When Your Child Has Sickle Cell Anemia
When Your Child Has Sickle Cell Anemia
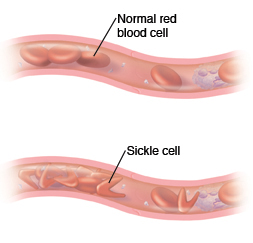
Sickle cell anemia is a problem passed down through genes. It affects the red blood cells (RBCs). RBCs have a protein called hemoglobin that lets them carry oxygen through the body. With sickle cell anemia, a problem with the hemoglobin causes the cells to be C-shaped (like a sickle) instead of round. As a result, the cells can’t move easily through the smallest blood vessels. Because the cells tend to stick together, this can clog the vessels and prevent normal blood flow. Also, sickled cells don’t live as long as normal RBCs. When the body doesn’t have enough healthy RBCs, this causes anemia. Sickle cell anemia is very serious and can hurt your child’s health. Work with your child’s healthcare provider to learn about treatment options for your child.
What causes sickle cell anemia?
Children with sickle cell anemia get one sickle cell gene from each parent. If a child gets a sickle cell gene from one parent and a normal gene from the other parent, it’s called sickle cell trait. Children with sickle cell trait don’t have sickle cell anemia. But they can pass the gene on when they have children. Parents and siblings of a child with sickle cell anemia should also be tested for it. Ask a healthcare provider about genetic counseling.
Sickle cell anemia also affects certain groups of people more often than others. This includes African-American and Central American people and those from the Mediterranean.
Why is sickle cell anemia a problem?
With sickle cell anemia, problems can occur all over the body. These include:
Pain episodes. Pain, ranging from mild to severe, can occur and affect the whole body. This is a sickle cell crisis. When sickle cells get trapped in blood vessels, blood does not flow properly through the body. Organs and tissues may not get enough oxygen and nutrients, causing pain. In some cases, pain lasts for a few hours to a few days. In other cases, it lasts a few weeks or longer. It can even be ongoing.
Damage to spleen. The spleen stores extra blood and helps remove old RBCs from the body. In some kids with sickle cell anemia, sickled cells get trapped in the spleen, causing it to rapidly enlarge. This cuts the number of RBCs that can carry oxygen to the rest of the body. In all children with sickle cell, the spleen will eventually stop working properly.
Infections. All children with sickle cell have spleen damage. So they are at high risk of certain infections that the spleen helps to fight. These include pneumonia and meningitis.
Lung problems. Sickled cells can become trapped in the lungs, too. This can cause chest pain and shortness of breath (acute chest syndrome). Over time, the lungs can be severely damaged, causing other health problems.
Stroke. Sickled cells can block blood vessels leading to the brain or inside the brain, causing stroke.
Other complications. Other problems include painful swelling in the hands and feet, leg ulcers, eye damage, delayed growth, gallstones, or painful and prolonged erections.
What are the symptoms of sickle cell anemia?
Symptoms of sickle cell anemia can range from mild to severe. Most children will have symptoms of anemia such as:
Pale skin
Extreme tiredness (fatigue)
Weakness
Shortness of breath
Rapid heartbeat
Dizziness or fainting
In addition, many children will often have pain with sickle cell crisis. Other symptoms depend on whether your child has other health problems.
How is sickle cell anemia diagnosed?
In most states, hospitals are required to screen all newborns for various health problems including blood disorders such as sickle cell anemia. This is so newborns can be diagnosed before symptoms start.
To confirm the diagnosis, other tests are also done. These can include:
A complete blood cell count (CBC) to measure the amounts of different types of cells in the blood.
A blood smear to check the sizes and shapes of the blood cells for anything abnormal.
Hemoglobin electrophoresis to check for the amounts and different types of hemoglobin in the blood.
How is sickle cell anemia treated?
Your child will be referred to a pediatric hematologist for treatment. This is a doctor who treats blood disorders (hematology). Following are common treatments that may be included in your child’s plan.
Medicines. These are prescribed to help:
Manage pain (pain relievers)
Fight infections (antibiotics and immunizations)
Prevent the sickling of cells (hydroxyurea)
Vitamins. Folate may be prescribed to help the body make more RBCs.
Fluids. Fluid loss (dehydration) can cause the cells to sickle more easily. Children with sickle cell should drink plenty of fluids to prevent dehydration.
Blood transfusions. These are often needed to:
Increase the number of RBCs if anemia is too severe
Release blood trapped in the spleen
Reduce the risk of stroke
Surgery. In rare cases, surgery to remove the spleen or gallbladder may be needed.
Bone marrow transplant. In severe cases, the body can’t make enough healthy blood cells. Treatment replaces diseased bone marrow cells with healthy cells from a matched donor.
What are the long-term concerns?
Sickle cell anemia is a lifelong condition. How your child fares depends on the severity of symptoms and other complications. Some children can be active and independent. Others may need more treatment and supportive care. Work closely with your child’s healthcare provider to learn how to help your child.
Coping with your child’s condition
A positive outlook helps while supporting your child. Counseling can help you and your child deal with any worries or concerns. And seek help from family, friends, community resources, or support groups. Many hospitals have child life programs to help kids cope with their condition. A hospital social worker can also answer questions and refer you to other supportive services, if needed. The more you learn about your child’s condition and its treatments, the more in control you may feel.
Updated:
October 07, 2017
Sources:
Overview of the clinical manifestations of sickle cell disease, Up To Date, Overview of the management and prognosis of sickle cell disease, Up To Date
Reviewed By:
Adler, Liora C., MD,Bass, Pat F. III, MD, MPH,Image reviewed by StayWell medical illustration team.