Open Subclavian Aneurysm Repair
Open Subclavian Aneurysm Repair
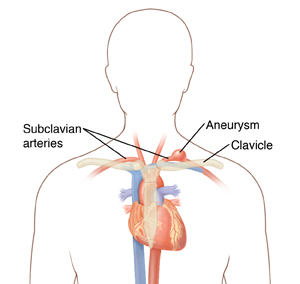
Open subclavian aneurysm repair is a type of surgery. It repairs a subclavian aneurysm through one or more cuts (incisions). The subclavian artery carries blood from your heart to your arms. An aneurysm is a balloon-like bulge in the wall of an artery. It can form when a part of the subclavian artery wall thins and weakens. Over time, the aneurysm can grow so large that it bursts (ruptures). This can cause severe pain and bleeding. Even if the aneurysm doesn’t burst, blood can become trapped inside it and form a clot. The clot can block blood flow to your arm, causing symptoms such as arm or hand pain. If parts of the clot break off and travel to your brain, they can cause a stroke. The aneurysm must be repaired to prevent these problems from happening.
Getting ready for surgery
Follow any instructions from your healthcare provider.
Tell your healthcare provider about any medicines you are taking. You may need to stop taking all or some of these before the procedure. This includes:
Blood-thinning medicines (anticoagulants)
All prescription medicines
Over-the-counter medicines such as aspirin or ibuprofen
Street drugs
Herbs, vitamins, and other supplements
Also tell your healthcare provider if you:
Have any allergies or intolerances to any medicines, including antibiotics
Smoke or drink alcohol on a regular basis
Follow any directions you’re given for not eating or drinking before surgery.
The day of surgery
The surgery takes about 2-4 hours.
Before the surgery begins:
An IV (intravenous) line is put into a vein in your arm or hand. This line gives you fluids and medicines.
To keep you free of pain during the surgery, you’re given general anesthesia. This medicine puts you in a deep sleep through the surgery.
A thin tube (catheter) may be placed into your bladder to drain urine. It may be used through the surgery and for a time afterward.
During the surgery:
One or more cuts (incisions) will be made to repair the aneurysm. Possible incision sites include your neck, chest, and arm.
Nearby muscle or bone (such as a rib) may be removed if it is pressing on the artery and causing symptoms.
Blood thinners are given through the IV line to help prevent blood clots.
The artery is clamped above and below the aneurysm to stop blood flow.
The aneurysm is opened and cleaned of any blood clots.
A substitute blood vessel (graft) is then used to help with the repair. The graft may be a tube made from special fabric. Or it may be tissue taken from your own body. If your own tissue is used, it is usually taken from a vein in your leg.
The graft is sewn to healthy parts of the artery at either end of the aneurysm. The wall of the aneurysm is then sewn over the graft. (In some cases, the part of the artery that has the aneurysm is removed.)
Or, the aneurysm may be tied off at either end. The graft is then sewn into place above and below the aneurysm. This is called a bypass. It moves the blood flow around the part of the artery that has the aneurysm.
When the repair is done, the clamps are removed. This restores blood flow through the artery.
The skin incisions are closed with stitches (sutures) or staples. Small tubes (drains) may be placed near any incisions. These drains remove fluid that can build up after the surgery.
Recovering in the hospital
After the surgery, you may need to stay in the hospital for 3-4 days. While in the hospital:
You may have imaging tests to make sure the graft is working properly.
The tube to drain urine will be removed.
You’ll be given medicines to manage any pain. Let your providers know if you are still in pain.
You’ll be shown ways to cough and breathe that will keep your lungs clear.
When you’re able, you’ll need to stand and walk for short amounts of time. A nurse or therapist will help you.
When it’s time for you to go home, have an adult family member or friend ready to drive you. Also, have someone help you at home for the first few days.
Recovering at home
Once at home, follow any instructions you’ve been given. Be sure to:
Take all medicines as directed.
Care for your incisions as instructed.
Check for signs of infection at any incision sites (see below).
Avoid heavy lifting and strenuous activities as directed.
Walk at least a few times a day. Slowly increase your pace and distance as you feel able.
Don’t drive until your provider says it’s OK. Don’t drive while taking medicines that can make you drowsy or sleepy.
If you smoke, get help to stop smoking. Not smoking lowers your risk of hurting other blood vessels. Your body will also heal better.
Call your healthcare provider if you have any of the following:
New or increased pain in your chest, or trouble breathing
Fever of 100.4°F (38°C) or higher, or as directed by your provider
Return of previous symptoms
Signs of infection at any incision sites, such as increased redness or swelling (inflammation), warmth, more pain, bleeding, or bad-smelling drainage
Pain that gets worse or can't be controlled with medicines
Pain, numbness, or tingling in your arm, hand, or fingers
Rapid, pounding, or irregular heartbeat
Pain or swelling in your legs
Follow-up care
You will have a follow-up visit with your surgical team within 2-3 weeks. This lets your surgical team check how well you’re healing. Any stitches or staples can also be removed, if needed.
Risks and possible complications include:
Bleeding
Infection
Blood clots
Stroke
Problems with the graft. These include the graft moving from its original site, or blood clots at the graft.
Injury to nearby blood vessels, muscles, bones, and organs
Collapse of the lung on the side of the aneurysm. This may require a tube to be placed in your chest for a short period of time to allow the lung to re-expand. The tube will likely be removed before you go home.
Injury to the nerve that leads to your diaphragm. This may cause breathing problems.
Injury to certain nerves that affect your eyes and face, causing Horner’s syndrome. Signs of this condition include partial drooping of the eyelid and a small (constricted) pupil.
Abnormal buildup of fluid around your lungs
Risks of anesthesia
Updated:
March 20, 2017
Sources:
Zhan, Bicheng. Operation for huge subclavian artery aneurysm: a case report. Journal of Thoracic Disease. 2nd ed. 2010: (2), 117-120.
Reviewed By:
Kolbus, Karin, RN, DNP, COHN-S,Image reviewed by StayWell medical illustration team.,Mancini, Mary, MD