Pericarditis
Pericarditis
What is pericarditis?
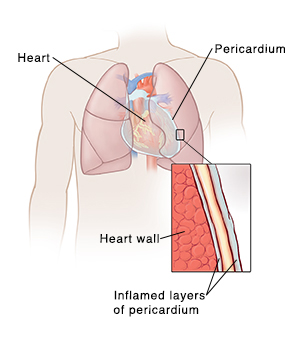
The pericardium helps protect the heart from infection. It consists of 2 thin layers of tissue with a small amount of fluid between them. When these layers become inflamed, they can rub against the heart. This causes chest pain. Pericarditis most often happens after a respiratory infection. It occurs in people of all ages, but is more common in men aged 20 to 50 years.
What are the symptoms of pericarditis?
Pericarditis can be acute or chronic. The acute type occurs suddenly and typically lasts days or up to 3 weeks. The chronic type develops over time and lasts for more than 3 months. Symptoms can vary between the types.
Symptoms of acute pericarditis may include:
Sharp pain in the center or left side of the chest
Fever
Weakness
Trouble breathing
Palpitations
Coughing
Symptoms of chronic pericarditis may include:
Tiredness
Coughing
Shortness of breath
Swelling of the stomach and legs (in severe cases)
Low blood pressure (in severe cases
Chest pain may worsen by lying down or with deep breathing and improved sitting up and leaning forward
What causes pericarditis?
In many cases, the cause of this condition is unknown (called idiopathic pericarditis).The following are possible causes:
Viral infection (common, particularly after a viral respiratory infection)
Bacterial or fungal infection
Autoimmune diseases, such as scleroderma and lupus
Recovery from heart attack
Injury or surgery to the chest, esophagus, or heart
Radiation treatment to the chest
Certain types of cancer
HIV/AIDS
Medicines that suppress the immune system
Kidney failure
How is pericarditis diagnosed?
The doctor will take your medical history and ask you to describe your symptoms. You’ll have a physical exam. Your doctor will listen to your heart to see if it makes certain sounds (pericardial rub) and certain tests may be done. These include:
Electrocardiogram (ECG). This test records the electrical activity of your heart. During an ECG, small sticky pads (electrodes) are placed on your chest, arms, and legs. Wires connect the pads to a machine, which records your heart's electrical signals.
Lab tests. Samples of blood or pericardial fluid may be taken and tested in a lab. These tests can help determine the cause of pericarditis.
Imaging tests of the heart or chest. These may include X-ray, MRI, and CT. They create pictures of the heart or the inside of the chest. An MRI (magnetic resonance imaging) scan uses magnets and radio waves. A CT (computed tomography) scan uses X-rays and a computer.
Echocardiogram (echo). This is usually the main imaging test used for diagnosis. This test creates a moving picture of the heart. During an echo, a probe moved over the chest sends out harmless sound waves. These create a picture that shows the size and shape of the heart. It shows how well the heart is working. It also shows whether fluid has built up around the heart.
Radionuclide scanning (also called nuclear medicine scanning). This test creates a picture showing the structure of the heart. It also shows how well the heart is functioning. A low-level radioactive substance is injected into a vein or taken by mouth. The substance collects in the heart. There, it gives off gamma rays (similar to X-rays). A special camera takes pictures of the gamma rays.
How is pericarditis treated?
Treatment depends on how severe the condition is. Treatment can address the symptoms or the cause of pericarditis. Or it can address complications the condition may cause.
Treatment of symptoms. For minor symptoms, rest may be the only treatment needed. To relieve pain and inflammation, medicine may be prescribed. These include aspirin and ibuprofen. If pain is severe, a strong anti-inflammatory called colchicine may be prescribed.
Treatment of the cause, if known. For instance, antibiotics may be prescribed. This is done if the cause is a bacterial infection.
Treatment of complications. Serious but uncommon complications can result from both acute and chronic pericarditis. These include:
Cardiac tamponade. Fluid builds up within the layers of the pericardium. This can keep the heart from working properly. To treat this condition, a needle is inserted into the chest wall and between the layers of the pericardium. It removes the excess fluid. Sometimes surgery may be done to remove a portion of the pericardium.
Constrictive pericarditis. Over time, scar-like tissue forms in the pericardium. The tissue prevents the heart from expanding enough when it beats. This keeps the heart from working right. Surgery to cut or remove the pericardium is the only treatment.
When should I call my healthcare provider?
Be sure to call your healthcare provider right away if you have any symptoms of pericarditis. This is especially important if you have chest pain. Without treatment, this condition can be life-threatening.
Updated:
March 21, 2017
Sources:
Khandaker, MH. Pericardial Diseases: Diagnosis and Management. Mayo Clinic Proceedings (2010); 85(6); pp. s572-s593, Treatment of acute pericarditis, Up To Date
Reviewed By:
Fraser, Marianne, MSN, RN,Image reviewed by StayWell medical illustration team.,Mancini, Mary, MD