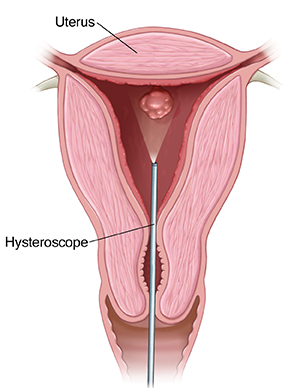
Hysteroscopy
Hysteroscopy
Hysteroscopy is a procedure that is done to see inside your uterus. It can help find the cause of problems in the uterus. This helps your healthcare provider decide on the best treatment. In some cases it can be used to perform treatment. Hysteroscopy may be done in your healthcare provider's office or in the hospital.
Why might I need hysteroscopy?
Hysteroscopy may be done based on the results of other tests. It can help find the cause of problems. These can include:
Unusually heavy or long menstrual periods
Bleeding between periods
Postmenopausal bleeding
Trouble becoming pregnant (infertility) or carrying a pregnancy to term
To locate an IUD (intrauterine device)
To perform sterilization
What are the risks and complications of hysteroscopy?
Problems with the procedure are rare. But all procedures have risks. Risks of hysteroscopy include:
Infection
Bleeding
Tearing of the uterine wall
Damage to internal organs
Scarring of the uterus
Fluid overload
Problems with anesthesia, the medicine that prevents pain during the procedure
How do I get ready for hysteroscopy?
Tell your healthcare provider if you have any health problems. These include diabetes, heart disease, or bleeding problems.
Tell your healthcare provider about all the medicines you take. This includes any over-the-counter medicines, prescription medicines, vitamins, herbs, or supplements.
You may be told not to use vaginal creams or medicine. And you may be told not to have sex or wash out your vagina (douche).
You may be told not to eat or drink the night before the procedure.
You may be tested for pregnancy and infection.
You may be asked to sign a consent form.
You may be given a pain reliever to take an hour before the procedure. This helps relieve cramping that may occur.
What happens during a hysteroscopy?
You’ll lie on an exam table with your feet in stirrups.
You may be given general anesthesia or medicines to help you relax or sleep. In some cases, an IV (intravenous) line will be put into a vein in your arm or hand. This line is then used to give fluids and medicines.
A tool called a speculum is inserted into the vagina to hold it open. A tool called a dilator may be used to widen the cervix.
Numbing medicine may be applied to the cervix.
A long, thin lighted tube (hysteroscope) is inserted through the vagina and into the uterus. It is used to see inside the uterus. Images of the uterus are viewed on a monitor.
A gas or fluid may be injected into the uterus to expand it.
Other tools may be put through the hysteroscope. These are used to take tissue samples, remove growths, or place implants for the purpose of sterilization.
What happens after hysteroscopy?
You may have cramps and bleeding for 24 hours after the procedure. This is normal. Use pads instead of tampons.
Don't douche or use tampons until your healthcare provider says it’s OK.
Don't use any vaginal medicines until you are told it’s OK.
Ask your healthcare provider when it’s OK to have sex again.
When should I call my healthcare provider?
Call your healthcare provider if you have:
Heavy bleeding (more than 1 pad an hour for 2 or more hours)
A fever of 100.4°F (38.0°C) or higher, or as directed by your provider
Increasing belly (abdominal) pain or soreness
Bad-smelling discharge
Follow-up care
Schedule a follow-up visit with your healthcare provider. Based on your test results, you may need more treatment. Be sure to follow instructions and keep your appointments.
Updated:
December 31, 2017
Sources:
Haney, AF, Danforths Obstetrics and Gynecology (2008); 10th ed., Van Leeuwen, AM, Davis's Comprehensive Handbook of Laboratory and Diagnostic Tests with Nursing Implications (2015), 6th ed.
Reviewed By:
Sacks, Daniel, MD, FACOG,Goode, Paula, RN, BSN, MSN