Understanding Lumbar Radiculopathy
Understanding Lumbar Radiculopathy
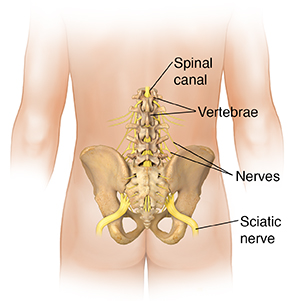
Lumbar radiculopathy is irritation or inflammation of a nerve root in the low back. It causes symptoms that spread out from the back down one or both legs. To understand this condition, it helps to understand the parts of the spine:
-
Vertebrae. These are bones that stack to form the spine. The lumbar spine contains 5 vertebrae near the bottom of your spine.
-
Disks. These are soft pads of tissue between the vertebrae. They act as shock absorbers for the spine.
-
Spinal canal. This is a tunnel formed within the stacked vertebrae. In the lumbar spine, nerves run through this canal.
-
Nerves. These branch off and leave the spinal canal, traveling out to parts of the body. As they leave the spinal canal, nerves pass through openings between the vertebrae. The nerve root is the part of the nerve that is closest to the spinal canal.
-
Sciatic nerve. This is a large nerve formed from several nerve roots in the low back. This nerve extends down the back of the leg to the foot.
With lumbar radiculopathy, nerve roots in the low back become irritated. This leads to pain and symptoms. The sciatic nerve is commonly involved, so the condition is often called sciatica.
What causes lumbar radiculopathy?
Aging, injury, poor posture, extra body weight, and other issues can lead to problems in the low back. These problems may then irritate nerve roots. They include:
-
Damage to a disk in the lumbar spine. The damaged disk may then press on nearby nerve roots.
-
Degeneration from wear and tear, and aging. This can lead to narrowing (stenosis) of the openings between the vertebrae. The narrowed openings press on nerve roots as they leave the spinal canal.
-
Unstable spine. This is when a vertebra slips forward. It can then press on a nerve root.
Other, less common things can put pressure on nerves in the low back. These include diabetes, infection, or a tumor.
Symptoms of lumbar radiculopathy
These include:
-
Pain in the low back
-
Pain, numbness, tingling, or weakness that travels into the buttocks, hip, groin, or leg
-
Muscle spasms in the low back, or leg
Treatment for lumbar radiculopathy
In most cases, your healthcare provider will first try treatments that help relieve symptoms. These may include:
-
Prescription and over-the-counter pain medicines. These help relieve pain, swelling, and irritation.
-
Limits on positions and activities that increase pain. But lying in bed or avoiding all movement is only recommended for a short period of time.
-
Physical therapy, including exercises and stretches. This helps decrease pain and increase movement and function.
-
Steroid shots into the lower back. This may help relieve symptoms for a time.
-
Weight-loss program. If you are overweight, losing extra pounds may help relieve symptoms.
In some cases, you may need surgery to fix the underlying problem. This depends on the cause, the symptoms, and how long the pain has lasted.
Possible complications
Over time, an irritated and inflamed nerve may become damaged. This may lead to long-lasting (permanent) numbness or weakness in your legs and feet. If symptoms change suddenly or get worse, be sure to let your healthcare provider know.
When to call your healthcare provider
Call your healthcare provider right away if you have any of these:
-
New pain or pain that gets worse
-
New or increasing weakness, tingling, or numbness in your leg or foot
-
Problems controlling your bladder or bowel
Updated:
March 03, 2020
Sources:
Ellenberg M, et al. Lumbar Radiculopathy. In: Frontera WR, et al, editors. Essentials of Physical Medicine and Rehabilitation: Musculoskeletal Disorders, Pain, and Rehabilitation. 3 ed. Philadelphia: Elsevier; 2015. p. 237-43., Hsu PS, et al. Acute lumbosacral radiculopathy: Pathophysiology, clinical features, and diagnosis. Up To Date. June 7 ed: Up To Date; 2015. p. 30., Levin K, et al. Acute lumbosacral radiculopathy: Treatment and prognosis. Up To Date. September 15 ed: Up To Date; 2015. p. 10., Manchikanti L, et al. Lumbar Radiculopathy. In: Waldman SD, editor. Pain Management. 2 ed. Philadelphia: Saunders; 2011. p. 707-15., Waldman S. Lumbar Radiculopathy. In: Waldman SD, editor. Atlas of Common Pain Syndromes. Philadelphia: Saunders; 2012. p. 238-41.
Reviewed By:
Raymond Kent Turley BSN MSN RN ,Ronald Karlin MD,Raymond Kent Turley BSN MSN RN