Understanding Deep Vein Thrombosis
Understanding Deep Vein Thrombosis
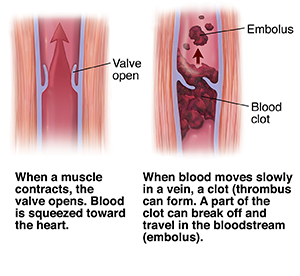
Deep vein thrombosis (DVT) is a condition in which a blood clot or thrombus forms in a deep vein. A blood clot is most common in the leg, but can develop in a large vein deep inside the leg, arm, or other part of the body. Part of the clot called an embolus can separate from the vein. It may travel to the lungs and form a pulmonary embolus (PE). This can cut off the flow to a portion of the lung or to the entire lung. A PE is a medical emergency and may cause death. Healthcare providers use the term venous thromboembolism (VTE) to describe the two conditions, DVT and PE. They use the term VTE because the two conditions are very closely related. And, because their prevention and treatment are closely related.
Over time, a blood clot can also permanently damage veins. To protect your health, a blood clot must be treated right away.
How DVT develops
The deep veins of the legs are located in the muscles. These help carry blood clot from the legs to the heart. When leg muscles contract and relax, blood is squeezed through the veins back to the heart. One-way valves inside the veins help keep the blood moving in the right direction. When blood moves too slowly or not at all, it can pool in the veins. This makes a clot more likely to form.
Risk factors
Anyone can develop a blood clot. The following risk factors make a blood clot more likely to happen:
Being inactive for a long period, such as when you’re in the hospital, or traveling by plane or car
Injury to a vein from an accident, a broken bone, or surgery
Having blood clots in the past
Personal or family history of a blood-clotting disorder
Recent surgery
Cancer and certain cancer treatments
Smoking
Other factors can also put you at higher risk for a blood clot. They include:
Age over 60 years
Pregnancy
Taking birth control or hormone replacement
Having other vein problems
Being overweight
Common symptoms
A blood clot does not always cause obvious symptoms. If you do have symptoms, they usually happen suddenly. They may include:
Pain, especially deep in the muscle
Swelling
Aching or tenderness
Red or warm skin
Fever
Call your healthcare provider if you have these symptoms.
Symptoms of pulmonary embolism may include:
Trouble breathing
Fast heartbeat
Chest pain
Sweating
Coughing (may cough up blood)
Fainting
Call 911 if you have these symptoms.
If you take medicine to help prevent blood clots, you have an increased risk of bleeding. Call 911 if you have heavy or uncontrolled bleeding. Call your healthcare provider if you have other signs or symptoms of bleeding like blood in the urine, bleeding with bowel movements, or bleeding from the nose, gums, a cut, or vagina.
Diagnosing DVT
Diagnosis begins with thorough questions about your symptoms and medical history along with a physical exam.
Diagnostic tests include:
An imaging test called a duplex ultrasound. This test uses sound waves to create pictures of veins and blood flow.
Blood tests to check for clotting and other problems.
If your healthcare provider thinks you may have pulmonary embolism, additional testing will be done.
Treating DVT
Treating a blood clot may include:
Medicine to thin the blood and prevent pulmonary embolism and other complications.
Staying in the hospital. This may or may not be necessary.
Surgery for some people, like those who cannot take blood-thinning medicines.
Preventing DVT
Many people who are in the hospital are at an increased risk of developing blood clots. So, preventing blood clots is an important part of in-hospital care. The care may include getting out of bed regularly, taking medicine, or using special therapies or devices. Other factors and conditions may increase the risk of blood clots. Review your risk with your healthcare provider.
Updated:
March 29, 2018
Sources:
Guyatt, G. Executive Summary: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest. 2012;141(2):s7-47.
Reviewed By:
Dozier, Tennille, RN, BSN, RDMS,Image reviewed by StayWell medical illustration team.,Mancini, Mary, MD