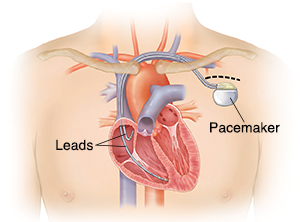
Pacemakers
Pacemakers
A pacemaker is a small electronic device that keeps your heart beating at the right pace. Inserting the pacemaker into your body is called implantation. You stay awake during the procedure. You may be asked some questions or be asked to take some deep breaths.
How do I get ready for a pacemaker procedure?
Don’t eat or drink anything after midnight the night before the procedure, or 8 hours before the procedure.
Tell your doctor about any allergies to medicines, shellfish or iodine contrast, tape or adhesives, or antibiotic types of soaps. Alternatives can be provided and precautions can be taken to avoid exposing you to anything that you are allergic to.
Follow your healthcare provider's instructions on what medicines to take. If you are taking a blood thinning medicines, your healthcare provider may give you instructions on stopping it before the procedure to decrease the risk of major bleeding. You may be instructed to stop medicines that interact with the contrast dye that is used to place the pacemaker wires in the vein.
You may be asked to shower with antibacterial soap the night before your procedure and the morning of the procedure. Ask your provider if he or she wants you to use a certain kind of soap.
Your provider may ask you to use clean bed sheets and pajamas the night before the procedure to reduce the risk of infection.
You may be given an antibiotic through an IV to also protect you from infection after the pacemaker implant procedure.
You will have blood drawn depending on your overall health. If your kidney function is not normal, special precautions may be needed before the procedure.
If you are a woman of child-bearing age you may be asked to take a pregnancy test before the procedure.
What happens during the procedure?
Your doctor may prescribe a medicine to help you relax and to prevent pain during the procedure.
A local anesthetic is given by injection to numb the area where the pacemaker will be inserted. This keeps you from feeling pain during the procedure.
The doctor will make a cut (incision) where the generator is placed.
The doctor will guide the wire (lead) through a vein into your heart’s chambers using X-ray monitors.
The doctor will attach the pacemaker generator to the lead or leads.
The doctor will close the incision site with stitches and may seal the site with a surgical glue to prevent infection.
A dressing may be applied to your incision to reduce the risk of bleeding and also protect it from infection.
The pacemaker’s settings are programmed to help your heart beat at a rate that’s right for you.
What happens after the procedure?
You will have a chest X-ray while you are in the recovery area.
Your pacemaker settings will be rechecked.
Your provider may prescribe antibiotics to take after the procedure to prevent infection.
Follow the instructions you are given for caring for the implantation site. You will likely be told not to raise the arm on that side for a certain amount of time. You may have a sling or arm immobilizer put on to keep you from moving your arm on the incision side. This is done to prevent the new pacemaker wired from becoming displaced. Your doctor will give you instructions on how long and when you should wear this.
Take your temperature and check your incision for signs of infection every day for a week.
Return for a follow-up visit as advised.
As your healthcare provider when it will be safe to shower, bathe, or swim. Generally, you should not soak in water for about a week to prevent the incision from softening, opening, or becoming infected.
Avoid all activities that would put pressure on your incision site or cause irritation to the incision. Do not use lotions, powders, or ointments unless your provider says it is safe to do so. Do not carry a purse or backpack that would put pressure on your incision site.
Call 911
Call 911 if you have:
Chest pain
Severe trouble breathing
When to call your healthcare provider
Call your healthcare provider right away if you have any of the following:
You feel any of the symptoms you had before the pacemaker was implanted. These include dizziness, lightheadedness, lack of energy, or fainting spells.
Your chest or abdominal muscles twitch
You have hiccups that won't stop
You have a rapid or pounding heartbeat or shortness of breath
You feel pain in the area around your pacemaker
You have a fever of 100.4°F (38°C) or higher, or as directed by your healthcare provider
Redness, severe swelling, drainage, bleeding, or warmth at the incision site
Your incision site is not healing or the incision separates or opens
Your pacemaker generator feels loose or like it is wiggling in the pocket under the skin
If you need an MRI for any reason. In some cases, it is not safe to have an MRI with a pacemaker.
Updated:
September 03, 2017
Sources:
Infections Involving Cardiac Implantable Electronic Devices, UpToDate, Pacemakers. UpToDate., Wollmann, CG., Safe performance of magnetic resonance of the heart in patients with magnetic resonance conditional pacemaker systems: the safety issue of the ESTIMATE study, Journal of Cardiac Magnetic Resonance (2014)16(30);1-8
Reviewed By:
Image reviewed by StayWell medical illustration team.,Kang, Steven, MD,Snyde,r, Mandy, APRN