Duodenitis
Duodenitis
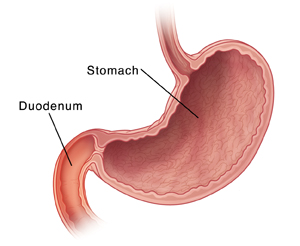
The duodenum is the first part of the small intestine, just past the stomach. Duodenitis is inflammation of the lining of the duodenum. This sheet tells you more about the condition.
Causes of duodenitis
The most common cause of duodenitis is infection by Helicobacter pylori (H. pylori) bacteria. Another common cause is long-term use of NSAIDs (such as aspirin and ibuprofen). Celiac disease, an allergy to gluten, causes a particular type of inflammation in the duodenum along with other changes. Less commonly, duodenitis happens along with another health problem, such as Crohn's disease. Drinking alcohol, smoking, or taking certain medicines also may make duodenitis more likely to happen.
Symptoms of duodenitis
The condition may cause no symptoms. If symptoms do happen, they can include:
Burning, cramping, or hunger-like pain in your stomach
Gas or a bloated feeling
Nausea and vomiting
Feeling full soon after starting a meal
Diagnosing duodenitis
Here is what will be done to diagnose duodenitis:
If duodenitis is suspected, an upper endoscopy with biopsy will be done to confirm it. During this test, a thin, flexible tube with a light and camera on the end (endoscope) is used. The scope is moved down your throat to the stomach and into the duodenum. The scope sends images of the duodenum to a video screen. Small samples (biopsy) of the lining of the duodenum may be taken. These samples may be sent to a lab for testing for H. pylori.
To check for H. pylori or other pathogens, a blood, stool, gastric biopsy, or breath test may be done. Samples of blood or stool are taken and tested in a lab. For a breath test, you swallow a harmless compound. If H. pylori bacteria are present, extra carbon dioxide gas can then be detected in your breath.
To check for celiac disease, blood tests may be done. If positive, an upper endoscopy with biopsy is usually done to confirm the diagnosis.
In rare cases, an upper gastrointestinal (GI) series is done. This gives more information about the digestive tract. This procedure takes X-rays of the upper GI tract from the mouth to the small intestine.
Treating duodenitis
Duodenitis is treated using one or more of the following:
Antibiotic medicines to kill H. pylori
Medicines to reduce the amount of acid the stomach makes
Stopping NSAIDs such as aspirin and ibuprofen. However, if you take aspirin for a medical condition, such as heart disease or stroke, do not stop until you check with your prescribing healthcare provider. If you take NSAIDs for arthritis or pain, check with your healthcare provider about alternatives.
Adopting a gluten-free diet if celiac disease is the cause.
Avoiding alcohol
Stopping smoking
Your healthcare provider can tell you more about what treatments are needed.
Recovery and follow-up
With treatment, most cases of duodenitis clear up completely. In rare cases, duodenitis can be an ongoing (chronic) problem or can develop into a duodenal ulcer. If your symptoms do not improve or if they go away and come back, let your healthcare provider know. In such cases, regular healthcare provider visits and treatments are needed to manage your condition.
When to call the healthcare provider
Call your healthcare provider right away if you have any of the following:
Fever of 100.4°F (38.0°C) or higher, or as advised by your healthcare provider
Nausea or vomiting (vomit may be bloody or look like coffee grounds)
Dark, tarry, or bloody stools
Sudden or severe stomach pain
Pain that does not improve with treatment
Rapid weight loss
Updated:
January 13, 2018
Sources:
Frequent Occurrence of Gastritis and Duodenitis in Patients with Inflammatory Bowel Disease. Sonnenberg A. Inflammatory Bowel Diseases. 2010;17(1):s39-s44.
Reviewed By:
Fraser, Marianne, MSN, RN,Lehrer, Jenifer, MD