When Your Child Has Irritable Bowel Syndrome
When Your Child Has Irritable Bowel Syndrome
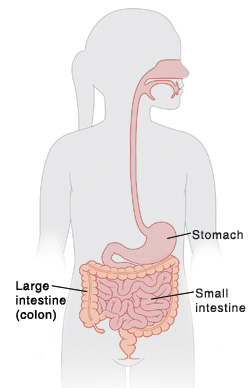
Irritable bowel syndrome (IBS) is a relatively common condition in children. It affects your child’s digestive tract. This is where food is broken down to give your child energy and to help him or her grow. No one knows exactly what causes IBS. It may be a result of the nerves in the intestine being overly sensitive, causing spasm and changes in the way the intestine contracts. IBS may come and go, but there are things you can do to help your child feel better.
What causes IBS?
The exact cause of IBS is not known. But it may involve the nerves and muscle movement that passes food and liquids through the digestive tract. If food passes too quickly, the colon can’t absorb enough water. This can cause painful cramping and watery stools (diarrhea). If food passes too slowly, too much water is absorbed. This can make the stool dry and hard (constipation).
What are IBS symptoms?
Symptoms of IBS can vary from child to child. Common symptoms include:
Painful cramps
Gas
Bloating
Diarrhea
Constipation
How is IBS diagnosed?
To diagnose IBS, the healthcare provider will start by asking about your child’s medical history. A physical exam will be performed. The healthcare provider may also order some tests to rule out other digestive problems. These may include bloodwork, stool tests, radiology studies, and possibly scopes, inserting a flexible tube through the mouth or anus to evaluate the inside of the intestine.
How is IBS treated?
There is no cure for IBS. But your child’s symptoms can be managed. The healthcare provider might prescribe medicine for symptoms such as diarrhea and constipation. There are also things you and your child can do at home to manage IBS:
Help your child avoid foods or drinks that seem to make symptoms worse. Certain substances may irritate your child’s digestive tract. These substances can be different for each child. Write down what your child is eating and drinking and what symptoms happen. Use this list as a guideline to help your child avoid irritating foods.
Make sure your child drinks plenty of water. Ask the healthcare provider how much water your child should drink each day. If your child is having IBS symptoms, limit drinks with caffeine and carbonation.
Increase your child’s fiber intake, if told to by the healthcare provider. Fiber is found in many plant foods. It helps stool keep enough water, so it passes easily through the colon. Your child can get more fiber through food or prescribed fiber supplements.
Have your child eat small meals. If eating triggers your child's symptoms, frequent small meals may be beneficial.
Help your child reduce stress and anxiety. While stress itself may not cause IBS, it can make symptoms feel worse. Help your child identify sources of stress. Talk with your child about ways to handle stressful situations. A counselor or therapist can teach your child ways to manage stress, such as medicine or other relaxation methods.
Encourage physical activity. Physical activity is a great way to relieve stress. It may even help ease constipation and other IBS symptoms. So encourage your child to play and be active every day.
When to call the healthcare provider
Even if your child’s symptoms are under control, contact the healthcare provider if you notice:
Weight loss
Blood in your child’s stool
Vomiting
Fever over 100.4°F (38.0°C) or higher, or as directed by your healthcare provider
Fear of using the toilet, at home or at school
Withdrawal from friends and family or prolonged sadness (which could be signs of depression)
Updated:
January 20, 2018
Sources:
An Evidence-Based Systematic Review on the Management of Irritable Bowel Syndrome American College of Gastroenterology Task Force and Irritable Bowel Syndrome. Brandt L. The American Journal of Gastroenterology. 2009;104(1):s1-s35., Chronic abdominal pain in children and adolescents: Approach to the evaluation. UpToDate, Common Gastrointestinal Symptoms: Irritable Bowel Syndrome. Fashner J. FP Essent. 2013;413:16-23., Functional abdominal pain in children and adolescents: Management. UpToDate, Subtypes of Irritable Bowel Syndrome in Children: Prevalence at Diagnosis and at Follow-Up. Giannetti E. The Journal of Pediatrics. 2014;164(5):1099.
Reviewed By:
Freeborn, Donna, PhD, CNM, FNP,Lehrer, Jenifer, MD