Discharge Instructions: When Your Baby Cries
Discharge Instructions: When Your Baby Cries
The way your baby cries can tell you how he or she is feeling. It can also alert you to the baby’s needs. This sheet will help you understand what it means when your baby cries and what you can do to help.
Crying
It’s normal for babies to cry. Sometimes the baby just wants to be held. But if the crying doesn’t stop, look for a cause. Common causes of crying include:
Hunger
Discomfort (such as a wet diaper, clothes that are too tight, feeling too hot or too cold, or gas pains)
A stuffy nose, which can make it hard for the baby to breathe
Stress or overstimulation
Illness
What to do when your baby cries
Crying can be the baby’s way of telling you there’s a problem. The baby trusts you to respond to crying and fix whatever is causing the problem. You already know your baby better than anyone else, although figuring out exactly what’s your baby is telling you may take some guesswork at first. If holding the baby doesn’t help, here are some other things you can try:
Try feeding, in case your baby is hungry. To help prevent gas pains, burp the baby about every 5 minutes while feeding. Also keep the baby’s head higher than the rest of the body while feeding.
Check the baby’s diaper. Change it if needed.
Give your baby a warm bath. Or, hold a damp, warm towel on the baby’s stomach for a little while. This may calm some babies.
Rock or walk with your baby. Motion is soothing. Some parents and babies enjoy using slings or other hands-free baby carriers for this purpose.
Offer your baby a pacifier at naptime or bedtime. Don't attach a string or clip to the pacifier. And don't give the pacifier until you have fully established breastfeeding. Breastfeeding and regular checkups help lower the risk for sudden infant death syndrome (SIDS).
Wrap the baby snugly in a blanket. This is called swaddling. It may help the baby feel safe and secure. (See the box later on this sheet to learn how to swaddle your baby.) Swaddling is common throughout the world but has become controversial. Swaddling can make a baby too hot. More importantly, if the blanket becomes loose or a swaddled baby rolls over, the baby can suffocate. Discuss swaddling your baby with your baby's healthcare provider.
Hold your baby against your bare chest. Skin-to-skin contact can be comforting to the baby.
Never shake your baby. Babies who are shaken can suffer life-long disabilities. If you can't calm your baby, it is OK to put him or her in a safe place and take a short break. Also ask a family member or friend to give you a break from your baby.
If the baby has a stuffy nose, use a bulb syringe to clear it. (Your baby’s healthcare provider can show you how to do this.)
Check for signs of illness, such as fever or diarrhea. If the baby seems sick, call the healthcare provider.
When to call the healthcare provider
Call the healthcare provider if your baby:
Has diarrhea
Has a fever (see Fever and children, below)
Has a fever and looks very ill, is unusually sleepy, or is very fussy
Has a fever and has had a seizure
Fever and children
Always use a digital thermometer to check your child’s temperature. Never use a mercury thermometer.
For infants and toddlers, be sure to use a rectal thermometer correctly. A rectal thermometer may accidentally poke a hole in (perforate) the rectum. It may also pass on germs from the stool. Always follow the product maker’s directions for proper use. If you don’t feel comfortable taking a rectal temperature, use another method. When you talk to your child’s healthcare provider, tell him or her which method you used to take your child’s temperature.
Here are guidelines for fever temperature. Ear temperatures aren’t accurate before 6 months of age. Don’t take an oral temperature until your child is at least 4 years old.
Infant under 3 months old:
Ask your child’s healthcare provider how you should take the temperature.
Rectal or forehead (temporal artery) temperature of 100.4°F (38°C) or higher, or as directed by the provider
Armpit temperature of 99°F (37.2°C) or higher, or as directed by the provider
Child age 3 to 36 months:
Rectal, forehead, or ear temperature of 102°F (38.9°C) or higher, or as directed by the provider
Armpit (axillary) temperature of 101°F (38.3°C) or higher, or as directed by the provider
Child of any age:
Repeated temperature of 104°F (40°C) or higher, or as directed by the provider
Fever that lasts more than 24 hours in a child under 2 years old. Or a fever that lasts for 3 days in a child 2 years or older.
How to swaddle your baby
Wrapping your newborn baby securely in a lightweight blanket (swaddling) may help your baby feel warm and safe. But swaddling may have some risks and needs to be done safely. Don't swaddle babies older than 2 months, because they are old enough to learn other ways to comfort themselves. They are also starting to try to roll onto their side or stomach. Here is one method of swaddling:
Fold a square blanket diagonally to make a triangle. Turn the triangle so the flat base is at the top and the point is at the bottom.
Lay the baby on top of the blanket with the head over the straight base of the triangle and the feet toward the point.
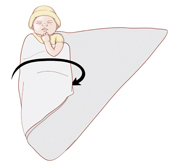
Pull one side of the triangle all the way over the baby’s torso and tuck it under the baby’s body (Figure 1). A baby is most comfortable with the arms folded over the chest. It is best to leave one arm free so the baby can suck on her fingers and learn to calm herself, eventually without needing to be swaddled.
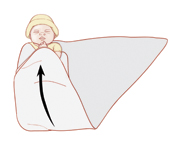
Bring the bottom of the blanket loosely over the baby’s feet and all the way up to the neck (Figure 2). It is very important to keep the baby's feet and legs free to move. Your baby's legs should be able to bend up and out at the hips. Don’t place your baby’s legs so that they are held together and straight down. This raises the risk that the hip joints won’t grow and develop correctly. This can cause a problem called hip dysplasia and dislocation. If your baby has hip dysplasia, don't swaddle.
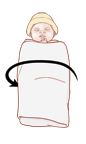
Wrap the other side of the triangle across the baby’s chest (Figure 3).
After your baby is swaddled, check often for the following:
The blanket stays secure. A loose blanket can cover the baby’s face and cause suffocation. But tight blankets may make it hard for babies to breathe, so be sure you can easily insert three fingers between the blanket and the baby's chest.
The baby is lying on his back. Babies lying on their sides or stomachs (or babies who roll onto their sides or stomachs) have a higher risk of SIDS.
The baby is not overheated. This may increase the risk for SIDS. Try to use lightweight blankets or sheets for swaddling.
Figure 1 |
Figure 2 |
Figure 3 |
Updated:
March 21, 2017
Sources:
Epidemiology and Pathogenesis of Developmental Dysplasia of the Hip, UpToDate, Infant Deaths and Injuries Associated with Wearable Blankets, Swaddle Wraps, and Swaddling. E. McDonnel. The Journal of Pediatrics. 2014;164(5):1152-1156., Swaddling and Infant Sleeping Practices. B. Kelly. Journal of Community Health. 2016.
Reviewed By:
Freeborn, Donna, PhD, CNM, FNP,Godsey, Cynthia, MSN, APRN, MSHE, FNP-BC,Lee, Kimberly G., MD, MSc, IBCLC