When Your Child Has Gastrointestinal (GI) Bleeding
When Your Child Has Gastrointestinal (GI) Bleeding
Blood in your child’s vomit or stool can be a sign of gastrointestinal (GI) bleeding. GI bleeding can be scary for you and your child. Many times, the cause of the bleeding is not serious. Still, your child should ALWAYS be seen by a healthcare provider if GI bleeding happens.
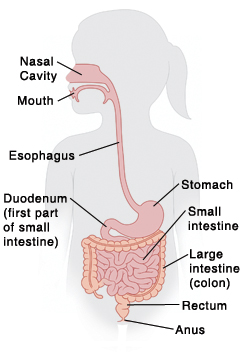
The GI tract
The GI tract is the path that food travels through the body. Food passes from the mouth down the esophagus (the tube from the mouth to the stomach). Food begins to break down in the stomach. It then moves through the duodenum, the first part of the small intestine. Nutrients are absorbed as food travels through the small intestine. What is left passes into the large intestine (colon) as waste. The colon removes water from the waste. Waste continues from the colon to the rectum (where stool is stored). Waste then leaves the body through the anus.
What causes GI bleeding?
Your child’s GI bleeding may have been caused by many different problems. These vary depending on your child's age and where you live. Some of the more common ones include:
Nosebleeds
Cuts or scrapes in the mouth or throat
Infection (bacteria, viruses, parasites)
Food allergies
Medicines
Ulcer (sore on the lining of the GI tract)
Inflammation (swelling or irritation of the lining of the GI tract)
Polyps (growths of tissue)
Abnormal pouches in part of the GI tract
Small tears (fissures) in the anus (common in children with constipation)
Hemorrhoids (swollen blood vessels in the rectum)
Blood in stool: How is the problem diagnosed?
If blood is coming out with your child’s stool, it may signal a lower digestive tract problem. Bleeding from the lower GI tract can be bright red, or it may look dark and tarry. The healthcare provider will start by examining your child and asking questions. Some tests may be ordered. These tests may include:
Blood tests
Hemoccult. A test that checks your child’s stool for blood.
Stool cultures. Tests that check your child’s stool for bacteria or parasites.
X-ray, ultrasound, MRI, or CT scan. Tests that take pictures of the digestive tract.
Colonoscopy or sigmoidoscopy. A test during which a flexible tube with a camera is inserted through the anus into the rectum to view the inside of your child’s colon. This lets the healthcare provider do a biopsy (take a tiny tissue sample).
Capsule study. A wireless camera that is swallowed and sends pictures of the small intestine to a monitor. The pictures are then uploaded to a computer for evaluation. The capsule is passed in the stool and flushed.
Blood in vomit: How is the problem diagnosed?
If your child is vomiting blood, it may signal an upper digestive tract problem. The healthcare provider may order certain tests, such as:
Endoscopy. A test during which a flexible tube with a camera is inserted through the mouth and throat to see inside the upper GI tract. This lets the healthcare provider do a biopsy (take a tiny tissue sample).
X-ray, ultrasound, or CT scan. Tests that take pictures of the digestive tract.
Upper GI series. X-rays of the upper part of the GI tract taken from inside the body.
When to call the healthcare provider
GI bleeding can sometimes be a sign of a serious problem. Call the healthcare provider right away if you notice any of the following in your child:
Bleeding from the mouth or anus that can’t be stopped right away
Fever over 100.4°F (38°C) or higher, or as directed by your healthcare provider
Child is unresponsive or lethargic (acts very sleepy)
Child is inconsolable (cannot be calmed or soothed)
Child is bleeding and becomes lightheaded or dizzy
Dehydration. Symptoms include dry mouth, extreme thirst, no tears when crying, fewer than 6 wet diapers in a day or no urination in 6 hours, being fussy or upset.
Updated:
March 21, 2017
Sources:
Approach to upper gastrointestinal bleeding in children. UpToDate, Diagnosis and Management of Upper Gastrointestinal Bleeding in Children. Owensby S. Journal of the American Board of Family Medicine. 2015;28:134-45., Diagnostic approach to lower gastrointestinal bleeding in children. UpToDate, The Young Child With Lower Gastrointestinal Bleeding Or Intussusception. Lumba A. Pediatric Emergency Medicine Practice. 2012;9(1):1-16.
Reviewed By:
Freeborn, Donna, PhD, CNM, FNP,Lehrer, Jenifer, MD