Scoliosis
Scoliosis
What is scoliosis?
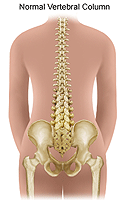
A normal spine, when viewed from behind, appears straight. However, a spine affected by scoliosis shows a side-to-side curvature, with the spine looking like an "S" or "C." The back bones (vertebrae) may also be rotated. This makes it look like the person is leaning to one side. Scoliosis is defined as a curvature of the spine measuring 10° or greater.
Scoliosis is not due to poor posture.
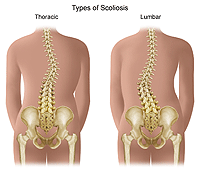
Spinal curvature from scoliosis may occur on the right, left or both sides of the spine. Both the thoracic (mid) and lumbar (lower) spine may be affected by scoliosis.
What causes scoliosis?
In most cases, the cause of scoliosis is unknown — called idiopathic scoliosis. In other cases, scoliosis may develop as a result of breakdown of the spinal discs, as seen with arthritis, osteoporosis, or as a hereditary condition that runs in families.
The abnormal curves of the spine are classified according to their cause, including:
-
Nonstructural scoliosis (also called functional scoliosis). In this condition, a structurally normal spine is curved due to one or more underlying conditions (for example, difference in leg length or an inflammatory condition). This type of scoliosis is generally temporary and is often relieved when the underlying condition is treated.
-
Structural scoliosis. The possible causes of structural scoliosis include:
-
Unknown (idiopathic scoliosis)
-
Disease (for example, neuromuscular, metabolic, connective tissue, or rheumatoid disease)
-
Birth defect
-
Injury
-
Infection
-
Abnormal growth
-
What are the symptoms of scoliosis?
These are the most common symptoms of scoliosis:
-
Difference in shoulder height
-
The head isn't centered with the rest of the body
-
Difference in hip height or position
-
Difference in shoulder blade height or position
-
When standing straight, difference in the way the arms hang beside the body
-
When bending forward, the sides of the back appear different in height
Back pain, leg pain, and changes in bowel and bladder habits are not commonly seen with idiopathic scoliosis. A person who has these types of symptoms needs immediate medical evaluation by a doctor.
The symptoms of scoliosis may look like other spinal conditions or deformities, or may be a result of an injury or infection. Always see your doctor for a diagnosis.
How is scoliosis diagnosed?
In addition to a complete medical history and physical exam, X-rays are the main tool for diagnosing scoliosis. In establishing a diagnosis of scoliosis, the doctor measures the degree of spinal curvature on the X-ray.
The following other tests may be done for nonidiopathic curvatures, atypical curve patterns, or congenital scoliosis:
-
Magnetic resonance imaging (MRI). MRI uses a combination of large magnets and a computer to produce detailed images of organs and structures within the body.
-
Computed tomography (CT) scan. A CT scan uses X-rays and computer technology to make horizontal, or axial, images (often called slices) of the body. A CT scan shows detailed images of any part of the body, including the bones, muscles, fat, and organs. CT scans are more detailed than general X-rays.
Early detection of scoliosis is most important for successful treatment.
How is scoliosis treated?
The goal of treatment is to stop the progression of the curve and prevent deformity. Treatment may include:
-
Observation and repeated exams. This may be needed to determine if the spine is continuing to curve, and are used when a person has a curve less than 25° and is still growing.
-
Bracing. Bracing may be used when the curve measures more than 25° to 30° on an X-ray, but skeletal growth remains. It may also be needed if a person is growing and has a curve between 20° and 29° that isn't improving. The type of brace and the amount of time spent in the brace will depend on the severity of the condition.
-
Surgery. Surgery may be recommended when the curve measures 45° or more on an X-ray and bracing isn't successful in slowing down the progression of the curve when a person is still growing.
There's no scientific evidence to show that other methods for treating scoliosis (for example, chiropractic manipulation, electrical stimulation, nutritional supplementation, and exercise) prevent the progression of the disease.
Updated:
March 16, 2019
Sources:
Reamy, BV., Adolescent Idiopathic Scoliosis: Review and Current Concepts, American Family Physician (2001); 64(1); pp. 111-117
Reviewed By:
Banerjee, Rahul, MD,Dozier, Tennille, RN, BSN, RDMS