Your Child's Gastrostomy Tube: Checking the Balloon
Your Child's Gastrostomy Tube: Checking the Balloon
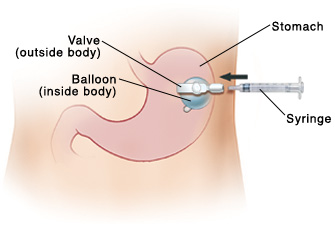
Your child is going home with a gastrostomy tube (G tube) in place. This tube is used to send liquid food directly to your child’s stomach. The tube is placed through the abdominal wall into your child’s stomach. The end of the tube inside the stomach has a small balloon filled with water. This keeps the tube in place. You must check the balloon every 7 days. This is to make sure it holds the amount of water prescribed by your child’s healthcare provider. You were shown how to do this before your child was discharged from the hospital. This sheet will help you remember those steps at home. If you need more help, talk with the hospital about how to arrange a home health nurse to help you.
Keep in mind that there are many types of G tubes and syringes. Your child’s tube and supplies may look or work differently from what are described and shown here. Make sure to follow the instructions given by your child’s healthcare provider or home health nurse.
Contact information to keep handy
Ask for phone numbers to call if you need help. Also, make sure you have the phone number for your child’s medical supply company. You’ll need to order more supplies for your child in the future. Write all of these phone numbers below.
Healthcare provider phone number: ____________________________________
Home health nurse phone number: _____________________________________
Medical supply company phone number: __________________________________
Checking the balloon
Check the balloon every 7 days to make sure it holds the prescribed amount of water.
The supplies you’ll need are:
5 to 10 ml syringe
Water
Follow these steps:
Wash your hands with soap and water.
Make sure the feeding port cap of the tube is closed.
Next to the feeding port is a valve. Connect the empty syringe to this valve.
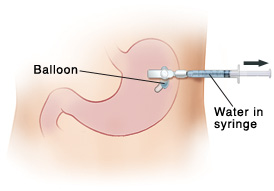
Slowly pull back the plunger of the syringe with one hand, until all the water is removed from the balloon. Be sure to hold the tube in place with your other hand. The tube is more likely to slip away from the body since the balloon no longer has any water to hold the tube in place.
Check the syringe for the amount of water removed from the balloon.
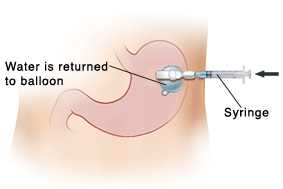
If the water is at the prescribed amount, push the plunger to return the water into the balloon. Disconnect the syringe.
If the water is less than the prescribed amount or appears dirty, see below.
Adding water to the balloon
When you check the balloon, if the water is less than the prescribed amount:
Write down the amount of water that is missing.
Push the plunger to return the water into the balloon.
Disconnect the syringe.
Put the empty syringe into a small bowl of clean water. Pull in the amount of water that is needed to add to the balloon.
Reconnect the syringe to the valve.
Push the plunger to add the water to the balloon.
Replacing the water in the balloon
Always replace the water in the balloon if it’s dirty or cloudy. To do this:
After you draw the balloon water into the syringe, disconnect the syringe from the tube. Then discard the water.
Put the empty syringe into a small bowl of clean water.
Draw the prescribed amount of water with the syringe.
Reconnect the syringe to the valve.
Push the plunger to refill the balloon with water.
Additional instructions
_____________________________________________________________________________
_____________________________________________________________________________
_____________________________________________________________________________
When to call the healthcare provider
Contact the healthcare provider right away if any of the following occurs:
You think that the balloon is damaged.
Your child has trouble breathing.
The tube feels loose or comes out.
The opening where the tube enters the skin becomes larger.
Red, rough tissue forms around the tube site.
The tube becomes clogged or blocked and you can’t clear it.
The skin around the tube site has redness, swelling, leaking fluid, or sores.
You see blood around the tube, in your child’s stool, or in the contents of the stomach.
Your child coughs, chokes, or vomits while feeding.
Your child’s belly looks bloated or feels hard when gently pressed.
Your child has diarrhea or constipation.
Your child has a fever 100.4°F (38°C) or higher.
Updated:
October 08, 2017
Sources:
Bankhead, R. Enteral Nutrition Practice Recommendations. Journal of Parenteral and Enteral Nutrition (2009); 33(2); pp. s122-s167
Reviewed By:
Adler, Liora C., MD,Freeborn, Donna, PhD, CNM, FNP