Brachytherapy for Cancer
Brachytherapy for Cancer
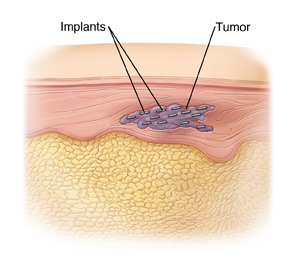
Brachytherapy uses small implants to treat cancer. These implants attack the tumor from inside the body. This treatment can help slow the growth of a tumor. It can also help relieve pain and other symptoms caused by the tumor.
How brachytherapy works
This treatment uses small implants that give off radiation. These implants are also called sources. The sources are placed into the tumor or nearby tissue. Sources give off radiation. With low-dose rate (LDR) brachytherapy, the implants stay in the body for hours or days and then are removed. With high-dose rate (HDR) brachytherapy, the implants stay in the body for several minutes and then are removed. With permanent brachytherapy, implants that give off a low dose of radiation are used. They are not removed. With time, the radiation lessens, then stops completely.
Possible side effects of brachytherapy
Brachytherapy can kill healthy cells in addition to cancer cells. This can lead to side effects, such as fatigue. Many side effects affect only the area where the radiation is given. For instance, if the breast is treated, skin on the breast may become red and dry. Your healthcare provider can tell you more about what side effects you may expect.
Preparing for the procedure
Your healthcare provider will tell you what to do to prepare for the procedure. Follow the directions closely. Tell your healthcare provider about all medicines you take. This includes over-the-counter medicines. It also includes herbs, vitamins, and other supplements. You may need to stop taking some or all of them before the procedure. For example, you may need to stop taking aspirin because it can cause bleeding problems. Also, follow any directions you’re given for not eating or drinking before the procedure.
The procedure
The type of cancer you have, its location, and other factors will determine your treatment schedule. You may go home after treatment. Or you may stay in the hospital for one or more nights.
-
Before the procedure begins: Depending on how the implant is placed, a small tube called an IV may be put into a vein in your arm or hand to give you fluids and medicines. To keep you free of pain during the procedure, you may be given anesthesia. This medicine makes you numb, drowsy, or completely asleep.
-
During the procedure: A device to carry the implant to the proper place is placed into the cancer site. This can be a needle or a small tube. The device may be passed through a nearby opening in the body, such as the vagina or rectum. Or, a small cut (incision) may be made in the skin. Implants are then passed through the device into or near the cancer site. The implants are placed by hand or machine. X-rays, ultrasound, or another imaging test may be used to ensure correct placement.
-
With low dose brachytherapy, the implants and device stay in place for hours to days. You remain in the hospital during this time.
-
With high dose brachytherapy, the implants are put in once a day for several minutes, then removed. The device may be removed after each treatment session. Or it may remain in place. You may go home between treatments. Or you may stay in the hospital until all treatment sessions are done.
-
With permanent brachytherapy, the implants are put in place and not removed. Very low doses of radiation are given, and the radiation stops over time.
-
-
After the procedure: You will recover from the procedure, then go to your hospital room. Or you will be released to go home. If you are able to go home, have an adult family member or friend drive you.
If you go home
Follow any directions you are given for caring for yourself between treatments. These may include:
-
Taking any prescribed medicine exactly as directed.
-
Caring for your bandage and implant site as instructed.
-
If you have a tube left in place, following your healthcare provider’s instructions for taking care of it.
-
Following your healthcare provider’s directions about not putting weight or pressure on the implant site.
-
Following any radiation precautions you are given.
Radiation precautions
Brachytherapy involves doses of radiation. If you are given special precautions by your healthcare team, be sure to follow them closely.
-
With low dose brachytherapy, the implants are removed before you go home. Once they are removed, you are not radioactive and don't pose a danger to others. In most cases, you are not likely to need special precautions.
-
With high dose brachytherapy, the implants are in your body only a short time. But the radiation dose is high. Between treatment sessions, you may be given some precautions to help keep others safe. Follow these closely.
-
With permanent brachytherapy, the implants stay in your body. At first, they give off a very low dose of radiation. This is not likely to affect others. But depending on the type of implant used, you may be told to avoid close contact with small children and pregnant women. Follow your healthcare team’s instructions carefully.
When to call your healthcare provider
Call your healthcare provider if you have any of the following:
-
Fever of 100.4ºF (38ºC) or higher, or as directed by your healthcare provider
-
Trouble concentrating
-
Ongoing fatigue
-
Wheezing, shortness of breath, or trouble breathing
-
Nausea or vomiting
-
Pain that doesn’t go away, especially if it’s always in the same place
-
New or unusual lumps, bumps, or swelling
-
Unusual bleeding
-
Diarrhea that doesn’t improve with time
-
Any other signs or symptoms indicated by your healthcare provider
Checking your progress
During the course of your treatment, you’ll have routine follow-up visits with your healthcare provider. These allow your healthcare provider to check your health and your response to the treatment. After the treatment ends, you and your healthcare provider will discuss your treatment results. You’ll also discuss whether you need additional cancer treatments.
Risks and complications
Risks and complications of brachytherapy for cancer include:
-
Fatigue (tiredness)
-
Discomfort from having to stay in one position
-
Temporary side effects in the area being treated (digestive issues, etc.)
-
Infection
-
Failure to affect tumor growth
-
Damage to healthy tissue and organs
-
Another cancer later on due to radiation exposure
-
Risks of anesthesia
Updated:
March 16, 2019
Sources:
Radiation Therapy Techniques in Cancer Treatment, Up To Date
Reviewed By:
LoCicero, Richard, MD,Sather, Rita, RN