Your Child's Nasogastric Tube: Flushing the Tube
Your Child's Nasogastric Tube: Flushing the Tube
Your child is going home with a nasogastric (NG) feeding tube in place. This is a soft thin tube inserted through your child’s nose down into the stomach. It sends liquid food directly to the stomach. You’ll need to flush your child’s tube regularly to keep it from getting clogged. You were shown how to do this before your child was discharged from the hospital. This sheet will help you remember those steps at home. If you need more help, talk with the hospital about how to arrange a home health nurse to help you.
Keep in mind that there are many types of NG tubes and syringes. Your child’s NG tube and supplies may look or work differently from what are described and shown here. Make sure to follow the instructions given by your child’s healthcare provider or home health nurse.
Contact information to keep handy
Ask for phone numbers to call if you need help. Also, make sure you have the phone number for your child’s medical supply company. You’ll need to order more supplies for your child in the future. Write all of these phone numbers below.
Healthcare provider phone number: ____________________________________
Home health nurse phone number: _____________________________________
Medical supply company phone number: __________________________________
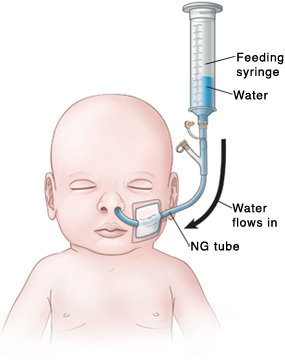
Flushing the tube for bolus feeding using a syringe
Flush your child’s NG tube after each feeding, or as instructed by your child’s healthcare provider or home health nurse.
The supplies you'll need are:
Feeding syringe
Water
Follow these steps:
Wash your hands with soap and water.
Make sure the feeding syringe is already connected to the NG tube.
Pour water into the syringe. Let it run through the NG tube by gravity.
If the water flows too slowly or doesn’t flow at all, place the plunger in the syringe. Gently push the plunger a small amount. This can help remove anything that is blocking or clogging the NG tube. Do not push hard, and do not push the plunger all the way into the syringe. Changing your child’s position so that he or she is lying down or sitting upright may also improve the flow.
Disconnect the syringe from the NG tube when the flushing is done.
Close the feeding port cap of the NG tube.
Additional instructions:
________________________________________________________________________
________________________________________________________________________
________________________________________________________________________
________________________________________________________________________
Flushing the tube for bolus feeding or continuous feeding using a pump
Flush your child’s NG tube after each bolus feeding, or as instructed by your child’s healthcare provider or home health nurse. With continuous feeding, you may only need to flush the tube after the last daily feeding.
The supplies you’ll need are:
5 to 10 ml syringe
Water
|
|
|
|
Follow these steps:
Wash your hands with soap and water.
Make sure the pump is in the STOP/OFF mode.
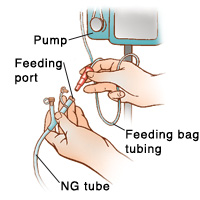
Make sure the clamp on the feeding bag tubing is closed.
Disconnect the feeding bag tubing from the NG tube.
Put the tip of the empty syringe in water.
Draw up 5 to 10 ml of water.
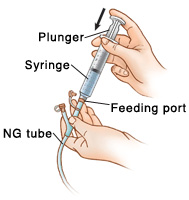
Connect the syringe to the feeding port of the NG tube.
Gently push the plunger all the way into the syringe.
Disconnect the syringe from the NG tube when the flushing is complete.
Close the feeding port cap of the NG tube.
Additional instructions:
________________________________________________________________________
________________________________________________________________________
________________________________________________________________________
________________________________________________________________________
When to call the healthcare provider
Contact the healthcare provider right away if your child has any of the below:
Trouble breathing
Redness, swelling, leakage, sores, or pus on the skin around the tube site
Blood around the tube, or in your child’s stool or vomit
Coughing, choking, or vomiting while feeding
Vomiting between feedings
Belly that looks bloated or feels hard when gently pressed
Diarrhea or constipation
Fever 100.4°F (38°C) or higher, or as directed by your healthcare provider
Updated:
October 08, 2017
Sources:
Bankhead, R. Enteral Nutrition Practice Recommendations. Journal of Parenteral and Enteral Nutrition (2009); 33(2); pp. s122-s167, Narins, Brigham. The Gale Encyclopedia of Nursing and Allied Health. 2013. 3; 3393-3395.
Reviewed By:
Adler, Liora C., MD,Freeborn, Donna, PhD, CNM, FNP