When Your Child Has Swollen Lymph Nodes
When Your Child Has Swollen Lymph Nodes
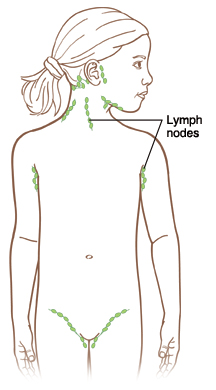
What causes swollen lymph nodes?
Swollen lymph nodes can be caused by:
Common illnesses, such as a cold or an ear infection
Bacterial infections, such as strep throat
Viral infections, such as mononucleosis
Certain rare illnesses that affect the immune system
Rarely, cancer
How is the cause of swollen lymph nodes diagnosed?
The healthcare provider asks about your child’s symptoms and health history.
A physical exam is performed on your child. The healthcare provider will check the nodes in the neck, behind the ears, under the arms, and in the groin. These nodes can often be felt from outside the body when they are swollen. If an infection is suspected, the healthcare provider may order more tests as needed.
How are swollen lymph nodes treated?
Treatment for swollen lymph nodes depends on the underlying cause. In most cases, no treatment is needed at all.
Medicine can be prescribed by the healthcare provider to treat an infection. Your child should take all of the medicine, even if he or she starts feeling better.
If lymph nodes are painful or tender, do the following at home to relieve your child’s symptoms:
Give your child over-the-counter medicine, such as ibuprofen or acetaminophen, to treat pain and fever. Do not give ibuprofen to an infant 6 months of age or less, or to a child who is dehydrated or constantly vomiting. Do not give aspirin to a child. This can put your child at risk of a serious illness called Reye syndrome.
Apply a warm compress to any painful or tender lymph nodes. Use an item such as a warm, clean washcloth. A bottle filled with warm water, or a potato warmed in a microwave and wrapped in a towel, can be used as a compress.
Call the healthcare provider
Contact your healthcare provider if your child has any of the following:
Fever (see Fever and children, below)
Your child has had a seizure caused by the fever
Painful or tender swollen lymph nodes
Lymph nodes that continue to grow in size or persist beyond 2 weeks
A large lymph node that is very hard or doesn't seem to move under your fingers
Fever and children
Always use a digital thermometer to check your child’s temperature. Never use a mercury thermometer.
For infants and toddlers, be sure to use a rectal thermometer correctly. A rectal thermometer may accidentally poke a hole in (perforate) the rectum. It may also pass on germs from the stool. Always follow the product maker’s directions for proper use. If you don’t feel comfortable taking a rectal temperature, use another method. When you talk to your child’s healthcare provider, tell him or her which method you used to take your child’s temperature.
Here are guidelines for fever temperature. Ear temperatures aren’t accurate before 6 months of age. Don’t take an oral temperature until your child is at least 4 years old.
Infant under 3 months old:
Ask your child’s healthcare provider how you should take the temperature.
Rectal or forehead (temporal artery) temperature of 100.4°F (38°C) or higher, or as directed by the provider
Armpit temperature of 99°F (37.2°C) or higher, or as directed by the provider
Child age 3 to 36 months:
Rectal, forehead, or ear temperature of 102°F (38.9°C) or higher, or as directed by the provider
Armpit (axillary) temperature of 101°F (38.3°C) or higher, or as directed by the provider
Child of any age:
Repeated temperature of 104°F (40°C) or higher, or as directed by the provider
Fever that lasts more than 24 hours in a child under 2 years old. Or a fever that lasts for 3 days in a child 2 years or older.
Updated:
April 05, 2018
Reviewed By:
Adler, Liora C., MD,Dozier, Tennille, RN, BSN, RDMS,Turley, Ray, BSN, MSN