Tuberculosis (TB)
Tuberculosis (TB)
Tuberculosis (TB) is a serious disease caused by bacteria that spread from person to person through the air. Most often, TB infects the lungs, but it can also affect other parts of the body including the brain, kidneys and spine. When not treated properly, TB can be fatal. Here is more information about TB, how it is treated, and ways to help prevent its spread.
What are the risk factors for TB?
Anyone can get TB, but your risk is greatest if you:
Have an immune system weakened by medicinessuch as steroids or a disease such as HIV infection
Have close contact with someone who has untreated active TB
Are elderly
Live or work in a residential facility, such as a shelter, nursing home, or prison
Travel to or come from a country where TB is common
How does TB spread?
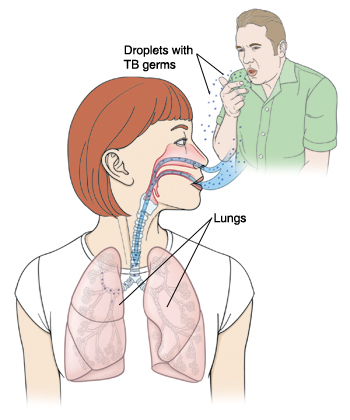
TB germs (bacteria) are released into the air when someone with the active form of TB coughs or sneezes. The bacteria spread easily, especially in crowded places with poor airflow. The longer you breathe these germs, the more likely you are to become infected.
What are the symptoms of TB?
There are 2 types of TB: inactive (also called latent TB infection) and active (also called TB disease).
Inactive TB (latent TB infection)
If you have been diagnosed with inactive TB, it means you:
Have live TB bacteria in your lungs, but the germs have been sealed off, much like a scab covers a wound. As a result, you don’t have symptoms or feel sick. The only way to know you have inactive TB is with a TB test.
Can’t spread the infection to others
May need medicine to keep the infection from becoming active at some future time
Active TB (TB disease)
If you have been diagnosed with active TB, it means you:
Have symptoms of TB such as a lasting cough, tiredness (fatigue), fever, night sweats, and weight loss. You are likely to feel very sick.
Can spread the infection to others.
Must take medicine to help cure the disease. Treatment often takes months. TB can be hard to cure.
How is TB diagnosed?
Two tests can help detect TB infection:
Skin test (PPD). A testing solution is placed just beneath the skin on your arm to see if a reaction (such as a hard, red bump) occurs. You will need to return to the office in 2 or 3 days to have your arm checked. Be sure to keep the appointment. You will learn the test results during this visit.
Blood test. In this test, a small amount of blood is drawn and sent to a lab for testing. Your healthcare provider can tell you if this test is offered in your area.
Other tests. If you have TB infection, other tests, such as a chest X-ray, are needed to learn if the infection is active. Your healthcare provider may also take a sample of your sputum (mucus that comes up when you cough). The sample is sent to a lab and tested for TB bacteria. Knowing the type of bacteria causing your illness helps your provider choose the right medicine to treat the disease.
What do the test results mean?
A negative result usually means that your body is free of TB bacteria.
A positive result means you have been exposed to the germs that cause TB. You may have an inactive or active infection.
How is TB treated?
Both inactive and active TB are treated with medicines. If you have active TB, you may take more medicine for a longer time.
You will likely begin feeling better shortly after starting treatment, but be sure to keep taking all the medicine you have been prescribed. This is the only way to cure the disease. Not taking all the medicine means you won’t get well and can continue to spread TB germs to others.
Sometimes TB is drug-resistant. This means it doesn’t respond to 1 or more of the usual medicines for TB. Resistant TB is harder to cure and is usually managed by a TB specialist.
What is DOT?
During treatment, you may participate in a program called DOT (directly observed therapy). In this program, a nurse or healthcare worker supervises your treatment. This is a standard approach. It makes it easier to manage medicines, watch for any side effects, and make sure the medicines are working. You can also ask a friend or family member to remind you to take your medicine.
During treatment for TB
Make sure to take all the medicine as directed, even when you start feeling better. You will take the medicine for 6 months or longer. Sticking to this schedule takes patience. But stopping treatment early means your symptoms may come back. It may also lead to drug-resistant TB.
Get plenty of rest and eat healthy meals. A nutritious diet full of fresh fruits and vegetables helps the body fight infection.
Check with your healthcare provider before using any over-the-counter medicines that haven’t been prescribed.
If you are taking birth control pills, you may need to use an additional backup method of birth control. Some TB medicines may make the pill less effective.
Limit your activity to avoid fatigue. Plan frequent rest periods.
Keep your medical appointments. You will need to be checked often to make sure that your medicine is working and you are getting better.
How family and friends can help
TB is a serious illness that takes a long time to cure. If you have a family member or friend with TB, you can help by reminding your loved one to:
Take TB medicines at the same time every day (they’re best taken with water, milk, or juice 30 minutes before meals or at bedtime)
Keep all follow-up appointments (you can help by driving or arranging for a ride)
Get plenty of rest
Eat healthy meals
Preventing the spread of TB
If you have active TB, you should:
Ask family, friends, and the people you work with to get tested. Active TB can spread to other people.
Avoid close contact with others until your healthcare provider says it’s OK.
Wash your hands often, especially after coughing.
Use a tissue to cover your mouth when you cough. If you don’t have a tissue, cough into your elbow, not your hand.
Wear a mask, if you have been told to do so, when you go out in public or visit your healthcare provider
Use a plastic bag to throw away old tissues and other supplies.
When to seek medical care
Call your health care provider right away if you have any of the following:
A fever of 100.4°F (38°C) or higher
Increased coughing or coughing up blood
Chest pain or shortness of breath
Worsening or recurring night sweats
Trouble breathing
Also call your healthcare provider if you are taking TB medicine and think you are having side effects. These include skin rash, yellowing of the eyes, or stomach problems.
Updated:
March 21, 2017
Sources:
Nahid, P. Official American Thoracic Society/Centers for Disease Control and Prevention/Infectious Diseases Society of America Clinical Practice Guidelines: Treatment of Drug-Susceptible Tuberculosis. Clinical Infectious Diseases. 2016, pp. 1-49., Tuberculosis Transmission and Control, Up To Date
Reviewed By:
Holloway, Beth Greenblatt, RN, M.Ed.,Lentnek, Arnold, MD