When Your Child Has Hand, Foot, and Mouth Disease
When Your Child Has Hand, Foot, and Mouth Disease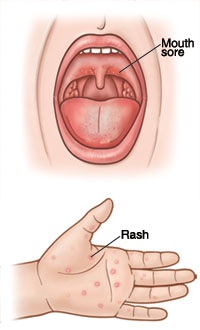
Hand, foot, and mouth disease (HFMD) is a common viral infection in children. It can cause mouth sores and a painless rash on the hands, feet, or buttocks. HFMD can be easily spread from one person to another. It occurs more often in children younger than 10 years old, but anyone can get it. HFMD is often mistaken for strep throat because the symptoms of both conditions are similar. HFMD can cause some discomfort, but it’s not a serious problem. Most cases can easily be managed and treated at home.
What causes hand, foot, and mouth disease?
HFMD is usually caused by the coxsackievirus. It can also be caused by other viruses in the same family as coxsackievirus. Your child may have caught HFMD in one of the following ways:
Breathing infected air (the virus can enter the air when an infected person coughs, sneezes, or talks).
Contact with items contaminated with stool from an infected person. Contamination can occur when an infected person doesn’t wash his or her hands after having a bowel movement or changing a diaper.
Contact with fluid from the blisters that are part of the rash (this type of transmission is rare).
What are the symptoms of hand, foot, and mouth disease?
Symptoms usually appear 24 to 72 hours after exposure. They include:
Rash (small, red bumps or blisters on the hands, feet, or buttocks)
Mouth sores that often occur on the gums, tongue, inside the cheeks, and in the back of the throat (mouth sores may not occur in some children)
Sore throat
A nonspecific rash over the rest of the body
Fever
Loss of appetite
Pain when swallowing
Drooling
How is hand, foot, and mouth disease diagnosed?
HFMD is diagnosed by how the rash and mouth sores look. To get more information, the healthcare provider will ask about your child’s symptoms and health history. He or she will also examine your child. You will be told if any tests are needed to rule out other infections.
How is hand, foot, and mouth disease treated?
There is no specific treatment for HFMD, but there are things you can do at home to help relieve some symptoms. The illness generally lasts about 7 to 10 days. Your child is no longer contagious 24 hours after the fever is gone.
Mouth pain
Unless your child’s healthcare provider has prescribed another medicine for mouth pain, give your child ibuprofen or acetaminophen to treat pain or discomfort. Talk with your child's provider about dosing instructions and when to give the medicine (schedule). Do not give ibuprofen to an infant age 6 months or younger. Do not give aspirin to a child with a fever. This can put your child at risk of a serious illness called Reye syndrome.
Liquid antacid can be used 4 times per day to coat the mouth sores for pain relief. Talk with your child's provider about how much and when to give the medicine to your child:
Children over age 4 can use 1 teaspoon (5ml) as a mouth rinse after meals.
For children under age 4, a parent can place 1/2 teaspoon (2.5ml) in the front of the mouth after meals. Avoid regular mouth rinses because they may sting.
Diet
Follow a soft diet with plenty of fluids to prevent fluid loss (dehydration). If your child doesn't want to eat solid foods, it's OK for a few days, as long as he or she drinks plenty of fluids.
Cool drinks and frozen treats (such as sherbet) are soothing and easier to take.
Avoid citrus juices (such as orange juice or lemonade) and salty or spicy foods. These may cause more pain in the mouth sores.
When to seek medical care
Call the child's provider if your otherwise healthy child has any of the following:
A mouth sore that doesn’t go away within 14 days
Increased mouth pain
Trouble swallowing
Neck pain
Chest pain
Trouble breathing
Weakness
Lack of energy
Signs of infection around the rash or mouth sores (pus, drainage, or swelling)
Signs of dehydration (very dark or little urine, excessive thirst, dry mouth, dizziness)
A fever ((see fever and children section below)
A seizure
Fever and children
Always use a digital thermometer when checking your child’s temperature. Never use mercury thermometers.
For infants and toddlers, be sure to use a rectal thermometer correctly. A rectal thermometer may accidentally poke a hole in (perforate) the rectum. It may also pass on germs from the stool. Always follow the product maker’s instructions for proper use. If you don’t feel comfortable taking a rectal temperature, use a different method. When you talk to your child’s healthcare provider, tell him or her which type of method you used to take your child’s temperature.
Here are guidelines for fever temperature. Ear temperatures aren’t accurate before 6 months of age. Don’t take an oral temperature until your child is at least 4 years old.
Infant under 3 months old:
Ask your child’s healthcare provider how you should take the temperature.
Rectal or forehead (temporal artery) temperature of 100.4°F (38°C) or higher, or as directed by the provider.
Armpit (axillary) temperature of 99°F (37.2°C) or higher, or as directed by the provider.
Child age 3 to 36 months:
Rectal, forehead (temporal artery), or ear temperature of 102°F (38.9°C) or higher, or as directed by the provider.
Armpit temperature of 101°F (38.3°C) or higher, or as directed by the provider.
Child of any age:
Repeated temperature of 104°F (40°C) or higher, or as directed by the provider.
Fever that lasts more than 24 hours in a child under 2 years old, or for 3 days in a child 2 years or older.
How can hand, foot, and mouth disease be prevented?
Follow these steps to keep your child from passing HFMD on to others:
Teach your child to wash his or her hands with soap and warm water often. Handwashing is especially important before eating or handling food, after using the bathroom, and after touching the rash. A child is very contagious during the first week of the illness and he or she can still be contagious for days to weeks after the illness resolves.
Your child should remain at home while he or she is sick with hand, foot, and mouth disease. Discuss with your child's health care provider how long you should keep your child from attending school or daycare or playing with others.
Do not allow your child to share cups, utensils, napkins, or personal items such as towels and toothbrushes with others.
Updated:
April 04, 2018
Sources:
Hand, foot, and mouth disease and herpangina: An overview, Up To Date, Up To Date. Epidemiology, Pathogenesis, Treatment, and Prevention of Enterovirus and Parechovirus Infections
Reviewed By:
Image reviewed by StayWell medical illustration team.,Lentnek, Arnold, MD,Turley, Ray, BSN, MSN