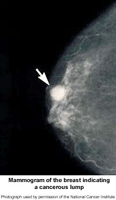
Mammograms and Breast Health
Mammogram
What is a mammogram?
A mammogram is an X-ray image of your breast. It is used to find and diagnose breast disease. A mammogram may be done if you have breast problems such as a lump, pain, or nipple discharge. A mammogram is also done as a screening test if you don’t have breast problems. It can check for breast cancers, noncancerous or benign tumors, and cysts before they can be felt.
A mammogram can’t prove that an abnormal area is cancer. But if a mammogram shows an area in your breast that may be cancer, a sample of breast tissue will be removed. This is called a biopsy. Your provider may remove the tissue by needle or during surgery. The tissue will be checked under a microscope to see if it is cancer.
A mammogram uses a low dose of radiation.
What are the different types of mammograms?
There are 2 types of mammograms:
Screening mammogram. This is used to find any breast changes in women who have no signs of breast cancer. Often 2 X-rays are taken of each breast. A mammogram can find a tumor before it can be felt.
Diagnostic mammogram. This is used to diagnose abnormal breast changes. These may include a lump, pain, nipple thickening or discharge, or a change in breast size or shape. More pictures are taken than during a screening mammogram. A diagnostic mammogram is also used to check any problems found on a screening mammogram.
How is a mammogram done?
X-rays of the breast are different from X-rays for other parts of your body. The breast is squeezed, or compressed, by the mammogram equipment. This spreads the breast tissue apart. Because of this, the radiation dose is lower. You may feel some mild pain when your breast is compressed. But this pressure is needed to keep the radiation level low. It also helps take the best picture of your breast tissue. The compression only lasts for a few seconds for each image of your breast. A breast health nurse or X-ray technologist often takes the X-rays. The films are read by a radiologist. He or she gives the results to your healthcare provider.
Mammograms may also be done with the help of a computer to make digital images. Digital mammograms are done the same way as a standard mammogram.
What conditions does a mammogram show?
A mammogram can show the following conditions:
Calcifications are tiny mineral deposits in the breast tissue. There are 2 types of calcifications:
Macrocalcifications. These are larger calcium deposits that often mean worsening changes in the breast. These changes may include aging of the breast arteries, past injuries, or swelling or inflammation.
Microcalcifications. These are tiny (less than 1/50 of an inch) specks of calcium. When many microcalcifications are seen in 1 area, they are called a cluster.
Masses may happen with or without calcifications. Masses may be caused by:
A cyst. This is a noncancer (benign) collection of fluid in the breast. It can’t be diagnosed by a physical exam alone or by a mammogram alone. A breast ultrasound or aspiration with a needle is needed. If a mass is not a cyst, you may need more tests.
Benign breast conditions. Some masses can be checked with regular mammograms. But for others you may need a biopsy.
Breast cancer
Who should get a screening mammogram?
Different health experts have different recommendations for women who have no symptoms of breast cancer:
The U.S. Preventive Services Task Force recommends screening every 2 years for women ages 50 to 74.
The American Cancer Society recommends screening be an option for women who are at average risk, starting at age 40. Mammograms should be done every year for all women ages 45 to 54. Then you can switch to mammograms every 2 years. Or you have the choice to continue annual mammograms.
Talk with your healthcare provider to find out which screening guidelines are right for you.
If you are at higher risk for breast cancer, talk with your provider about:
Starting screening mammograms earlier
Having additional tests such as a breast ultrasound or MRI
Having mammograms more often
Updated:
June 19, 2018
Reviewed By:
Cunningham, Louise, RN,Foster, Sara, RN, MPH,Horowitz, Diane, MD,Stump-Sutliff, Kim, RN, MSN, AOCNS