Breast Reduction Surgery
Breast Reduction Surgery
Preparing for surgery
Prepare for the surgery as you have been told. In addition:
Tell your healthcare provider about any recent health conditions and all medicines you take. This includes herbs and other supplements. It also includes any blood thinners, such as warfarin, clopidogrel, or daily aspirin. You may need to stop taking some or all of them before surgery.
Follow any directions you are given for not eating or drinking before surgery.
Don't smoke before surgery. Your healthcare provider may delay your surgery if you are smoking. Smoking reduces the blood flow in the skin and nipples, and increases the risk of wound healing complications.
The day of surgery
The surgery takes about 3 to 6 hours. You may go home the same day. Or you may stay overnight.
Before the surgery begins
An IV line is put into a vein in your arm or hand. This line delivers fluids and medicines.
You will be given medicine to keep you pain free during surgery. This may be general anesthesia, which puts you into a state like deep sleep. (A tube may be inserted into your throat to help you breathe.) Or you may have sedation, which makes you relaxed and sleepy. If you have sedation, local anesthesia will be injected to numb the area being worked on. The anesthesiologist will discuss your options with you.
During the surgery
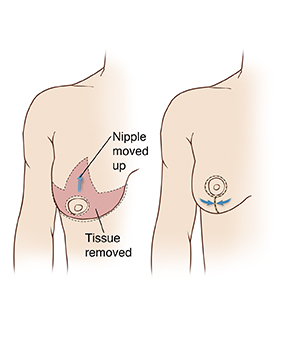
The healthcare provider makes one or more incisions in your breast. Incisions are mostly made around the areola, but extend down under your breast as well. You and your healthcare provider will have discussed incision sites before the surgery.
The healthcare provider removes fat, tissue, and skin from the breast. In some cases, fat is removed using liposuction. This involves inserting a cannula (hollow tube) into the breast. A special vacuum pulls fat through the cannula.
If needed, the areola and nipple are removed and positioned higher on the breast. To reduce the size of the areola, excess skin is removed. The areola is then stitched (sutured) into place.
The process is repeated on the other breast.
The incisions are closed with sutures (stitches), surgical glue, or both. A tube (drain) may be placed into the incisions before they are closed. This drains excess fluid as the wound begins to heal.
After the surgery
You will be taken to a room to wake up from the anesthesia. You may feel sleepy and nauseated. If a breathing tube was used, your throat may be sore at first. You will be given medicine to control pain. When you’re ready, you will be able to go home with an adult family member or friend. Or, you may be moved to a room to stay overnight.
Recovering at home
Once home, follow any instructions you are given. Your healthcare provider will tell you when you can return to your normal routine. During your recovery:
Take any prescribed medicines exactly as directed.
Wear the special bra or bandage you were given before discharge as directed by your healthcare provider.
Care for your incisions and the dressing (bandage) over them as instructed by your healthcare provider.
Follow your healthcare provider’s guidelines for showering. Don't swim, take a bath, use a hot tub, or do other activities that cause the incisions to be covered with water until your healthcare provider says it’s OK.
When you shower, gently wash your incision sites. Then pat the incisions dry. Don’t apply lotions, oils, or creams to the incisions until after they are fully healed.
Don’t raise your arms above breast level for 10 days. And don’t lift, push, or pull anything heavier than 10 pounds for at least 7 days.
Don’t drive until you are no longer taking prescription pain medicine and your healthcare provider says it’s OK. When riding in a car, carefully position the seatbelt so that it doesn’t compress your breasts.
Be aware that breast swelling may last for 3 to 5 weeks. If advised by your healthcare provider, use a cold pack wrapped in a thin towel to relieve discomfort and control swelling. It’s important not to leave the cold pack on for too long, or your skin could be damaged. Put the pack over your bandages for no more than 20 minutes at a time. Then, leave it off for at least 20 minutes. Repeat this as often as needed during waking hours until swelling starts to improve. Don’t fall asleep with the cold pack on. If you’re not sure how to safely use the cold pack, ask your healthcare provider.
When to call your healthcare provider
Be sure you have a contact number for your healthcare provider. After you get home, call your healthcare provider right away if you have any of the following:
Extreme chest pain or trouble breathing (call 911)
A fever of 100.4°F (38°C) or higher, or as directed by your healthcare provider
Bleeding or drainage through the special bra or bandage
Symptoms of infection at an incision site, such as increased redness or swelling, warmth, worsening pain, or foul-smelling drainage
Pain that is not relieved by medicine or pain that gets worse
Much more soreness, swelling, or bruising on one breast that the other
Breast that is very warm to the touch
Follow-up
You will have follow-up visits so your healthcare provider can see how well you’re healing. If needed, stitches or drains will be removed at one of these visits. If you have any questions or concerns about your recovery, let your healthcare provider know.
Risks and complications
Risks and possible complications include:
Bleeding or infection
Blood clots
Excessive internal or external scarring
Breasts that are asymmetric (not the same shape and/or size)
Breasts that are too firm
Changes in breast or nipple sensation (temporary or permanent)
Damage to nerves, muscles, or blood vessels
Persistent pain
Death of fat cells deep in the skin (fat necrosis)
Inability to breastfeed
Not happy with cosmetic result
Risks of anesthesia. The anesthesiologist will discuss these with you.
Updated:
August 08, 2018
Sources:
Breast Reduction. UpToDate
Reviewed By:
Fraser, Marianne, MSN, RN,Image reviewed by StayWell medical illustration team.,Lickstein, David, MD