Pituitary Tumor: Frequently Asked Questions
Pituitary Tumor: Frequently Asked Questions
What is the pituitary gland?
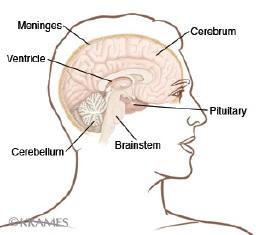
The pituitary gland is a small gland located inside the skull, just below the brain. It is behind the nasal sinuses and above the roof of the mouth. The pituitary gland connects to a part of the brain called the hypothalamus. Together, the hypothalamus and the pituitary control the body’s production of many important hormones.
The pituitary gland sits in a tight, bony space. It has little room to grow or expand when swollen, or if there is a tumor.
The pituitary gland controls most of the body’s gland activity. This includes the adrenal and thyroid glands. It also includes sex hormone production. In women, it controls egg production (ovulation). In men, it controls testosterone and sperm production in the testicles. It is also believed to be the main control gland of the body’s neuroendocrine system.
The pituitary gland has 2 parts: the back part (posterior pituitary) and the front part (anterior pituitary). The back part makes the following hormones:
Vasopressin, also called ADH (antidiuretic hormone). This hormone lets the kidneys keep healthy amounts of water and not send it all out in urine. It can also raise blood pressure by causing blood vessels to narrow or tighten.
Oxytocin. This female hormone helps the uterus contract during childbirth. It also helps the breasts release milk when a woman is nursing.
The front part of the pituitary makes several kinds of hormones. These hormones control other glands all over the body:
Growth hormone (somatotropin). This hormone helps a child's body grow, especially during the teen years (puberty). Adults don’t normally make a lot of this hormone.
Thyroid-stimulating hormone (TSH or thyrotropin). This hormone helps the thyroid gland to grow, and to make and release the thyroid hormone. The thyroid hormone controls how your body turns food into energy (metabolism).
Adrenocorticotropic hormone (ACTH). This hormone stimulates the adrenal gland so that it can make certain steroid hormones.
Luteinizing hormone (LH) and follicle-stimulating hormone (FSH), also called gonadotropins. In women, these hormones control the menstrual cycle ovulation. In men, they control testosterone and sperm production.
Prolactin. This hormone helps make milk in a woman’s breast. It’s not clear how it works in men.
What are pituitary tumors?
A pituitary tumor is a tumor that begins in the pituitary gland. Most pituitary tumors are not cancer. Cancerous pituitary tumors are very rare. They are so rare that cancer agencies don’t keep track of how many people get them each year. Noncancerous (benign) pituitary tumors are also rare. About 10,000 people in the U.S. get them each year.
What are adenomas?
There are different kinds of pituitary tumors. Most of these tumors are not cancer. They are called adenomas. They don’t usually spread outside the pituitary gland. But they can greatly affect your health. They can push on nearby parts of the brain. And they may send out excess hormones.
Pituitary adenomas are grouped in 2 ways: by their size and by the kind of hormone they make.
Size. Pituitary adenomas are grouped into 2 sizes:
Microadenomas are tumors that are smaller than 1 centimeter (cm).
Macroadenomas are tumors that are bigger than 1 cm.
Both kinds of tumors can either make hormones (functional) or not make hormones (nonfunctional). Most pituitary tumors are functional. This means they make excess hormones.
Hormones. Pituitary adenomas are also grouped by whether they make excess hormones. Those that do are called functional. They are then grouped by the type of hormone they make. Functional adenomas include tumors that:
Make prolactin
Make growth hormone
Make ACTH (corticotropin)
Make gonadotropin (LH and FSH)
Make thyroid-stimulating hormone (TSH and thyrotropin)
Some tumors make more than 1 type of hormone. A pituitary adenoma that doesn’t make excess hormones is called nonfunctional.
What are the risk factors for pituitary tumors?
Certain factors can make 1 person more likely to get a pituitary tumor than another person. These are called risk factors. Doctors are not sure exactly what causes pituitary tumors. Most people who get a pituitary tumor have no known risk factors.
The only proven risk factor for a pituitary tumor is a rare condition called MEN1 (multiple endocrine neoplasia, type 1). MEN1 syndrome is hereditary. This means it is passed down from parent to child. People with MEN1 have a high risk of getting tumors of the pituitary, the parathyroid, and the pancreas. If a parent carries the gene change for this rare syndrome, the child has a 50% change of getting MEN1.
What are the symptoms of pituitary tumors?
Both noncancer and cancerous pituitary tumors can cause symptoms. These may include:
Double or blurred vision
Loss of side (peripheral) vision
Sudden loss of sight
Headaches
Dizzy spells
Fainting
Upset stomach (nausea)
Weakness
Unwanted weight loss or gain
Loss of menstrual periods
Men having problems keeping an erection (erectile dysfunction)
Loss of interest in sex
These symptoms can also be signs of other problems. If you have these symptoms, see your healthcare provider.
Pituitary tumors that affect hormones may cause many different symptoms linked to high hormone levels and production. These symptoms will be different in children than in adults. For example, in children, tumors that make growth hormone may cause:
Rapid growth
Joint pain
Excessive sweating
Being abnormally tall (known as gigantism)
In adults, tumors that make growth hormone may cause:
Increase in hat, shoe, or ring size caused by growth of skull, hands, or feet
Deeper voice
Change in facial structure
Joint pain
Excessive sweating
Headache
Heart disease
High blood pressure
Diabetes
Kidney stones
Other more rare kinds of pituitary tumors cause other symptoms. If you have any unusual symptoms, see your healthcare provider.
How are pituitary tumors treated?
In most cases, pituitary tumors are treated using surgery, radiation therapy, or medicines that block the tumor from making hormones.
Surgery. The goal of surgery is to remove the whole tumor from the pituitary gland. Sometimes the whole pituitary gland will have to be removed. If this is needed, medicines can provide the hormones that the pituitary gland used to make.
Radiation. The goal of radiation therapy is to kill the tumor by using X-rays. This treatment is often used when someone can’t have surgery. Or it may be used when a tumor can’t entirely be removed in surgery. It can also be used if the tumor comes back after surgery.
Hormone-blocking medicine. This treatment stops the tumor from making excess hormones that are causing problems in other parts of the body. In some kinds of pituitary tumors, this may be the only treatment needed.
Researchers are always finding new ways to treat pituitary tumors. These new methods are tested in clinical trials. Before starting treatment, ask your doctor if there are any clinical trials you should consider.
What are clinical trials?
Clinical trials are studies of new kinds of cancer treatments. Researchers conduct clinical trials to learn about how well new treatments work and what their side effects are. If these new treatments look promising, they are then compared to the current treatment. People who take part in these studies may be able to try new treatments before the FDA approves them. They also help doctors better understand cancer and help future cancer patients.
Should everyone get a second opinion?
Many people with cancer get a second opinion from another doctor. There are many reasons to get a second opinion, such as:
You are not comfortable with the treatment decision
Your type of cancer is rare
There are different ways to treat the cancer
You are not able to see a cancer expert
How can I get a second opinion?
There are many ways to get a second opinion:
Your healthcare provider may be able to recommend a specialist. This may be a surgeon, medical oncologist, or radiation oncologist. Sometimes these doctors work together at cancer centers or programs.
The Cancer Information Service (800-4-CANCER or 800-422-6237) can tell you about treatment facilities, including cancer centers and other programs supported by the National Cancer Institute.
You can get names of doctors from your local medical society, a nearby hospital, a medical school, or a local cancer advocacy group. You can also ask other people who have had the same type of cancer.
Updated:
March 21, 2017
Sources:
National Comprehensive Cancer Network: NCCN Clinical Practice Guidelines Neuroendocrine Tumors Version I.2014
Reviewed By:
MMI board-certified, academically affiliated clinician,Moloney Johns, Amanda, PA-C, MPAS, BBA