Testicular Cancer: Introduction
Testicular Cancer: Introduction
What is cancer?
Cancer is when cells in the body change and grow out of control. Your body is made up of tiny building blocks called cells. Normal cells grow when your body needs them, and die when your body does not need them any longer.
Cancer is made up of abnormal cells that grow even though your body doesn't need them. In most cancers, the abnormal cells grow to form a lump or mass called a tumor. If cancer cells are in the body long enough, they can grow into (invade) nearby areas. They can even spread to other parts of the body (metastasis).
What is testicular cancer?
Cancer that starts in a testicle is called testicular cancer. It is one of the most curable forms of cancer.
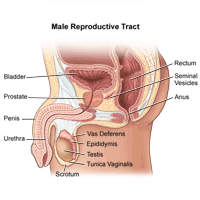
Understanding the testicles
The testicles are the male sex glands and are part of the male reproductive system. Testicles are also called testes or gonads. They are located behind the penis in a pouch of skin (scrotum).
The testicles make sperm. Sperm are the male cells needed to fertilize a female egg cell. The testicles also make several male hormones, including testosterone. These hormones control the development of the reproductive organs. They also control other features such as body and facial hair and a lower voice.
What are the types of testicular cancer?
Germ cell tumors
More than 90% of testicular cancers begin in a type of cell in the testicles called a germ cell. These are the cells that give rise to sperm. There are 2 main types of germ cell tumors: seminomas and nonseminomas. These 2 types occur almost equally. Many testicular cancers have both seminoma and nonseminoma cells. These are called mixed germ cell tumors.
Seminomas
Seminomas tend to grow more slowly. They often respond very well to treatment. There are 2 types:
Classical (typical). More than 90% of seminomas are classical. These are usually found in men between ages 25 and 45.
Spermatocytic. These tend to occur later in life. The average age of diagnosis is 65.
Nonseminomas
These grow faster than seminomas. They tend to occur in men between their late teens and early 30s.
There are 4 main subtypes:
Embryonal carcinomas. This type tends to grow and spread quickly. Under a microscope, these tumors look like tissue in early embryos.
Yolk sac carcinomas. This is the most common form of germ cell tumor in infants and boys. These are usually treated successfully when found in children. They can be harder to treat in adults.
Choriocarcinomas. This type is very rare and tends to grow fast. It often spreads quickly to other parts of the body.
Teratomas. Under a microscope these tumors look like the 3 layers of tissue in a growing embryo. They are rarely the only type of cell in a nonseminoma.
Most nonseminomas are a mix of different subtypes. Sometimes seminoma cells are mixed in as well.
Stromal tumors
The stroma are tissues in the testicles that make hormones or support other tissues. Stromal tumors start in these tissues. There are 2 main types:
Leydig cell tumors. These tumors develop from cells that normally make hormones.
Sertoli cell tumors. These tumors develop from cells that support and nourish germ cells.
Overall, stromal cell tumors make up less than 5% of all adult cases of testicular cancer. But they are found in up 20% of all childhood cases.
Secondary testicular tumors
Secondary tumors are tumors that start in another part of your body and spread to your testicles. For example, some kinds of lymphoma, a cancer of the lymph nodes, can spread to the testicles. In men ages 50 and older, secondary testicular cancer that begins as lymphoma is more common than tumors that start in the testicles. Other cancers that may spread to your testicles include lung, melanoma, kidney, and prostate cancer.
Talk with your healthcare provider
If you have questions about testicular cancer, talk with your healthcare provider. He or she can help you understand more about this cancer.
Updated:
January 11, 2018
Reviewed By:
Alteri, Richard, MD,Gersten, Todd, MD