and 6 hours. Your surgeon may stop your heart during the surgery. In this case, a heart-lung bypass machine will do the work of your heart, keeping oxygen-rich blood flowing throughout your body during surgery. The surgery usually proceeds as follows:
- You will be asked to remove any jewelry or other objects that may interfere with the procedure.
- You will change into a hospital gown and empty your bladder.
- A health professional will start an intravenous (IV) line in your arm or hand. He or she may insert additional catheters in your neck and wrist to monitor the status of your heart and blood pressure, and to take blood samples.
- The anesthesiologist will continuously monitor your heart rate, blood pressure, breathing, and blood oxygen level during the surgery. Once you are sedated, he or she will insert a breathing tube through your throat into your lungs and connect you to a ventilator, which will breathe for you during the surgery.
- A member of the surgery team will insert a catheter into your bladder to drain urine.
- Your doctor will clean the skin over the surgical site with an antiseptic solution.
- Your doctor will make an incision in the front of your chest, down through your chest wall to reach your heart. He or she will insert tubes into your heart, so that a heart-lung bypass machine can keep your blood moving.
- Your doctor will implant the RVAD device into your heart.
- Once the procedure has been completed, your doctor will allow the blood circulating through the bypass machine to re-enter your heart and remove the tubes to the machine.
- Your doctor will insert tubes into your chest to drain blood and other fluids from around the heart. These tubes will be connected to a suction device to drain fluids away from the heart.
- A tube will be inserted through your mouth or nose into your stomach to drain stomach fluids.
- Your doctor will close the incisions with sutures or surgical staples and apply a sterile dressing.
What happens after RVAD implantation?
In the hospital
How long you stay in the hospital will depend on your overall condition after surgery.
- For the first few days, you may be in intensive care where you can be monitored closely until your vital signs have stabilized.
- As you recover, your doctor will remove the tubes that give you nourishment, help you breathe, and drain fluids from your body.
- Your doctor may place temporary pacing wires on your heart during the surgery. He or she will remove these wires once it is determined that your heart rhythm is stable and you no longer need them.
- Physical rehabilitation (cardiac rehab or physical therapy) and pulmonary rehabilitation are important for your long term recovery. You will begin a step-wise program of increasing time and intensity of activity in preparation for going home.
- Healthcare professionals will help you care for your incision, manage pain, and get you up walking.
- A nurse helps you learn how to use and care for the RVAD. Before you leave the hospital, you and your loved ones should be able to use the device correctly and know what to do in emergencies.
At home
Once your doctors feel that you have recovered enough, you will be discharged home. Follow all your instructions for medicines, pain control, diet, activity, and wound care. Make sure to keep all your follow-up appointments. Your doctor might prescribe anticoagulant drugs. These help prevent blood clots from forming. Make sure you understand how to take them and what side effects they might cause.
If you are waiting for a heart transplant, keep in close contact with your transplant center.
Other common instructions after surgery include:
- Walk as much as possible.
- Avoid any heavy lifting. Your surgeon will provide a timeline for certain lifting restrictions.
- Gradually resume normal activities as instructed (ask your doctor about driving, working, and sexual activity). You won’t be able to drive for a period after the surgery to allow for healing of the breastbone (sternum) and muscles of the chest wall.
- Watch your wounds for any sign of swelling, redness, bleeding, or discharge and report these to your medical and surgical team.
- Tell your doctor about any increasing pain, fever, chest pain, or shortness of breath.
- Eat a heart-healthy diet and maintain a healthy weight. Eat foods that are low in salt, cholesterol, and fat. Try to eat fruits, vegetables, and lean meats.
- Don’t smoke or use any other tobacco products including electronic cigarettes.
Next steps
Before you agree to the test or the procedure make sure you know:
- The name of the test or procedure
- The reason you are having the test or procedure
- What results to expect and what they mean
- The risks and benefits of the test or procedure
- What the possible side effects or complications are
- When and where you are to have the test or procedure
- Who will do the test or procedure and what that person’s qualifications are
- What would happen if you did not have the test or procedure
- Any alternative tests or procedures to think about
- When and how will you get the results
- Who to call after the test or procedure if you have questions or problems
- How much will you have to pay for the test or procedure
Updated:
March 22, 2017
Sources:
Short term mechanical circulatory assist devices, Up To Date
Reviewed By:
Fetterman, Anne, RN, BSN,Mancini, Mary, MD